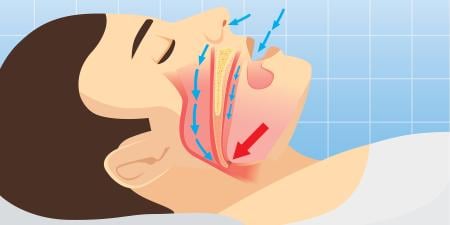
Primary sleep disorders constitute a significant health problem because of their relatively high prevalence and their potential to adversely affect the morbidity, mortality, and quality of life of those who suffer from them. Sleep complaints are also common in the context of many other diseases. The National Center on Sleep Disorders Research estimates that between 50 and 70 million Americans are affected by a sleep-related problem [1]. In the 2008 Sleep in America poll by the National Sleep Foundation, 65 percent of respondents reported having experienced a sleep disturbance at least a few nights a week in the prior month, and 44 percent reported sleep problems occurring every night or almost every night [2]. The most common sleep disorder—obstructive sleep apnea syndrome—which occurs in 2 percent of women and 4 percent of men over 50—h as been linked to conditions such as angina [3], cardiac arrhythmias [4], myocardial infarction [5], stroke [6], and motor vehicle crashes [7]. Importantly, treatments that can improve quality of life and decrease morbidity are available for most sleep disorders.
Given the impact that sleep disorders have on the health and well-being of a significant portion of society, it is remarkable that so little structured, didactic time is given to these topics in the medical school curriculum. This article will examine what is known about sleep medicine and what is taught to medical students and will propose ways of addressing this disparity.
Physicians—regardless of specialty—will inevitably encounter patients with sleep complaints and should have the knowledge and awareness to diagnose them. Unfortunately, despite the common presentation and clinical significance of these conditions, they often go undiagnosed and, consequently, untreated [8, 9]. In the 2005 National Sleep Foundation's Sleep in America poll, 70 percent of respondents reported that their doctor had never asked about their sleep habits or patterns [10].
A likely contributor to physicians' general lack of awareness is the relative paucity of exposure to sleep medicine during medical school. Even when compared to other topics that have been historically underrepresented in the medical school curriculum, such as nutrition and the health benefits of exercise, teaching about sleep is scant.
A national survey of medical school course directors in 1993 found that the average medical school curriculum devoted fewer than 2 hours to sleep and sleep disorders over the four years of medical education [11]. Indeed, 46 percent of the responding medical schools reported allocating no structured didactic time at all to this subject. More than two-thirds of those who responded rated the time dedicated to sleep education as inadequate [11]. In a follow-up survey in 1998, the average number of hours devoted to sleep medicine instruction improved only slightly to 2.1 hours. Seventy-nine percent of respondents reported spending between 0.75 hours and 2.0 hours on the topic. Twelve percent reported spending between 2.5 and 4 hours, and only 9 percent reported providing 6-10 hours of sleep instruction. Respondents indicated that the greatest need was more instruction time, a tall order for an already crowded curriculum [12].
A 2007 review of medical specialty textbooks found that sleep and sleep disorders information made up only about 2 percent of the content [13]. This lack of emphasis has contributed to the medical culture in which few physicians, other than sleep specialists, ask questions about sleep when taking a patient's history [10].
Recognizing Physician Impairment
Aside from preparing future physicians to care more effectively for their patients, more information about sleep should be included in the medical school curriculum because medical students, residents, and physicians are among those at greatest risk for sleep loss due to their educational and professional obligations. Physicians should know enough about the signs and symptoms of sleep deprivation to assess their own performance and professional behavior [14]. The time to learn about managing the sleep loss that they will endure during residency training is during medical school.
The need for change is clear, but implementing it presents several challenges. The modern medical school curriculum must cover a great deal of material in a limited time, so it is unlikely that a block of curriculum time can be dedicated to sleep medicine instruction. A viable alternative approach is to integrate sleep medicine instruction into the existing curriculum [15, 16]. Harding et al. suggest several ways to do so. Their suggestions include: (1) integrating sleep medicine topics into neuroscience, neuroanatomy, physiology, and behavioral science classes and as case studies in problem-based curricula in the preclinical years; (2) including sleep questions in the history-taking portion of physical diagnosis classes; (3) introducing sleep disorders into clinical correlations classes; (4) introducing computer-based simulations for sleep disorders and their symptoms; (5) integrating sleep topics into internal medicine, neurology, and psychiatry rotations during the clinical years as appropriate; and (6) establishing an elective sleep medicine rotation into the fourth year [15]. Harding et al. also emphasize that, for this approach to succeed, the current curriculum, curricular development processes, and availability of educational resources must be assessed [15].
Conclusion
The gap between what we know about sleep and the limited exposure the average medical student has to that knowledge makes the need for more instruction time devoted to this topic clear. Sleep disorders constitute a significant health problem and, if detected, can generally be treated, improving the health and quality of life for these patients. Medical students should also learn about sleep and sleep loss in order to regulate their own sleep effectively while they are students and when they become house staff. The challenges of teaching medical students more sleep medicine can best be met by actively integrating information about sleep and sleep disorders into the existing medical school curriculum. Increasing awareness of sleep disorders among nonspecialists could improve the rate of diagnosis of these treatable disorders.
References
-
National Sleep Disorders Research Plan. Sleep. 2003;26(3):253-257.
-
National Sleep Foundation. 2008 Sleep in America Poll Summary of Findings. Washington, DC: National Sleep Foundation; 2008. Accessed July 21, 2008.
-
Wei K, Bradley TD. Association of obstructive sleep apnea and nocturnal angina [abstract]. Am Rev Respir Dis. 1992;145(4 pt 2):A433.
- Guilleminault C, Connolly SJ, Winkle RA. Cardiac arrhythmias and conduction disturbances during sleep in 400 patients with sleep apnea syndrome. Am J Cardiol. 1985;52(5):490-494.
- Hung J, Whitford EG, Parsons RW, Hillman DR. Association of sleep apnea with myocardial infarction in men. Lancet. 1990;336(8710):261-264.
- Partinen M, Guilleminault C. Daytime sleepiness and vascular morbidity at seven-year follow-up in obstructive sleep apnea patients. Chest. 1990;97(1):27-32.
- Aldrich MS. Automobile accidents in patients with sleep disorders. Sleep. 1989;12(6):487-494.
- Kapur V, Krohl KP, Redline S, Iber C, O'Connnor G, Nieto J. Underdiagnosis of sleep apnea syndrome in U.S. communities. Sleep Breath. 2002;6(2):49-54.
- Rosen RC, Zozula R, Jahn EG, Carson JL. Low rates of recognition of sleep disorders in primary care: comparison of a community-based versus clinical academic setting. Sleep Med. 2001;2(1):47-55.
-
National Sleep Foundation. 2005 Sleep in America Poll Summary of Findings. Washington, DC: National Sleep Foundation; 2005. Accessed July 30, 2008.
- Rosen RC, Rosenkind M, Rosevar C, Cole WE, Dement WC. Physician education in sleep and sleep disorders: a national survey of U.S. medical schools. Sleep. 1993;16(3):249-254.
- Rosen R, Mahowald M, Chesson A, et al. The Taskforce 2000 survey on medical education in sleep and sleep disorders. Sleep. 1998;21(3):235-254.
- Teodorescu MC, Avidan AY, Teodorescu M, et al. Sleep medicine content of major medical textbooks continues to be underrepresented. Sleep Med. 2007;8(3):271-276.
- Papp KK, Miller CM, Strohl KP. Graduate medical training, learning, relationships, and sleep loss. Sleep Med Rev. 2006;10(5):339-345.
- Harding SM, Berner ES. Developing an action plan for integrating sleep topics into the medical school curriculum. Sleep Breath. 2002;6(4):155-160.
-
Gamaldo CE, Salas RE. Sleep medicine education: are medical schools and residency programs napping on the job? Nat Clin Pract Neurol. 2008;4(6):344-345.