Abstract
Supporting people living with dementia in maintaining selfhood, relationships, and well-being requires seeing beyond the common negative focus on disability. Furthermore, prioritizing the person rather than the disease requires rejecting the tragedy discourse, which is the negative lens through which dementia is typically considered. In this paper, we highlight qualitative research on dementia involving people living with dementia as active participants. Recognizing that many people living with dementia remain capable of making decisions that affect their lives, we highlight a research-based approach to support known as “authentic partnerships” that includes people living with dementia as equal partners. We conclude by proposing eight beliefs to mobilize positive change in transcending the tragedy discourse of dementia, thereby opening a space for selfhood, relationships, and well-being.
Introduction
With an estimated 5.4 million people living with Alzheimer’s disease in the United States [1] and almost 50 million worldwide [2], an essential question is the extent to which our society, communities, and health care professionals support people in living well with dementia, rather than focusing exclusively on managing or treating a disease. It is the authors’ contention that the dominant view of dementia is grounded in a “tragedy discourse,” which emphasizes the loss of both ability and identity [3, 4], and that this view directly harms people living with dementia above and beyond the effects of the pathology of any disease. In this paper, we first show that the negative impact of the tragedy discourse can be readily understood by listening to people living with dementia talk about their experiences and by considering how they are commonly characterized in the public sphere. We then show that care partners can promote well-being through including and engaging persons living with dementia in decision making. However, we contend that the dominant frame for understanding dementia, the tragedy discourse, promotes stigma and is used as an inappropriate justification for denying persons with dementia opportunities for autonomy and engagement, thus threatening their well-being.
Perspectives of People Living with Dementia
In 2007 and 2008, the lead author on this paper (PR), on behalf of the Alzheimer’s Association National Office, led a series of town hall meetings designed to listen to, and directly engage with, people diagnosed with dementia. The methods and full results of these listening sessions were reported by the Alzheimer’s Association in its publication, Voices of Alzheimer’s Disease [5]. In the town hall meetings across the US, along with a virtual town hall opportunity online, a total of 301 people living with dementia offered stories of their personal experiences. Each town hall meeting included the same structured discussion questions, inquiring about experiences across the following eight topics: (1) diagnosis, (2) available treatments and medicines, (3) participation in research, (4) loss of independence and coping with changes in function, (5) changes in roles and relationships (personal and professional), (6) safety issues (e.g., driving, so-called “wandering,” and home safety), (7) care and support services, and (8) meaningful activities and social opportunities.
Throughout the town hall meetings, there was surprisingly little discussion of the impact of the disease on personal functioning or abilities. Rather, participants largely focused on poor interactions with physicians during and after the diagnosis process, as well as on the pernicious stigma of the disease and the immediate change in the way they were treated by others in their everyday life postdiagnosis [5]. In other words, participants perceived the social reaction of the medical community and society in general, including friends and family, to dementia as more damaging to their day-to-day well-being than the disease itself. The stigma of being diagnosed and the immediate implications for control and autonomy in everyday decisions (or lack thereof) were of primary concern. In addition, participants expressed the desire to make a difference by advocating for increased awareness of their condition and finding ways to enhance their own quality of life and that of others. Table 1 presents direct quotations from people living with dementia explaining the impact of the disease on their everyday life. The presence of a social impact of dementia beyond the condition’s effects on physical and cognitive function was a resounding theme.
| “When people say ‘dementia’ or ‘Alzheimer’s,’ everybody thinks you’re going to die” (p. 7). |
| “My doctor just kind of let me go, because he was of the belief that there was no treatment. He just kind of cut me loose. ‘You have dementia and there’s nothing that can be done. It’s a progressive illness. Goodbye’” (p. 12). |
| “There is a stigma that goes along with the disease. Many people are worried about sharing the fact openly” (p. 7). |
| “People shy away … like a reaction that might be associated with BO [body odor]” (p. 20). |
| “When I came down with Alzheimer’s, my friends weren’t my friends anymore. They don’t come to talk with me or just to be with me” (p. 21). |
| “People didn’t know how to talk to me even though I was the same person I was five minutes before I told them I had it. They just saw this big A on my forehead. They didn’t look at me as the same person—I was stupid, or couldn’t carry a conversation, or have a single thought of my own, which was very distressing to me” (p. 21). |
| “Something that’s really important is to help people understand the level at which we want to be engaged. We still want to have social activities” (p. 24). |
| “We can do all sorts of things until our voices fail us, and then the people who are coming behind us will continue to speak for us” (p. 27). |
| “Just speak out, because if we don’t speak out now… nobody is going to speak for us later in life” (p. 27). |
Understanding the Tragedy Discourse of Dementia
The ubiquity of negative characterizations of dementia is not unique to the United States but readily evident in a variety of media and research from around the world. Studies demonstrate that the most common portrayals of people living with dementia center on the difficulties and challenges of living with memory loss, which are often represented in an exclusively negative light [3]. One study that analyzed 350 articles in British newspapers, coupled with individual interviews with care partners of people living with dementia, found frequent use of hyperbolic language that catastrophizes the condition, including language such as “tsunami” or “worse than death” [6]. In a separate analysis of the popular images of dementia in Belgian newspapers, movies, documentaries, literature, and health care communications, Van Gorp and Vercruysse [7] note that the dominant frame promotes the belief that people living with dementia have completely lost their identity. These portrayals of dementia highlight the perceived tragedy of the condition and, as noted, constitute the common lens through which dementia is viewed and discussed by both professionals and the public. Hence we contend that the primary view of dementia is one embedded in a tragedy discourse that serves to further stigmatize people living with dementia and to position them as something less than full members of our community due to their (mis-)perceived limitations.
The implications of the tragedy discourse are profound, with potentially negative impacts on people living with dementia across multiple dementia support contexts [8]. We contend that the standards of care for people living with dementia are essentially paternalistic in all settings of service, including community-based services such as support groups, education programs, and information and referral; home care; long-term care settings; and acute care for nondementia conditions of people living with dementia (both inpatient and outpatient). This negative lens is, as we have seen, also internalized by people living with dementia. To ascribe differences based solely on the diagnosis of dementia is what Ronch describes as “dementia-ism” [9], a form of both explicit and implicit bias against people living with dementia that serves to discriminate against them in everyday life (and in all health care settings).
How we view a person or group of people influences how we treat them, which might enable or constrain opportunities for a full and enriching life. In this light, why do some advocacy organizations that exist primarily to serve people living with dementia persist in the promotion of negative stereotypes and images, which further stigmatize people living with dementia as an unintended consequence? As Christine Bryden, an author and advocate who is living with dementia explains, “This stereotype tugs at the heartstrings and loosens the purse strings, so [it] is used in seeking funds for research, support and services. It’s a Catch 22, because [organizations] promote our image as non-persons and make the stigma worse” [10]. Yet tragedy and fear are not needed to raise awareness of dementia, as evidenced by Devlin, MacAskill, and Stead’s study [11], which highlights the need for images of dementia that portray the genuine experience of those living with the disease while steering clear of the use of fear in sensationalized messages.
Characterizations of people living with dementia that diminish their value and potential for self-determination—derived from the tragedy discourse—not only misrepresent the complexities of life with dementia but also serve to compromise fundamental principles of bioethics. While we argue that the impact of the tragedy discourse has implications for each of the four well-known moral principles for bioethics put forward by Beauchamp and Childress [12], the most obvious ethical dilemma relates to restricting personal autonomy. A diagnosis of dementia leads clinicians, family, friends, and the community to take a negative view of the capabilities for decision making and independence of people living with dementia [5]. In our experience working with people living with dementia, we have observed a general assumption being made by the public and professionals that the decision-making capacity of people living with dementia is greatly compromised [13], which might or might not be valid. However, the result of this assumption is a “prescription” for surrogate decision making, or diminished autonomy, in daily life. We believe that autonomy is a basic fundamental right and critical element of a human’s internalized well-being and that it never leaves a person, even if a person faces challenges in expressing it due to dementia. It is the responsibility of clinicians, care partners, and family members to provide the support necessary to ensure that decisions are made in a manner that is aligned with the preferences of a person living with dementia and that the person has the opportunity to contribute to those decisions to the greatest extent possible, even if he or she is severely disabled.
It is our view that a more supportive approach would strive to understand the capabilities of a person diagnosed with dementia through a person-centered assessment that does not include blanket assumptions about his or her limitations, but rather focuses on the person and his or her retainedabilities. This more individualized approach could better serve to promote and support the autonomy of persons living with dementia, enabling them to live well despite their diagnosis and maintaining their right to self-determination and autonomy in everyday decisions.
A Positive Approach to Inclusion
Internationally, reports published by organizations and initiatives, including Alzheimer’s Disease International [14], Dementia Alliance International [15], Partnerships in Dementia Care Alliance [16], and AARP® (formerly the American Association of Retired Persons) [17], demonstrate a growing movement calling for more social and relational understandings of dementia and the transformation of communities to better support people in maintaining well-being, including exercising autonomy to the greatest extent possible. Research demonstrates that people living with dementia retain their selfhood, despite the common assumption that a person’s identity is lost in the presence of cognitive changes [18].
The recognition and acceptance of a persistent sense of self among people living with dementia has implications for the approaches of clinicians and other care partners, including those in long-term care communities, in that it can promote patient- or person-centered care (PCC) [19, 20], which is an important goal of modern medicine. In 2001, a report issued by the Institute of Medicine (now the National Academy of Medicine) included PCC as one of the six essential aims of modern health care [21]. This approach typically calls for the inclusion of the person in all key health care decisions, especially when there is uncertainty regarding effective approaches to care [21]. Despite this emphasis, elders remain less likely to be actively engaged in their own health care [22]. This lack of engagement in decision making is further complicated when a person is living with dementia [23].
However, effective approaches exist to support people living with dementia in being recognized for who they remain as people and to actively engage them in mutually beneficial caring relationships. First, recognizing that identity and selfhood occur in the social context of relationships, researchers have taken PCC a step further to recommend a reciprocal approach to supporting people living with dementia, known as “relationship-centered care” [24]. A basic tenant of this approach is that optimal care and support can only be achieved when all parties involved in the context of care (i.e., the person living with dementia and his or her family and professional care partners) experience a sense of security, continuity, belonging, purpose, achievement, and significance, which provides a framework for relationship-centered care known as the “Senses Framework” [25]. The increased engagement of people living with dementia could extend beyond the health care context through public acceptance of their retained selfhood and the accompanying opportunity for people living with dementia to continue asserting their individual rights, autonomy, and citizenship (i.e., civic and community engagement) [26].
Recognizing a person’s selfhood within the context of decision making is not necessarily synonymous with his or her active engagement, hence the call for “care partnerships,” in which decision making is collaboratively supported to the highest extent possible [27]. Responding to this call, researchers from the University of Waterloo [28] worked in partnership with persons living with dementia to better understand what it takes to work in authentic partnerships across the continuum of dementia care and support. As stated by Dupuis et al. [29], “An ‘authentic partnership’ actively incorporates and values diverse perspectives and includes all key stakeholder voices directly (including [those of] people living with dementia) in decision-making. It involves working with others, not for others.” Drawing on their own partnership experiences and interviews with persons living with dementia and their care partners, they identified three guiding principles and five enablers (see figure 1) that, when supported, help care partners promote empowerment and equality and build collective capacity for shared decision making and social change. The authentic partnerships approach encourages regular collaborative reflection on the principles and enablers of authentic partnerships throughout the partnership process.
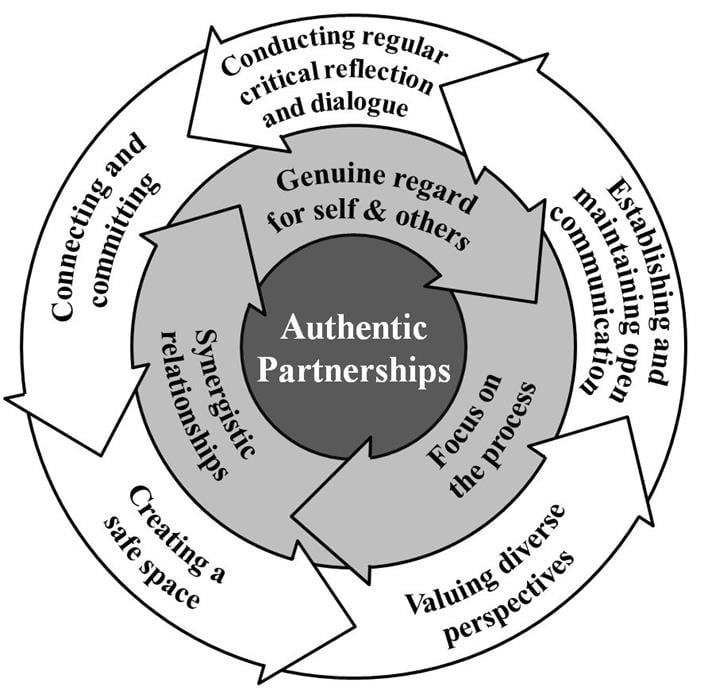
Figure 1. A model of authentic partnerships. From Dupuis SL, Gillies J, Carson J, Whyte C, Genoe R, Loiselle L, Sadler L. Moving beyond patient and client approaches: mobilizing “authentic partnerships” in dementia care, support and services. Dementia (London). 2012;11(4):427-452. Copyright © 2012 by The Author(s). Reprinted by permission of Sage Publications, Ltd.
When care partners work in partnership with persons living with dementia, they do more than just protect personhood; they mobilize social citizenship (meaning preserving the same civic and social rights and opportunities afforded to all citizens) by supporting people living with dementia in making contributions to civic dialogue and activities, and thus new possibilities emerge for living well [27].
Transcending the Tragedy Discourse
To conclude this discussion of the social and health care importance of embracing people living with dementia as valid, autonomous, and engaged partners, we offer eight fundamental beliefs (or principles) to help mobilize opportunities to transcend the tragedy discourse. These “mobilizing beliefs” are not intended as instructions for health care professionals but rather as a type of ethical roadmap for restoring fundamental rights, autonomy, and humanity to people living with dementia who have been disenfranchised by a prevalent view that discounts and diminishes their value and potential contributions. The tragedy discourse not only hinders the potential roles and opportunities of people living with dementia in our communities but also determines the quality of care they receive from health care professionals. Each mobilizing belief is positively framed and offers an aspiration for achieving an alternate lens through which to understand the experience of living with dementia as well as to shape the mindset and actions of professionals and communities (see table 2). Transcending the dominant tragedy discourse of dementia will contribute to an understanding of dementia that is more aligned with respect, dignity, and social justice and in turn will serve to enhance the well-being of the millions of people living with cognitive changes.
| 1. People are living with dementia. |
| 2. Understanding the experience of living with dementia requires understanding the whole person. |
| 3. Focusing on the whole person offers the opportunity to retain identity and assert autonomy and thus supports fundamental human rights. |
| 4. People living with dementia continue to grow and thrive as individuals when care partners avoid the tendency to medicalize, sterilize, and surveil all aspects of everyday life. |
| 5. People living with dementia are the genuine experts in the experience of dementia; their perspectives, wishes, and preferences should always be respected. |
| 6. People living with dementia can and do communicate and express themselves meaningfully. |
| 7. Truly engaging with each person living with dementia as a legitimate contributor to his or her own experience opens a discourse of possibilities. |
| 8. Supporting engagement, autonomy, and partnership with people living with dementia will promote improvements to their quality of life and well-being. |
References
-
Alzheimer’s Association. 2016 Alzheimer’s Disease Facts and Figures. Chicago, IL: Alzheimer’s Association; 2016. https://www.alz.org/documents_custom/2016-facts-and-figures.pdf. Accessed February 2, 2017.
-
Prince M, Wimo A, Guerchet M, Ali GC, Wu YT, Prina M; Alzheimer’s Disease International. World Alzheimer Report 2015: The Global Impact of Dementia: An Analysis of Prevalence, Incidence, Cost and Trends. London, UK: Alzheimer’s Disease International; 2015. http://www.worldalzreport2015.org/downloads/world-alzheimer-report-2015.pdf. Accessed June 1, 2017.
-
Mitchell GJ, Dupuis SL, Kontos PC. Dementia discourse: from imposed suffering to knowing other-wise. J Appl Hermeneutics. 2013;5. http://jah.journalhosting.ucalgary.ca/jah/index.php/jah/article/view/41/pdf. Accessed February 2, 2017.
- Dupuis SL, Kontos PC, Mitchell G, Jonas-Simpson C, Gray J. Re-claiming citizenship through the arts. Dementia. 2016;15(3):358-380.
-
Reed P, Bluethmann S. Voices of Alzheimer’s disease: a summary report on the nationwide town hall meetings for people with early stage dementia. Alzheimer’s Association; 2008. https://www.alz.org/national/documents/report_townhall.pdf. Accessed February 2, 2017.
-
Peel E. “The living death of Alzheimer’s’ versus “Take a walk to keep dementia at bay”: representations of dementia in print media and carer discourse. Sociol Health Illn. 2014;36(6):885.
- Van Gorp B, Vercruysse T. Frames and counter-frames giving meaning to dementia: a framing analysis of media content. Soc Sci Med. 2012;74(8):1274-1281.
- Benbow SM, Jolley D. Dementia: stigma and its effects. Neurodegener Dis Manag. 2012;2(2):165-172.
-
Ronch JL. Viewing and doing in Alzheimer’s disease: mind the gap! http://www.alz.org/maryland/documents/Ronch_Mind_the_Gap.pdf.
-
Bryden C. Nothing about Us without Us: 20 Years of Dementia Advocacy. London, UK: Jessica Kingsley; 2016:138.
- Devlin E, MacAskill S, Stead M. “We’re still the same people”: developing a mass media campaign to raise awareness and challenge the stigma of dementia. Int J Nonprofit Volunt Sect Mark. 2007;12(1):47-58.
-
Beauchamp TL, Childress JF. Principles of Biomedical Ethics. 7th ed. New York, NY: Oxford University Press; 2013.
-
Braun M, Gurrera R, Karel M, Armesto J, Moye J. Are clinicians ever biased in their judgments of the capacity of older adults to make medical decisions? Generations. 2009;33(1):78-91.
-
Alzheimer’s Disease International. Dementia friendly communities: global developments. London, UK: Alzheimer’s Disease International; April 2016. https://www.alz.co.uk/adi/pdf/dfc-developments.pdf. Accessed January30, 2017.
-
Dementia Alliance International. Dementia Alliance International response to WHO global action plan on the public health response to dementia “draft zero”. http://www.dementiaallianceinternational.org/wp-content/uploads/2016/10/DAI-Response-to-the-WHO-Draft-Zero-Global-Action-Plan-on-Dementia_15-October-2016.pdf. Accessed January 30, 2017.
- Dupuis S, McAiney CA, Fortune D, Ploeg J, de Witt L. Theoretical foundations guiding culture change: the work of the Partnerships in Dementia Care Alliance. Dementia (London). 15(1):85-105.
-
Turner N, Morken L. Better together: a comparative analysis of age-friendly and dementia friendly communities. Washington, DC: AARP International Affairs; March 2016. http://www.aarp.org/content/dam/aarp/livable-communities/documents-2016/Better-Together-Summary-Report.pdf. Accessed January 30, 2017.
- Fazio S, Mitchell DB. Persistence of self in individuals with Alzheimer’s disease: evidence from language and visual recognition. Dementia (London). 2009;8(1):39-59.
- Kontos PC. Embodied selfhood in Alzheimer’s disease: rethinking person-centred care. Dementia (London). 2005;4(4):553-570.
- Nowell ZC, Thornton A, Simpson J. The subjective experience of personhood in dementia care settings. Dementia (London). 2011;12(4):394-409.
-
2018;
Institute of Medicine Committee on Quality Health Care in America. Crossing the Quality Chasm: A New Health System for the 21st Century. Washington, DC: National Academy Press; 2001.
- Dewar BJ. Beyond tokenistic involvement of older people in research—a framework for future development and understanding. J Clin Nurs. 2005;14((suppl 1)):48-53.
- Wong JG, Clare CH, Holland AJ, Watson PC, Gunn M. The capacity of people with a “mental disability” to make a health care decision. Psychol Med. 2000;30(2):295-306.
-
Nolan M, Keady J, Aveyard B. Relationship-centred care is the next logical step. Br J Nurs. 2001;10(12):757.
- Ryan T, Nolan M, Reid D, Enderby P. Using the Senses Framework to achieve relationship-centred dementia care services. Dementia (London). 2008;7(1):71-93.
- Brannelly T. Citizenship and people living with dementia: a case for the ethics of care. Dementia (London). 2016;15(3):304-314.
-
Bartlett R, O’Connor D. Broadening the Dementia Debate: Towards Social Citizenship. Bristol, UK: Policy Press; 2010.
- Dupuis SL, Gillies J, Carson J, et al. Moving beyond patient and client approaches: mobilizing “authentic partnerships” in dementia care, support and services. Dementia (London). 2012;11(4):427-452.
-
Dupuis, Gillies, Carson, et al., 436.




