The patient with alcoholic liver disease poses complex medical and ethical challenges. This patient requires not only an understanding of the medical effects of alcohol on the liver but also an appreciation of the psychosocial aspects of alcohol use disorders. Without a doubt, the most critical aspect of treatment for such patients is to help them stop drinking.
Alcohol Use Disorders
The fourth edition of the American Psychiatric Association's Diagnostic and Statistical Manual of Mental Disorders (DSM-IV) distinguishes between alcohol dependence and alcohol abuse.1 Abuse is a destructive pattern of alcohol use, leading to significant social, occupational, or medical impairment.1 Patients with alcohol dependence demonstrate tolerance (either the need for increased amounts of alcohol to achieve intoxication or diminished effects with use of the same quantity) and withdrawal symptoms, including delirium tremens (DTs) and alcohol withdrawal seizures.1 Alcohol-dependent persons may also consume alcohol to avoid or relieve withdrawal symptoms. Patients with alcohol use disorders often continue to consume alcohol despite knowing that they suffer from alcohol-related medical problems. This is often true for patients with alcoholic liver disease.
Effects of Alcohol on the Liver
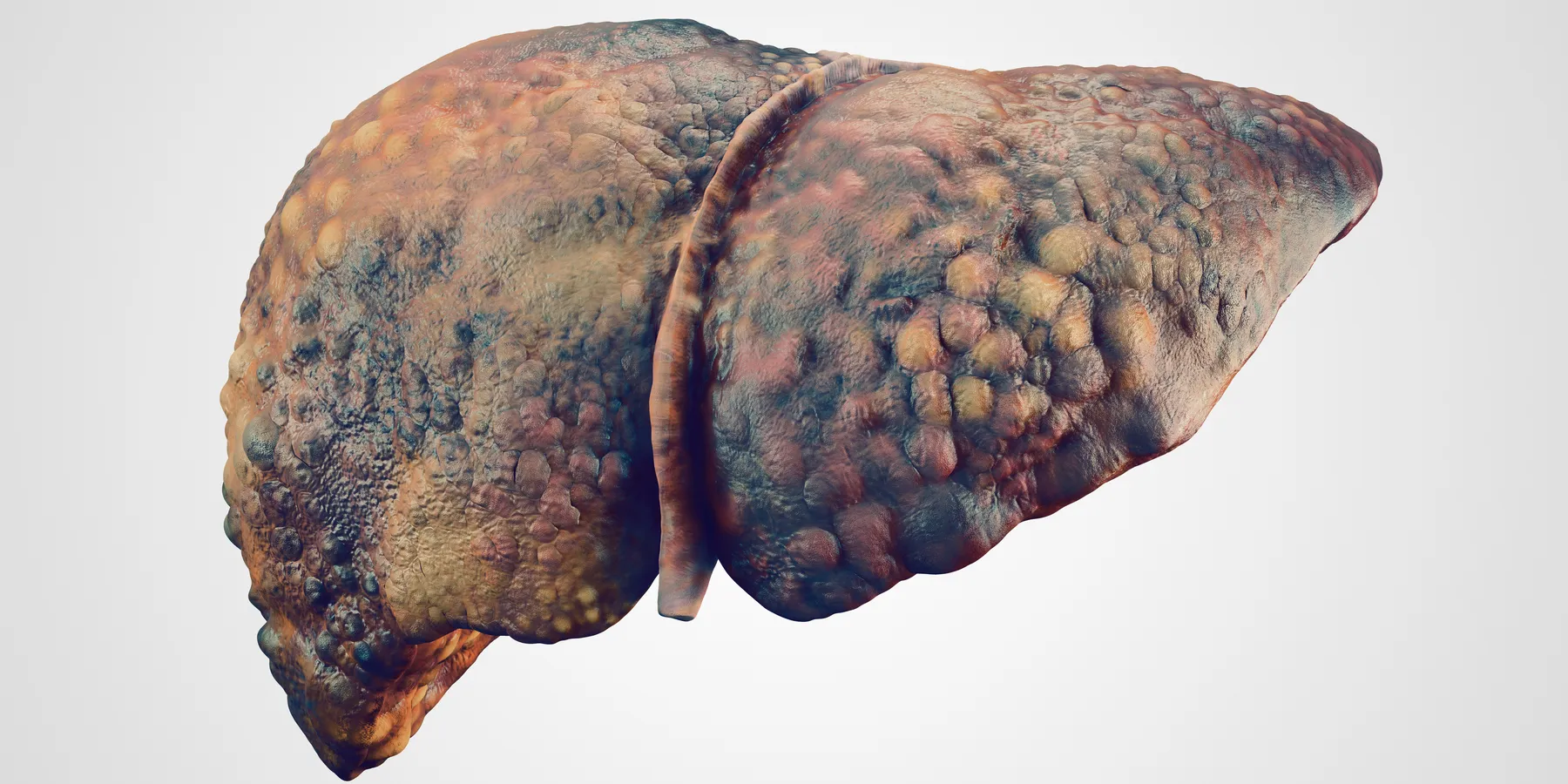
Alcohol affects many organ systems, most notably the central nervous system and the liver. Excessive alcohol consumption frequently leads to 3 pathological liver disorders, any or all of which can occur singly or simultaneously in the same patient. One type of liver disorder is steatosis, which is the accumulation of fat within hepatocytes, a condition that is reversible if the patient stops drinking. A second condition is hepatitis. Histologically, alcoholic hepatitis is characterized by the ballooning degeneration of hepatocytes, inflammation with neutrophils, and, sometimes, the presence of Mallory bodies, which are abnormal aggregations of intermediate filament and other proteins. Alcoholic hepatitis is also reversible if the patient stops drinking, but it can take months to fully resolve. Cirrhosis is the third type of liver disorder. It is irreversible and is a consequence of long-term excessive alcohol consumption. The anatomic features are widespread nodules combined with fibrosis; alcoholic cirrhosis is almost always micronodular (Laënnec's cirrhosis). Patients with cirrhosis can develop end-stage liver disease with complications such as jaundice, ascites, edema, bleeding esophageal varices, abnormal blood coagulation, hepatic encephalopathy, and coma. Cirrhosis also increases the risk of developing hepatocellular carcinoma.
Cirrhosis is currently the tenth leading cause of death in the United States, and alcohol is the cause or a contributing factor in the majority of cases. Despite its high prevalence, only a minority of heavy alcohol drinkers actually develop this liver disease. Estimates have varied across numerous studies, but it appears that only between 10 and 20 percent of those who consume excessive quantities of alcohol over decades develop cirrhosis.2,3,4 It should be noted, however, that environmental factors, such as chronic hepatitis C infection, increase the risk of the development of cirrhosis in an alcoholic. Other factors that may make one more susceptible to cirrhosis are: nutrition, gender (generally, women who drink an equal amount of alcohol are at higher risk than men), and genetic factors, although vulnerable genes or patterns of gene expression have not been identified.
Diagnosis and Treatment
The patient with alcoholic liver disease can present in many different ways. Every internist remembers his or her nights on call as an intern, taking care of a patient with severe alcoholic hepatitis, DTs, and alcohol withdrawal seizures. In these cases, the diagnosis of alcoholic hepatitis is obvious. While many such patients also have cirrhosis, the degree of irreversible liver dysfunction may not be clear until the patient has stopped drinking for several months. Alcoholic hepatitis can cause signs and symptoms of hepatic dysfunction, including jaundice, encephalopathy, and bleeding esophageal varices. Acute treatment of hospitalized patients with alcoholic hepatitis also involves treating the complications of the disease (eg, lactulose for hepatic encephalopathy, antibiotics for infections, and endoscopic procedures for bleeding esophageal varices). More immediate treatment for alcohol use disorders also includes stopping or preventing DTs or seizures (usually with benzodiazepines), nutritional support (eg, with thiamine), and assuring cessation of alcohol intake. When medically stable, patients hospitalized for alcoholic liver disease should be discharged to an inpatient rehabilitation program with plans for subsequent outpatient follow-up and social and psychiatric support. If signs of liver disease remain even after months of abstinence, cirrhosis is likely present. Cirrhosis can sometimes be diagnosed by the clinical picture and radiological or nuclear medicine tests, but a liver biopsy may be necessary to make the definitive diagnosis.
Many subjects with alcoholic liver disease, even cirrhosis, initially present as outpatients and often for other reasons. A majority will not be the typical "skid row" alcoholic but individuals who have managed to hold good jobs and function highly in society. These patients may have none or only a few clinical signs of liver disease. For example, some might have laboratory abnormalities such as elevated serum aminotransferase activities (often aspartate aminotransferase but not always more elevated than alanine aminotransferase), elevated serum bilirubin concentration, thrombocytopenia, hypoalbuminemia, and a prolonged prothrombin time. Intensive questioning about past and current alcohol consumption is critical when taking a history of any subject with liver disease. A liver biopsy may also reveal steatosis, alcoholic hepatitis, or other liver disorders.
Long-term survival of a patient with alcoholic liver disease depends upon his or her commitment to abstinence.5,6 Liver disease is not the only potentially life-threatening issue in patients with alcohol use disorders, and abstinence will also impact favorably on other medical, social, and psychological problems. Participation in Alcoholics Anonymous or a similar support network is a vital component of long-term treatment and likely to improve outcomes.7,8 Family members and friends may also benefit from participation in a support group. Liver transplantation for patients with severe alcohol use disorders and end-stage liver disease is a controversial topic. The generally accepted policy is that alcoholics who are abstinent for 6 months or more are potential candidates for transplantation.9,10 However, concurrent medical or social problems may prohibit transplantation.
References
-
American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. 4th ed. Washington, DC: American Psychiatric Association; 1994.
-
Klatskin G. Alcohol and its relation to liver damage. Gastroenterology. 1961;41:443-451.
-
Morgan MY. The prognosis and outcome of alcoholic liver disease. Alcohol Alcohol Suppl. 1994;2:335-343.
- Mandayam S, Jamal MM, Morgan TR. Epidemiology of alcoholic liver disease. Semin Liver Dis. 2004;24(3):217-232.
- Saunders JB, Walters JR, Davies AP, Paton A. A 20-year prospective study of cirrhosis. BMJ (Clin Res Ed). 1981;282263-266.
- Bullock KD, Reed RJ, Grant I. Reduced mortality risk in alcoholics who achieve long-term abstinence. JAMA. 1992;267(5):668-672.
- Mann RE, Smart RG, Anglin L, Adlaf EM. Reductions in cirrhosis deaths in the United States: associations with per capita consumption and AA membership. J Stud Alcohol. 1991;52(4):361-365.
-
Smart RG, Mann RE. Are increases in treatment levels and Alcoholics Anonymous membership large enough to reduce liver cirrhosis rates? Br J Addict. 1990;85(10):1291-1298.
- Lim JK, Keeffe EB. Liver transplantation for alcoholic liver disease: current concepts and length of sobriety. Liver Transpl. 2004;10(10 Suppl 2):S31-S38.
- Zetterman RK. Liver transplantation for alcoholic liver disease. Clin Liver Dis. 2005;9(1):171-181.