Abstract
Context: Pediatric burn patients warrant thorough evaluation because a sizeable proportion of pediatric burns are nonaccidental.
Design: A multidisciplinary method involving an internal child protection team (CPT) was developed and used to identify suspected nonaccidental pediatric burns in all pediatric burn patients 5 years of age or younger who were evaluated by the CPT and social workers at our institution over a 55-month period.
Results: We identified 343 cases for review that fit our age criteria, 6 of which we identified as cases of suspected abuse or neglect. On average, these patients were younger, suffered greater total body surface area burns, and required a longer length of stay in the hospital than the total population. We have not had readmissions for repeat nonaccidental pediatric burn injuries in this group of patients since this model was implemented.
Conclusions: Our multidisciplinary method might provide a more consistent and reliable method for identifying cases of suspected abuse.
Nonaccidental Pediatric Burns
In the pediatric population, it has been suggested that up to 20% of burns are nonaccidental.1-9 A variety of strategies have previously been described to identify instances of abuse or neglect that have already occurred in an effort to mitigate this problem. These include practitioner education and reliance on pattern recognition, protocols, algorithms, and assessment by a multidisciplinary team.10-12 As stated by one child safety board in the United Kingdom (UK), “there are no simple formulae for recognizing abuse,” and, unfortunately, the methods noted above have the potential to miss instances of abuse or neglect.10 It is critical to properly identify and address all such cases of nonaccidental pediatric burns. We developed a reliable, inclusive, multidisciplinary model for this purpose involving an internal child protection team (CPT), which might improve patient safety after discharge. Here we discuss our findings and provide a description of our approach to reviewing case of pediatric burns, including the CPT.
Methods
Data sources and inclusion criteria. We conducted a thorough review of the literature regarding pediatric burns secondary to abuse or neglect with a particular focus on their identification and management. After receiving Virginia Commonwealth University (VCU) institutional review board approval, we identified patients five years of age or younger who were admitted to our medical center with burn injuries. We collected data over a 55-month period from January 1, 2010 to July 31, 2014 for all pediatric burn patients evaluated by the CPT and social workers. The information collected included age, race, place where the injury occurred, mechanism of injury, total body surface area (TBSA) involved, region of the body that was injured, and hospital length of stay (reported in days).
Method for identifying nonaccidental pediatric burns. We approach pediatric burns using the model depicted in figure 1. The CPT is a hospital-based group founded in 1992 to address situations of suspected child abuse and neglect. It is composed of a medical director, who is board-certified in child abuse and neglect through the American Board of Pediatrics; nurse practitioners certified in pediatrics; and a coordinator. The team provides a number of services, including an inpatient consult service for child physical abuse, sexual abuse, and neglect cases; 24/7 emergency department coverage; and an outpatient clinic for referrals from physicians, child protective services (CPS), and law enforcement. The CPT works closely with the burn surgery team to evaluate pediatric patients for possible abusive or unsafe environments. The model was developed based on national statistics, which have shown that the risk of nonaccidental burns is greater in children under five years of age.7-9,13,14 Therefore, the CPT evaluates all burned children five years of age and under. A social worker also sees children over the age of five years; in these cases, CPT involvement is at the discretion of the burn surgery team. In the event of suspected abuse or neglect, social work acts as a liaison to CPS to arrange outpatient family assessment and follow up.
Figure 1. Approach to Pediatric Burn Patients Using the CPT
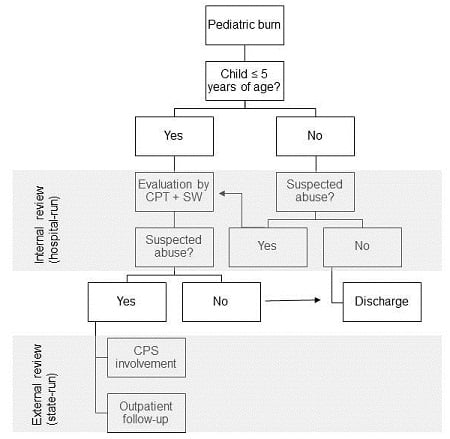
CPT indicates child protection team; CPS, child protective services; SW, social worker.
Results
Between January 1, 2010 and July 31, 2014, the Evans-Haynes Burn Center at Virginia Commonwealth University Medical Center cared for 343 children 5 years of age or younger. The majority of injuries occurred in the home setting, with scalds, followed by contact burns, representing the most common mechanism of injury. The extremities were most likely to be effected. Hospital length of stay (LOS) ranged from 1 to 51 days with an average stay of approximately 5 days. There were 6 cases of suspected abuse (2%), with 2 of these patients being discharged to alternative locations (ie, foster care). The average age of suspected abuse cases was 1.9 years as compared to an average age of 2.11 years in the total population, corroborating that younger children are more likely to be victims of abuse. The proportion of scald injuries was similar in abuse cases and in the total population (50% vs. 57.7%, respectively), suggesting that these factors cannot reliably be used to identify nonaccidental burns, although nonaccidental cases were more likely to have involvement of the perineum. However, injuries tended to be more severe in abuse cases than in the total population. The TBSA burned ranged from less than 0% (inhalation injury) to 30%, with an average of 8% in children with suspected abuse and an average of 2.9% in the total population. Moreover, the average LOS was 15.6 days for suspected abuse cases as compared to 4.6 days for the total population. While LOS was increased by CPT involvement and investigation, the findings also suggests that nonaccidental burns might be more severe and require more extensive care. Results are detailed in table 1. Since this model has been in effect, we have not had readmissions for repeat nonaccidental pediatric burn injuries.
| Variable | Total Patient Population (N = 343) |
Suspected Abuse Cases (n = 6) |
| Average age in years | 2.11 | 1.90 |
| Race, No. (%) | ||
|---|---|---|
| African American | 165 (48.1) | 3 (50) |
| White | 113 (32.9) | 2 (33.3) |
| Hispanic | 28 (8.2) | 1 (16.7) |
| Asian | 6 (1.8) | 0 (0) |
| Othera | 31 (9.0) | 0 (0) |
| Place Injured, No. (%) | ||
| Home | 325 (94.8) | 6 (100) |
| Non-home | 18 (5.2) | 0 (0) |
| Mechanism, No. (%) | ||
| Scald | 198 (57.7) | 3 (50) |
| Contact | 101 (29.5) | 1 (16.7) |
| Flash | 14 (4.1) | 0 (0) |
| Electrical | 12 (3.5) | 0 (0) |
| Other | 18 (5.2) | 2 (33.3) |
| TBSA (%) | ||
| Average | 2.9 | 8.0 |
| Range | 0-40.7 | 0-30.0 |
| Region burned, No. (%) | ||
| Head and neck | 97 (28.3) | 0 (0) |
| Trunk | 123 (35.9) | 0 (0) |
| Perineum | 19 (5.5) | 2 (33.3) |
| Extremities | 271 (79.0) | 5 (83.3) |
| Length of stay in days | ||
| Average | 4.6 | 15.6 |
| Range | 1-51 | 1-29 |
| a Includes chemical, radiation, conflagration, and degloving. | ||
Discussion
Nonaccidental burns in the pediatric population are a significant problem that might lead to recurrent, life-threatening injuries to the patient and financial strain on society.3,15,16 For instance, burns by abuse are associated with a longer LOS, as corroborated by our study, with one source citing an average of 18 days, and typically require more surgical intervention (eg, grafting) than nonaccidental burns.2,3,8,9,12
Recognizing characteristics that distinguish nonaccidental from accidental burns, such as burn type, depth, and distribution, can be a helpful tool for health care workers evaluating pediatric patients. Although scald injuries from contact with hot liquids are the most commonly seen burns in the pediatric population and are typically the most common mechanism of burn abuse or neglect,4,7,12,13,17-19 in our study they were not a distinguishing feature. The average TBSA for patients with suspected abuse in 3 previous studies was somewhat higher than in this study (13%-15% vs. 8%); however, the correlation between TBSA and abuse/neglect in these studies was inconsistent.7,9,12 Several authors have identified additional patient characteristics for burns by abuse or neglect: single parent family, parental drug abuse, family instability, younger patient age, and delay of presentation.1,4,5,7,9,15
In our study there were no nonaccidental pediatric burn injuries readmissions, in contrast to previous studies. Hight et al. demonstrated that 15 of 40 burn patients were readmissions after sustaining previous nonaccidental burn- and nonburn-related injuries.7 This finding was corroborated by Andronicus et al., who noted that 46% of children with nonaccidental burns were victims of previous abuse.1 After finding that 31% of nonaccidental pediatric burn patients had documented prior abuse/neglect encounters in the health care system, Rosenberg and Marino emphasized the importance of closely reviewing a child’s medical record.5 As mentioned earlier, others have described approaches to identifying instances of abuse and neglect using multidisciplinary teams, home assessments, algorithms, and practitioner education.10-12Unfortunately, while these methods can improve detection, they are not 100% sensitive, and potentially abusive situations might go undetected. Given our 0% readmission rate, we believe our unique method for detection and prevention of abuse using the CPT is reliable and improves the safety and quality of care for children under 5 years of age who have nonaccidental burns.
Nevertheless, our rate of detected, nonaccidental pediatric burns was 1.7%, which is considerably lower than the rate of 16% reported by Hight et al.,7thus drawing into question the strength of our model. However, our study is limited by a small sample size, with insufficient numbers to perform formal statistical analyses. Additionally, the model described only evaluates children 5 years old and younger unless a treating clinician has a compelling concern about an older child. There is therefore a possibility that older children who are victims of abuse might not be recognized.
Another limitation of the study is that the model requires additional staff resources (social workers, nurse practitioners, physician support) and time, which might contribute to health care expenditures. Future studies should analyze the cost effectiveness of our model on the hypothesis that it reduces patient morbidity and mortality from readmissions and might ultimately be a cost-saving measure.
Benjamin Franklin’s old adage, “an ounce of prevention is worth a pound of cure,” is particularly relevant in instances of nonaccidental pediatric burns. Toon et al. note that the best way to reduce the burden of nonaccidental burns is by prevention.20 Prevention efforts currently include community outreach as well as clinician education. Detecting abusive situations while a patient is in the hospital is critical. We encourage trauma and burn centers nationwide to implement a model that evaluates all pediatric burns using a multidisciplinary team.
References
- Andronicus M, Oates RK, Peat J, Spalding S, Martin H. Non-accidental burns in children. Burns. 1998;24(6):552-558.
- Hummel RP III, Greenhalgh DG, Barthel PP, et al. Outcome and socioeconomic aspects of suspected child abuse scald burns. J Burn Care Rehabil. 1993;14(1):121-126.
- Purdue GF, Hunt JL, Prescott PR. Child abuse by burning—an index of suspicion. J Trauma. 1988;28(2):221-224.
-
Chester DL, Jose RM, Aldlyami E, King H, Moiemen NS. Non-accidental burns in children—are we neglecting neglect? Burns. 2006;32(2):222-228.
- Rosenberg NM, Marino D. Frequency of suspected abuse/neglect in burn patients. Pediatr Emerg Care. 1989;5(4):219-221.
- Mathangi Ramakrishnan K, Mathivanan Y, Sankar J. Profile of children abused by burning. Ann Burns Fire Disasters. 2010;23(1):9-12.
- Hight DW, Bakalar HR, Lloyd JR. Inflicted burns in children. Recognition and treatment. JAMA. 1979;242(6):517-520.
- Dissanaike S, Wishnew J, Rahimi M, Zhang Y, Hester C, Griswold J. Burns as child abuse: risk factors and legal issues in West Texas and Eastern New Mexico. J Burn Care Res. 2010;31(1):176-183.
- Thombs BD. Patient and injury characteristics, mortality risk, and length of stay related to child abuse by burning: evidence from a national sample of 15,802 pediatric admissions. Ann Surg. 2008;247(3):519-523.
-
Leeds Safeguarding Children Board. Burns and scalds: multi-agency protocol for the assessment of suspected neglectful or inflicted burn and scald injury. Version 2. https://www.leedslscb.org.uk/LSCB/media/Images/pdfs/Burns-and-Scalds-v2dec-17-final.pdf. Published December 15, 2017. Accessed January 22, 2018.
- Peck MD, Priolo-Kapel D. Child abuse by burning: a review of the literature and an algorithm for medical investigations. J Trauma. 2002;53(5):1013-1022.
- Weimer CL, Goldfarb IW, Slater H. Multidisciplinary approach to working with burn victims of child abuse. J Burn Care Rehabil. 1988;9(1):79-82.
- Spinks A, Wasiak J, Cleland H, Beben N, Macpherson AK. Ten-year epidemiological study of pediatric burns in Canada. J Burn Care Res. 2008;29(3):482-488.
- McGuire L, Martin KD, Leventhal JM. Child abuse consultations initiated by child protective services: the role of expert opinions. Acad Pediatr. 2011;11(6):467-473.
- Evasovich M, Klein R, Muakkassa F, Weekley R. The economic effect of child abuse in the burn unit. Burns. 1998;24(7):642-645.
- Klein MB, Hollingworth W, Rivara FP, et al. Hospital costs associated with pediatric burn injury. J Burn Care Res. 2008;29(4):632-637.
- Stratman E, Melski J. Scald abuse. Arch Dermatol. 2002;138(3):318-320.
- Lorch M, Goldberg J, Wright J, Burd RS, Ryan LM. Epidemiology and disposition of burn injuries among infants presenting to a tertiary-care pediatric emergency department. Pediatr Emerg Care. 2011;27(11):1022-1026.
- Shah A, Suresh S, Thomas R, Smith S. Epidemiology and profile of pediatric burns in a large referral center. Clin Pediatr (Phila). 2011;50(5):391-395.
- Toon MH, Maybauer DM, Arceneaux LL, et al. Children with burn injuries—assessment of trauma, neglect, violence and abuse. J Inj Violence Res. 2011;3(2):98-110.




