Abstract
The pathologist rarely interacts with patients face-to-face, but he or she nonetheless maintains a crucial relationship with the patient (i.e., the patient-pathologist relationship). A more tangible relationship, the pathologist-clinician relationship, is typically augmented by the patient-pathologist relationship, but at times the two distinct relationships are at odds, creating ethical dilemmas for the pathologist. This case study and discussion highlight some of these potential ethical questions and underscore the need for pathologists and clinicians to have cooperative, collaborative, and professional relationships. Pathologists should feel empowered to guide the clinician’s use of appropriate clinical testing to ensure proper management of the patient and responsible use of health care resources.
Case
Dr. B is in the process of executing a retroperitoneal soft tissue mass biopsy. Midway through, she gets a call from Dr. M, who asks her to apply additional stains to this specimen, which Dr. M believes will identify the possible cause of a patient’s infection. Based on her original assessment of the sample, however, Dr. B believes that the so-called “bug stains” will not help diagnose the cause of this patient’s illness, that they are not indicated in this case, and that ordering them would require resources that would probably be wasted. If any additional testing is performed, Dr. B thinks that tissue cultures would be more likely to identify the cause of the infection. At the same time, she wants to maintain a good professional relationship with Dr. M, so she wonders if she should just apply the additional stains to avoid disagreement.
Commentary
This case study explores two relationships that are central to the pathologist: the patient-pathologist relationship and the pathologist-clinician relationship. The pathologist-clinician interaction is a routine and visible component of modern medicine, but the patient-pathologist relationship is less obvious [1]. Although pathologists rarely interact with their patients, they are still bound by the Hippocratic Oath to treat and prevent disease [2]. This commitment, however, manifests differently for pathologists than for other clinicians and is worthy of discussion in cases such as this one.
The Patient-Pathologist Relationship
The patient-pathologist relationship is unique in medicine; most patient care responsibilities undertaken by a pathologist never involve face-to-face interaction with a living patient. These responsibilities can include interpreting a biopsy specimen, surgical resection, or cytology fluid sample; reviewing a peripheral blood smear or flow cytometry plots; maintaining a chemistry, microbiology, hematology, or molecular laboratory; or performing an autopsy. Because these responsibilities can involve sensitive information gleaned from patients’ specimens, pathologists are obligated to protect patients’ privacy, to ensure that a specimen remains uniquely identified with a specific patient, and to treat patients’ specimens, parts, and bodies with respect [1].
Another—and perhaps the greatest—obligation pathologists have to patients is to provide pathology results that fellow clinicians can rely on when caring directly for patients [1]; pathology diagnostic information must be regarded by pathologists’ clinician colleagues as factual, reliable, and helpful in the diagnostic process. This is typically the case, as the clinically significant diagnostic error rate has been reproducibly found to be less than 1.2 percent, which, while not perfect, does provide enough reliability for clinical management of patients [3-8]. Steps taken by pathologists to mitigate the risk of misdiagnosis include mandatory continuing medical education, institutional quality assurance programs, and utilization of expert consultative services.
One of the pathologist’s many roles is directing laboratories and ensuring that quality testing is available for patients. An ideal test would not only be inexpensive but also have 100 percent sensitivity (i.e., correctly identify all patients who have a disease) and 100 percent specificity (i.e., correctly identify all patients who don’t have a disease). This ideal, however, is not the reality of laboratory testing because sensitivity and specificity are typically in opposition. Thus, if a test is highly sensitive but not specific and is performed on a patient with a low likelihood of having the disease, there is a high risk of a false positive result. False positive results lead to additional testing, which adds financial cost, and they also can cause anxiety in the patient. Screening men with serum prostate-specific antigen (PSA) testing to detect prostate cancer is one example of such a test; it is no longer recommended by the US Preventive Services Task Force, and men with false positive PSA results are prone to anxiety and sexual dysfunction [9-11]. In such cases, the pathologist must help educate the public and clinician colleagues concerning laboratory testing [1].
A less obvious aspect of a pathologist’s obligation to patients is to control costs. The Patient Protection and Affordable Care Act mandates both quality patient care and overall affordability of health insurance plans [12]. Inefficient or wasteful use of laboratory resources increases the cost of health care [13-15]. Laboratory and pathology testing accounts for at least 4 percent of total health care costs in the US [16], a number that is likely to rise with increased availability of molecular testing. Consequently, test utilization programs and lab formulary committees have been implemented in both large and small academic health care organizations to monitor costs and implement substantial cost savings when necessary [15, 17, 18]. Thus, pathologists should communicate effectively with clinicians to try to ensure that only indicated tests are ordered.
The Pathologist-Clinician Relationship
Nature of the relationship. While the patient-pathologist relationship is indirect, the pathologist-clinician relationship is visible and direct. Pathologists provide laboratory data and consultation services that are vital to helping clinician colleagues manage direct patient care. The clinician caring directly for a patient can be viewed as a mediator between a pathologist and a patient and as an interpreter of information generated by pathologists that has implications for a patient. Thus, pathologists have responsibilities to “develop habits and dispositions that further his or her relationships with clinical physicians” [1]. A strong pathologist-clinician relationship based on effective communication and mutual respect ultimately results in better and more cost-effective health care for a patient [19]. Because proper test utilization is imperative, pathologists have obligations to help a clinician colleague order tests that can be aptly applied to helping a patient; they should be familiar not only with the performance of a test but also with a patient’s clinical circumstances and the possible clinical and ethical implications of a test result for that specific patient [20].
Handling disagreement. Disagreements between health care professionals are inevitable. Stempsey acknowledges the potential for tension between the pathologist and other clinicians: “The pathologist’s being outside of the mainstream of clinical practice can sometimes lead the clinician to take the pathologist for granted and can leave the pathologist frustrated and feeling unappreciated” [1]. Awareness of this possibility can be a first step to resolving disagreements that arise, perhaps specifically about the kinds of tests that should be ordered for a patient or more generally about the goals of care for a patient. Pathologists and other clinicians all have obligations to try to identify and address problems in communication; failure to do so could have disastrous results for the patient. For example, suppose a pathologist pages a clinician with a critical result (i.e., that a peripheral blood smear is suspicious for acute promyelocytic leukemia), but the page is never received by the clinician and the pathologist does not follow up on the result because of interpersonal conflict between the two physicians; because of this communication lapse, the patient does not receive life-saving therapy (i.e., all-trans retinoic acid) immediately. Most hospitals and health centers have created codes of conduct that outline procedures for mediating intraprofessional problems, including patient care management disagreements [21].
Application to this Case
This case raises several practical and ethical questions: Should a pathologist suggest more appropriate laboratory testing when a test that’s not indicated or not likely to be helpful is ordered by a clinician colleague for a patient? Is it ethical for pathologists to perform tests they think are not indicated or not likely to be helpful for the sake of avoiding potential disagreement with a clinician colleague? If so, is it acceptable for the patient to pay the additional cost?
In this case, the pathologist, Dr. B, believes that applying additional stains will not help in the patient’s diagnosis and is not indicated. For these reasons, it would be ethical for Dr. B not to perform the requested testing, which would increase financial cost to the hospital and to the patient, possibly lead to additional unwarranted testing or treatment, and, in the case of a false positive result, could cause unnecessary anxiety or incur other risks for the patient. Health care resources are limited, and it would be unethical to knowingly misuse or waste them. Dr. B certainly could recommend an alternative test, such as tissue cultures, if she feels they are indicated.
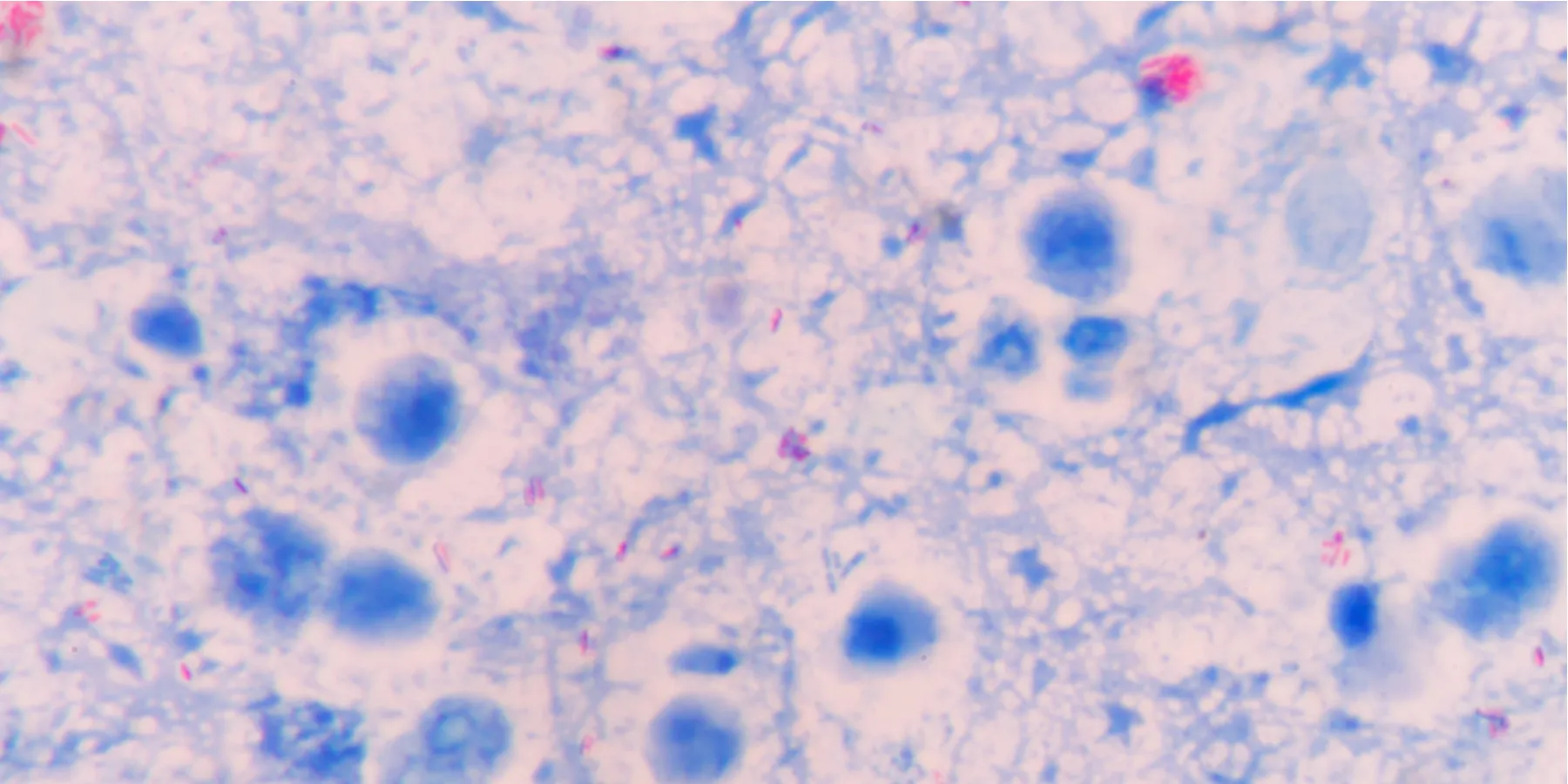
Careful morphologic assessment of a histology slide typically mitigates the need for use of additional stains. For example, some infectious organisms (e.g., Helicobacter pylori) can be identified with routine histology even though (more expensive) special stains are available for this purpose [22, 23]. Conversely, some infectious organisms (e.g., Mycobacterium tuberculosis) do require ancillary testing, such as special staining or culture techniques. In the case of inconspicuous organisms that require further staining, communication between a clinician directly caring for the patient and a pathologist regarding next steps is essential. For example, suppose granulomatous inflammation is present in a lung biopsy and a clinician informs the pathologist that the patient has lived in an area endemic for M. tuberculosis; in this set of circumstances, an acid-fast stain (i.e., Ziehl-Neelsen stain) for mycobacteria is certainly warranted. On the other hand, if the alveolated lung parenchyma is unremarkable and without an inflammatory infiltrate, applying an acid-fast stain would most likely represent poor use of resources. If a clinician suspects tuberculous infection, a pathologist could advise her or him to obtain samples for culture or for molecular diagnostic techniques.
It should be noted that, in this case, Dr. B appears to possess a sample that is formalin-fixed and paraffin-embedded (FFPE) tissue. Thus, Dr. B’s tissue sample can no longer be used for culture techniques. Newer, molecular-based assays for detection of microbial organisms can be performed on FFPE, but these assays cost more than the “bug stains” (e.g., Gömöri methenamine silver or Brown-Hopps). The high financial cost with better sensitivity and specificity of the molecular assays should be weighed against both the lower financial cost with worse sensitivity and specificity of the routine “bug stains” and the cost and practicality of obtaining fresh tissue for culture by performing another biopsy on a patient. Ideally, the decision of which test to order should be made collaboratively by pathologist and clinician. If they communicate well regarding the differential diagnosis prior to an initial biopsy or resection, then the patient’s tissue can be sent for culture at the time of the procedure.
In the case, Dr. B considers simply performing the requested staining to appease Dr. M and maintain a cordial, collegial relationship. Although this is common practice, it puts Dr. B’s professional relationship with her colleague before the interest of the patient and could therefore be considered unethical. Medicine is now firmly evidence based, and patient care decisions should be based on evidence, not on clinicians’ interpersonal relationship dynamics. A pathologist-clinician relationship, particularly one in which one professional feels unable to express an opinion, is dysfunctional and is more likely to cause harm to a patient than one in which both professionals communicate openly. A good example of possible harm comes from transfusion medicine and inappropriate use of blood products. For example, although serious adverse reactions are rare, blood component transfusion entails risk to the patient of adverse reactions, such as hemolysis, allergic reaction, transfusion-associated circulatory overload, or transfusion-related acute lung injury. Long-term sequelae, such as alloimmunization or iron-overload, are also possible harms [24]. Thus, a pathologist who is unable or afraid to communicate clearly with or to approach a clinician who might be misusing blood bank resources could be putting his or her patients at unnecessary risk for harm.
Furthermore, even if no adverse outcomes occur, patients, professionals, and organizations should not bear the financial responsibility for ensuring a cordial relationship between two clinicians. No patient should have to pay for testing that is not evidence based. Moreover, in the experience of one of the authors (MJM), fee codes for surgical pathology services that are ultimately deemed unnecessary by the attending pathologist during sign-out of surgical pathology cases, such as additional stains, are often removed from the billing portions of reports, thus placing financial burdens of the already-performed tests on the pathology department. In the case of transfusion medicine, blood products are limited resources, and it is not uncommon for blood bank reserves to be low. Giving a blood product to a patient who will not experience a benefit not only increases costs but also potentially leaves a patient who needs the transfusion more urgently at risk of not receiving it.
Conclusion
In summary, it is important for pathologists and clinicians to have cooperative, collaborative, professional relationships that allow for open discussion of ideas and are informed by evidence. Pathologists, as the mediators of laboratory medicine, should not hesitate to question requests for testing that’s not clinically indicated and should not hesitate to recommend more suitable approaches that meet a patient’s and clinicians’ needs. Sometimes, it is in the best interest of a patient for a pathologist to deny certain laboratory testing or services, and a patient should never be held financially responsible for wasted health care resources.
References
-
Stempsey WE. The virtuous pathologist: an ethical basis for laboratory medicine. Am J Clin Pathol. 1989;91(6):737.
-
Johns Hopkins Sheridan Libraries and University Museums. Hippocratic Oath: modern version. http://guides.library.jhu.edu/c.php?g=202502&p=1335759. Updated May 23, 2016. Accessed March 23, 2016.
- Troxel DB. Error in surgical pathology. Am J Surg Pathol. 2004;28(8):1092-1095.
- Safrin RE, Bark CJ. Surgical pathology sign-out. Routine review of every case by a second pathologist. Am J Surg Pathol. 1993;17(11):1190-1192.
- Ramsay AD, Gallagher PJ. Local audit of surgical pathology. 18 month’s experience of peer review-based quality assessment in an English teaching hospital. Am J Surg Pathol. 1992;16(5):476-482.
- Lind AC, Bewtra C, Healy JC, Sims KL. Prospective peer review in surgical pathology. Am J Clin Pathol. 1995;104(5):560-566.
- Wakely SL, Baxendine-Jones JA, Gallagher PJ, Mullee M, Pickering R. Aberrant diagnoses by individual surgical pathologists. Am J Surg Pathol. 1998;22(1):77-82.
- Renshaw AA, Cartagena N, Granter SR, Gould EW. Agreement and error rates using blinded review to evaluate surgical pathology of biopsy material. Am J Clin Pathol. 2003;119(6):797-800.
-
US Preventative Services Task Force. Final recommendation statement: prostate cancer: screening, May 2012. http://www.uspreventiveservicestaskforce.org/Page/Document/RecommendationStatementFinal/prostate-cancer-screening. Accessed May 24, 2016.
- Katz DA, Jarrard DF, McHorney CA, Hillis SL, Wiebe DA, Fryback DG. Health perceptions in patients who undergo screening and workup for prostate cancer. Urology. 2007;69(2):215-220.
-
Lin K, Croswell JM, Koenig H, Lam C, Maltz A. Prostate-specific antigen-based screening for prostate cancer: an evidence update for the US Preventive Services Task Force. Rockville, MD: Agency for Healthcare Research and Quality; 2011. AHRQ publication 12-05160-EF-1. http://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0032900/pdf/PubMedHealth_PMH0032900.pdf. Accessed April 29, 2016.
-
Patient Protection and Affordable Care Act of 2010, Pub Law No. 111-148, 124 Stat 119.
- Robinson A. Rationale for cost-effective laboratory medicine. Clin Microbiol Rev. 1994;7(2):185-199.
- Benson ES. Initiatives toward effective decision making and laboratory use. Hum Pathol. 1980;11(5):440-448.
- Kim JY, Dzik WH, Dighe AS, Lewandrowski KB. Utilization management in a large urban academic medical center: a 10-year experience. Am J Clin Pathol. 2011;135(1):108-118.
-
Hanson C, Plumhoff E. Test utilization and the clinical laboratory. Mayo Medical Laboratories Comminiqué. May 2012. http://www.mayomedicallaboratories.com/articles/communique/2012/05.html. Accessed April 29, 2016.
- Warren JS. Laboratory test utilization program: structure and impact in a large academic medical center. Am J Clin Pathol. 2013;139(3):289-297.
-
Paxton A. Slashing send-out costs with lab formularies. CAP Today. July 2014. http://www.captodayonline.com/slashing-send-out-costs-with-lab-formularies/. Accessed April 29, 2016.
-
Sbarbaro JA. Enter the pathologist/clinician. Chest. 1984;86(6):805.
-
Legg MA. What role for the diagnostic pathologist? N Engl J Med. 1981;305(16):950-951.
- Andrew LB. Conflict management, prevention, and resolution in medical settings. Physician Exec. 1999;25(4):38-42.
- Vartanian RK, Leung JK, Davis JE, Kim YB, Owen DA. A novel Alcian yellow-toluidine blue (Leung) stain for Helicobacter species: comparison with standard stains, a cost-effectiveness analysis, and supplemental utilities. Mod Pathol. 1998;11(1):72-78.
-
Guy CD, Giltman LI, Varma VA. Comparison of histochemical stains for the diagnosis of Helicobacter pylori [ASCP/CAP abstract 21]. Am J Clin Pathol. 1997;107(4):473.
-
Petrides M, Cooling L, Maes LY, Stack G. Practical Guide to Transfusion Medicine. 2nd ed. Bethesda, MD: AABB Press; 2007.