Abstract
When hospitals became places of treatment and recovery rather than places of sickness and death, hospital-based patient care also changed. This article examines relationships between design-induced practice transformations in US hospitals between the 1850s and 1980s and transformations in hospitals’ roles in American communities, with a specific focus on underserved communities.
Shifts in Hospital-Community Interactions
World War II marked a turning point in community hospital history. During the 19th century, hospitals underwent a transformation1,2—from traditional charitable institutions that provided “a place to be sick and die” to modern medical institutions that offered “a place to live and get well.”3 An undesirable side effect of that shift, however, was an increasingly impersonal interaction between caregiver and patient and between the hospital and the community it inhabited. In reaction, postwar hospital practitioners hoped that the hospital of the future “would be inherently connected to a specific community” and thereby provide better, more personal care.4 Although this hope—that better community integration would improve care—implied that hospitals were not sufficiently connected to a specific community, the history of hospitals reveals that each hospital was a specific, locally determined attempt to provide service to a perceived underserved community. Over time, what changed was not just the interaction of hospital and community and the nature of care provided but which community was serving and being served.
This article uses the history of architecture—particularly, hospital site choice and building layout—and the history of the changing community context and individual institutions to illuminate hospital-community interactions since the 1860s. The transformations in such interactions occurred first in urban areas, then spread across the nation; this article initially draws on examples from New York City and then expands the discussion to include smaller towns and rural areas.
A Hospital for Each Community
In 1869, a call to support a new Presbyterian hospital in New York City noted that Jewish, German, Catholic, and Episcopalian communities had founded hospitals “for the exclusive benefit of their own people”5 but that Presbyterian community members did not yet have a hospital of their own.5,6 At a time when home care—whether by family members or by physicians making house calls—was the norm, these hospitals were charities, providing free or low-cost care to the sick poor. Although each hospital officially admitted patients of any creed, race, or ethnicity, each also tailored its offerings to its own community. Presbyterian services were held in the Presbyterian Hospital, Jewish services in Mount Sinai, and Catholic services in St Vincent’s. German physicians practiced in the German Hospital and Jewish physicians in Mount Sinai and Beth Israel.
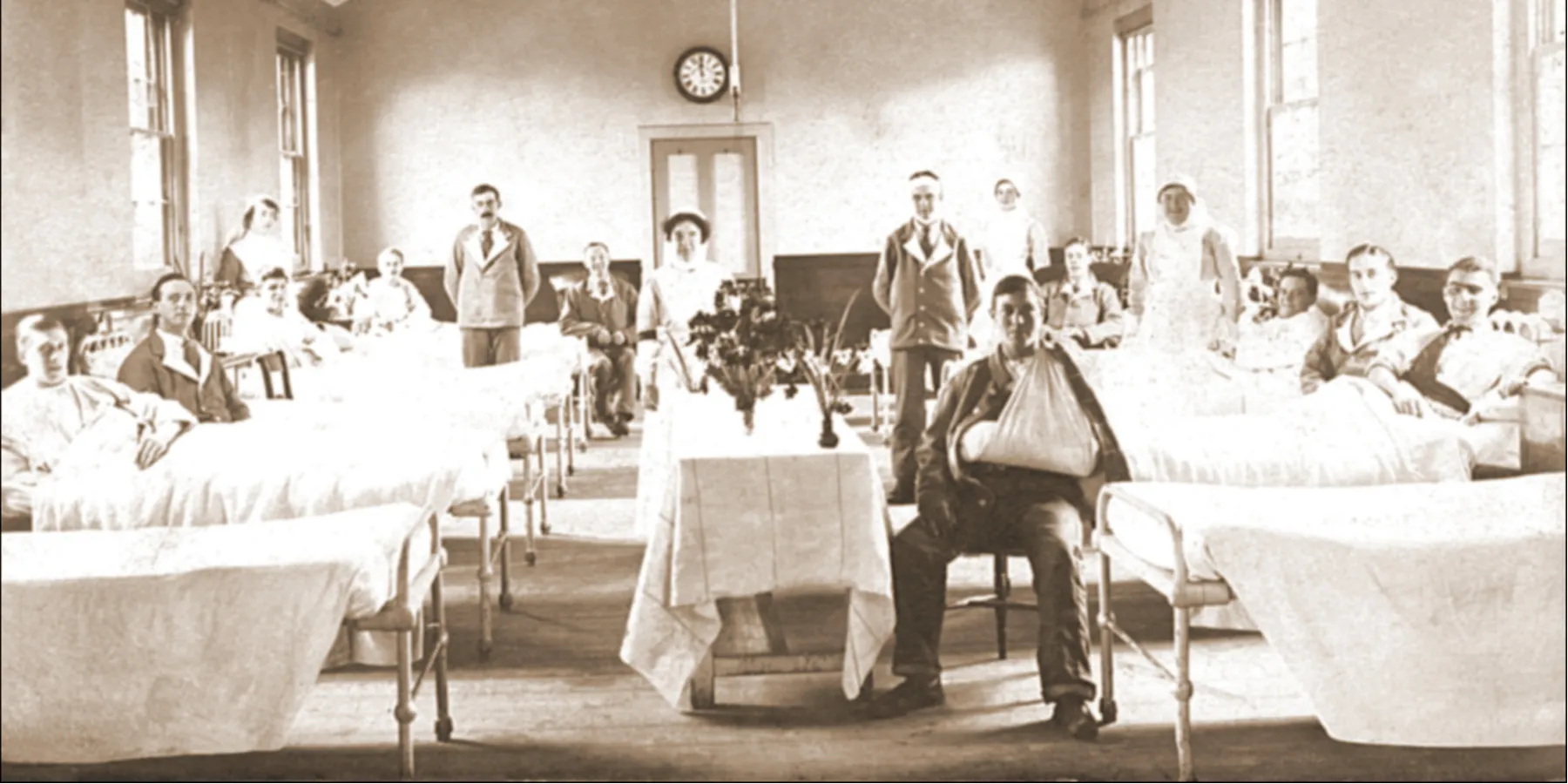
These hospitals’ facilities were arranged in pavilion-wards—a standardized design popularized worldwide by Florence Nightingale—which promised to make hospital buildings into places of cure rather than incubators of disease. Pavilion-ward hospital buildings included hygienic materials and details, large open wards, support spaces, and little else.7-9 Pavilion-ward designs were widely adopted in the late 19th century across the United States, whether in large cities, small towns, or rural areas. St Elizabeth Hospital in Utica, New York, offered essentially the same facilities as St Luke’s Hospital in Chicago, Illinois; the Miners’ Hospital in Hazleton, Pennsylvania; the Grady Memorial Hospital in Atlanta, Georgia; or the Good Samaritan Hospital in Portland, Oregon.
The greatest variation in hospital service was the result of site choice. Pavilion-ward guidelines required that sites be located beyond the built-up areas of a city, distant from their supporting community. In Manhattan of the 1870s, the centers of population remained below 23rd Street, but 8 general hospitals, including the Presbyterian Hospital, were all located above 54th Street, at least an hour horse-car ride away.10,11 This travel distance could prove excruciating or even deadly to patients with severe injuries or in need of urgent care. A handful of hospitals, including St Vincent’s and Beth Israel, did occupy sites embedded within the population center of the community they served.11 Travel time to their doors was measured in minutes.
The distance of a hospital from its community affected its patient composition and consequently its medical service. The remote hospitals filled slowly. For the first years of its operation, a good proportion of the Presbyterian Hospital’s beds were empty or occupied by nonurgent cases, and the surgeons were bored.12,13 To attract more patients, the directors increased the amount of free care, established a dispensary (an outpatient clinic), and added an ambulance department to facilitate getting the patients safely and quickly to the hospital.14-16 By the 1890s, one-third of the patients were delivered by ambulance from a variety of distant neighborhoods and only 10% of all inpatients were Presbyterians.17 In contrast, the embedded hospitals quickly filled with patients drawn largely from their immediate surroundings. Even without ambulances, Beth Israel Hospital, located in the geographic center of the densely populated, largely Jewish Lower East Side, was constantly turning away applicants.18,19 The hospital’s active dispensary service compensated for the overcrowding, treating 21 875 patients in 1897 and 70 423 patients in a larger facility in 1907. The vast majority of the hospital’s inpatients in the late 1890s and early 1900s—80% to 95%—were from Russia and Central Europe; most were Jewish.19,20 The hospital kept kosher and held Sabbath.20
Geographic distinctions reinforced institutional differences, creating 2 distinct types of hospital that served different communities and interacted with those communities differently. Hospitals that were physically embedded within a specific community offered care that was culturally and socially as well as medically specific to their patient community. Hospitals remote from the community they served developed a more diverse patient base and medically focused practice that de-emphasized patients’ specific social, ethnic, or cultural background.
1900s-1950s: Hospitals for Physicians and for All Patients
In the first decades of the 20th century, hospitals became locations of collaborative, specialized scientific medicine (ie, medicalized) and served all classes of patients, not just the poor. These medical and social transformations imposed new spatial requirements on the ubiquitous large pavilion-ward facilities. The medicalized hospital was focused on the physician and added extensive diagnostic, treatment, therapeutic, research, and educational spaces to the ward pavilions. Yet the medicalized hospital was open to all and thus also was focused on patients, adding a socioeconomic-spatial hierarchy of private rooms (for wealthy patients who paid in full), semiprivate rooms and small wards (for middle-class patients who paid for part of their care), and large wards (for poor patients who still received care at no or minimal cost). In contrast to remote urban medicalized hospitals, embedded urban and smaller rural hospitals served a specific community in facilities that typically included only necessary medical spaces and technologies but provided more personalized care.
Medicalized hospitals. The medicalized hospital’s purpose was the creation of better physicians.21,22 According to physician E. H. Lewinski-Corwin, the most important feature of the community hospital was “the opportunity it offers for organized and supervised team work, for critical analysis of the performance, and for the advancement of standards of medical education and practice in the community.”23 Designed for physicians and the increasingly complicated medicine they practiced, facilities ranged from smaller medically specialized institutions (like the Herman Knapp Memorial Eye Hospital) to gargantuan teaching hospitals and medical centers (like the Columbia Presbyterian Medical Center). These facilities housed not only patients but also, by the 1920s, an extensive array of specialized equipment and facilities such as x-ray, surgery, hydrotherapy, electrotherapy, physical therapy, laboratories, lecture rooms, collaborative meeting spaces, physicians’ lounges, medical libraries, and private physicians’ offices.7,24
Medicalized hospitals for all classes. Medicalized hospitals drew patients from multiple socioeconomic and geographic communities, making site accessibility critical to the institution’s success. The Columbia-Presbyterian Medical Center at 168th Street and Broadway was near Riverside Drive (a major highway facilitating access by suburban physicians and their affluent private patients), adjacent to a subway stop (facilitating access by a variety of patients from across the city or even from other cities), and near densely populated Washington Heights.25 The shifting composition of that neighborhood—from Irish to Hungarian, Polish, and German—was an indifferent factor in the care provided.
While the new medical hospitals attracted patients from all classes and diverse socioeconomic groups, accommodation of the variety of patients was far from equal. Most hospitals separated patients according to their medical condition and their economic status (whether in private rooms or charity wards). While hospitals did not officially separate patients based on their ethnicity, hospitals across the country (particularly in the South) provided separate, less attractive rooms, wings, or buildings for minority patients.7 And many medicalized hospitals targeted a single, underserved, patient community—whether that community was socially, geographically, or economically defined. Underprivileged (ie, ethnic, immigrant) communities remained the focus of newly founded embedded hospitals for more recent immigrant groups (like the French, Italian or Hungarian hospitals), and many provided extensive free or at-cost care to their patient community in larger wards.7
By the 1920s, as immigrant neighborhoods turned over, the older embedded hospitals in urban areas such as New York City faced the dilemma of whether to move with their original core community or to provide service to the new surrounding community. St Vincent’s Hospital remained on its original site, providing care in large wards to the remaining poorer residents but also serving the wealthier new residents in added private patient facilities.26 Beth Israel’s hospital directors chose to follow the Jewish population uptown, shifting the nature of the hospital’s service to match the improved economic circumstances of its original patient community. The new building at Stuyvesant square included small single-bed rooms to encourage use by middle-class patients, not just the poor.27 Other new hospitals (like the Fifth Avenue Hospital) also targeted the middle class by providing attractive facilities with smaller wards, comfortable patient lounges, and sites near parks.28,29
Hospitals for small towns. The medically specialized, all-class modern hospital and its success in treating many conditions was a hallmark of larger cities, thereby transforming small towns and rural areas into underserved communities. Many smaller towns did have existing hospitals, but they were built and operated on the old charitable model (full of wards and little else) and offered basic care by local “backwoods” physicians rather than research-based, specialized care by new professional physicians.30-32
Modern medicine required modern facilities, and providing an effective small modern hospital in remote areas was a design problem of intense interest but with varying solutions. Local decisions determined not only the facility design but also the kind of practice offered in the hospital. In 1922, G. R. Egeland in Sturgeon Bay, Wisconsin, grew tired of practicing medicine without modern equipment. He studied the problem of small hospitals and built one for the town himself.33 Some communities, believing that “the presence of hospital facilities alone appears to be one of the largest factors in attracting physicians to a community,” built well-equipped modern hospitals with that hope in mind.34 In contrast, the town of Leominster, Massachusetts, “demanded its own small but adequate hospital in preference to a large and modern one some distance away.”35 Smaller hospitals, embedded within specific communities, provided essential but limited medical facilities and equipment and offered more personal, but less medically specialized, care.
Hospitals Everywhere, With Local Variations
By the 1940s, it was clear that every geographic location deserved a modern hospital. After World War II, the Hill-Burton Act made federal funds available for hospital construction in underserved areas—quantified as 4.5 beds per 1000 persons of population.36-39 Requisite statewide community hospital surveys revealed that small towns, rural areas, and poor urban neighborhoods occupied the gaps on the map of adequate hospital coverage.36,40
While the US Public Health Service imposed minimum design and equipment standards to guarantee that public funds would create modern hospitals, local customs, de facto segregation, and other social divisions could alter the nature of the service.41 The addition of private rooms and physicians’ offices to a hospital, for example, could transform the community hospital into an elite institution serving the wealthy rather than all classes. The George H. Lanier Memorial Hospital (and many other Hill-Burton funded hospitals) provided “separate-but-equal” facilities for minority patients.42 Although the Civil Rights Act of 1964 officially ended segregation within federally funded facilities,40 within individual institutions, desegregating facilities and increasing access to minority physicians and patients was difficult. Nevertheless, desegregation was enforceable, visible, and largely successful.43 Geographically reinforced institutional segregation, however, has been more persistent, as hospitals embedded in poor and ethnic neighborhoods inevitably have a higher proportion of disadvantaged and minority patients than hospitals located in affluent neighborhoods; care and facilities available within these disparate institutions is far from equivalent.
In 1965, the War on Poverty shifted legislation and funding to promote neighborhood or community health centers (CHCs) in economically disadvantaged communities.44,45 Design guidelines shifted from minimum standards for a facility (such as a minimum number of beds) to a minimum standard of care. The early CHCs opened in borrowed and repurposed buildings—the Tufts-Delta Health Center in Mississippi opened in a remodeled church.45 These community health centers were conceived not as a medical workshop but “as a base for multiple points of entry into the problems of health and poverty,”45 providing care and treatment as well as jobs and training.45,46 This development was, in many ways, a return to the late 19th century embedded charity hospital but in a new architectural package.47
Health Care Spaces in Communities of the Future
History reveals the complexity and variety of the communities served by community hospitals. That variety also showed up architecturally in site choice and facility designs. Remote institutions broadened patient access by drawing from multiple socioeconomic and geographic communities, but by the end of World War II the care in these large-scale, technology-filled medical workshops was far from equal. During the same period, embedded institutions targeted a specific geographic or socioeconomic community, offering more personal care but limiting the specialized facilities available and consequently the medicine practiced within them. The current idea of a medical home and its goal of coordinating care will further alter the nature of hospital service. That the medical home is not a place will require another, perhaps broader, redefinition of community.
Twenty-first century concerns are prioritizing patient communities and promoting smaller-scale embedded facilities.47 The history of hospitals, however, makes it clear that today’s institutional answer is itself subject to transformation. The takeaway is not the appropriateness of serving a specific community and tailoring service to it but an acknowledgment of the choice being made and its consequences.
References
-
Rosenberg CE. The Care of Strangers: The Rise of America’s Hospital System. New York, NY: Basic Books; 1987.
-
Starr P. The Social Transformation of American Medicine. New York, NY: Basic Books; 1982.
-
Looking forward. Mod Hosp. 1948;107(2):45.
-
Aydelott AL, MacLean BC. The hospital design. Mod Hosp. 1948;107(2):48-55.
-
Presbyterian Hospital New York City. First Annual Report. New York, NY: Trow & Smith Book Manufacturing Co; 1869. https://babel.hathitrust.org/cgi/pt?id=nnc2.ark:/13960/t9h42f159;view=1up;seq=7. Accessed September 12, 2018.
- Lehr TK. Origins of a local hospital: the real story. J Public Health Policy. 1996;17(1):71-79.
-
Kisacky J. Rise of the Modern Hospital: An Architectural History of Health and Healing. Pittsburgh, PA: University of Pittsburgh Press; 2017.
-
Thompson JD, Goldin G. The Hospital: A Social and Architectural History. New Haven, CT: Yale University Press; 1975.
-
Adams A. Medicine by Design: The Architect and the Modern Hospital, 1893-1943. Minneapolis, MN: University of Minnesota Press; 2008.
-
Delavan DB. Early Days of the Presbyterian Hospital in the City of New York. East Orange, NJ: Abbey Printshop; 1926.
-
Kisacky J. An Architecture of Light and Air: Theories of Hygiene and the Building of the New York Hospital, 1771-1932 [dissertation]. Ithaca, NY: Cornell University; 2000.
-
Bellevue hospital: the opinions of leading physicians as the building’s fitness for hospital purposes. New York Times. June 9, 1873.
-
The Presbyterian hospital. New York Times. June 28, 1873.
-
Anniversary of the Presbyterian Hospital. New York Times. April 9, 1874.
-
Presbyterian Hospital New York City. Eleventh Annual Report. New York, NY: Trow’s Printing & Bookbinding Co; 1879. https://babel.hathitrust.org/cgi/pt?id=nnc2.ark:/13960/t7dr3jj6v;view=1up;seq=13. Accessed September 12, 2018.
-
One year in a hospital. New York Times. April 15, 1881.
-
Presbyterian Hospital New York City. Twenty-First Annual Report. New York, NY: Trow’s Printing & Bookbinding Co; 1889. https://babel.hathitrust.org/cgi/pt?id=nnc2.ark:/13960/t10p1rn1f;view=1up;seq=9. Accessed September 12, 2018.
-
Beth Israel Hospital: a worthy philanthropic institution of the East Side. New York Times. October 6, 1895.
-
Beth Israel Hospital New York City. Annual Report of the Directors of Beth Israel Hospital. New York, NY: A Ginsberg & Bros Printers; 1897.
-
Beth Israel Hospital New York City. Seventeenth Annual Report of the Directors of Beth Israel Hospital. New York, NY: Shapiro & Portugal Printers; 1907.
-
Presbyterian Hospital New York City. Thirty-Sixth Annual Report. New York, NY: [publisher unknown]; 1904. https://babel.hathitrust.org/cgi/pt?id=nnc2.ark:/13960/t9c549f7v;view=1up;seq=7. Accessed September 12, 2018.
-
New York Skin and Cancer Hospital. Annual Report. New York, NY: [publisher unknown]; 1908.
- Corwin EHL. Community responsibility of hospitals. Mod Hosp. 1926;26(2):109-113.
- Adams A, Schlich T. Design for control: surgery, science, and space at the Royal Victoria Hospital, Montreal, 1893-1956. Med Hist. 2006;50(3):303-324.
-
Presbyterian Hospital New York City. Medical center bulletin. October 27, 1925. Miscellaneous Folders, Medical Center Bulletins, 1925-1928: Columbia Presbyterian Medical Center. New York, NY: Archives and Special Collections, A. C. Long Health Sciences Library, Columbia University.
-
St Vincent’s Hospital New York City. 89th Annual Report, for the Year 1938. New York, NY: D & J Sadler & Co; 1939.
- Frank LJ. The spirit of Beth Israel. Mod Hosp. 15(2):110-112.
- Woodbury WE. New fifth avenue hospital embodies striking structural features. Mod Hosp. 19(3):187-192.
- Neergaard CF. The Carson C. Peck Memorial Hospital. Mod Hosp. 14(5):341-348.
- Pettit RT. The diagnostic hospital of a small community. Mod Hosp. 1921;17(3):195-199.
-
The influence of the war on hospital development. Trained Nurse Hosp Rev. 1920;64(1):39-40.
-
Mills AB, ed. The Modern Small Hospital and Community Health Center. Chicago, IL: Modern Hospital Publishing Co; 1946.
- Egeland GR. An economically built small hospital. Mod Hosp. 19(5):387-390.
- Division of Hospital Facilities, US Public Health Service, Federal Security Agency. The twenty-five bed hospital: an additional plan for the coordinated hospital system. Mod Hosp. 1948;71(1):48-53.
- Hill WC. A New England community hospital. Mod Hosp. 1924;23(4):307-310.
-
Lave JR, Lave LB. The Hospital Construction Act: An Evaluation of the Hill-Burton Program, 1948-1973. Washington, DC: American Institute for Public Policy Research; 1974.
-
Walsh GP; United States. Hospital Survey and Construction Act With Amendments. Washington, DC: US Government Printing Office; 1981.
- Perlstadt H. The development of the Hill-Burton legislation: interests, issues and compromises. J Health Soc Policy. 1995;6(3):77-96.
- Mantone J, The big bang. The Hill-Burton Act put hospitals in thousands of communities and launched today’s continuing healthcare building boom. Mod Healthc. 2005;35(33):6-7, 16, 1.
- Thomas KK. The Hill-Burton Act and Civil Rights: expanding hospital care for black southerners, 1939-1960. J South Hist. 2006;72(4):823-870.
- Hospital Facilities Section, US Public Health Service, Federal Security Agency. Elements of the general hospital. Archit Rec. 1946;99(6):72-90.
-
First of the Hill-Burton hospitals: George H. Lanier Memorial Hospital, Langdale, Ala. Archit Rec. 1950;107(6):146-153.
- Reynolds PP. The federal government’s use of title VI and Medicare to racially integrate hospitals in the United States, 1963 through 1967. Am J Public Health. 87(11):1850-1858.
-
Lefkowitz B. Community Health Centers: A Movement and the People Who Made It Happen. New Brunswick, NJ: Rutgers University Press; 2007.
- Geiger HJ. The first community health center in Mississippi: communities empowering themselves. Am J Public Health. 2016;106(10):1738-1740.
- Adashi EY, Geiger HJ, Fine MD. Heath care reform and primary care—the growing importance of the community health center. N Engl J Med. 2010;362(22):2047-2050.
-
Sloane DC, Sloane BC. Medicine Moves to the Mall. Baltimore, MD: Johns Hopkins University Press; 2003.