Abstract
Hypovitaminosis D is a prevalent micronutrient deficiency that can be severe and hard to treat in children with short bowel syndrome, a condition treated with substantial bowel resection. Surgically altered bowel anatomy then results in iatrogenic digestion and absorption limitations that require short- and long-term management and follow-up. Care of children with hypovitaminosis D standardly includes prescription dietary micronutrient supplementation, sometimes in irregularly high doses. This commentary responds to a pediatric case of vitamin D toxicity and suggests micronutrient-prescribing risk mitigation strategies in light of the absence of regulatory oversight of over-the-counter dietary supplements, inadequate insurance coverage, and easily available commercial retail products.
Case
MP is a teenage girl with short bowel syndrome (SBS) related to gastroschisis, initially leaving her with approximately 10 centimeters of small bowel in continuity with her descending colon. Following multiple autologous intestinal reconstructive surgeries performed to address clinically relevant bowel dilation, her small bowel length was measured at 73 centimeters. Her clinical course has been complicated by intestinal failure-associated liver disease, recurrent small bowel bacterial overgrowth, limited vascular access related to thrombosis that requires anticoagulation, and multiple central line-associated bloodstream infections prior to central line removal. She achieved enteral autonomy with line removal at age 10 years.
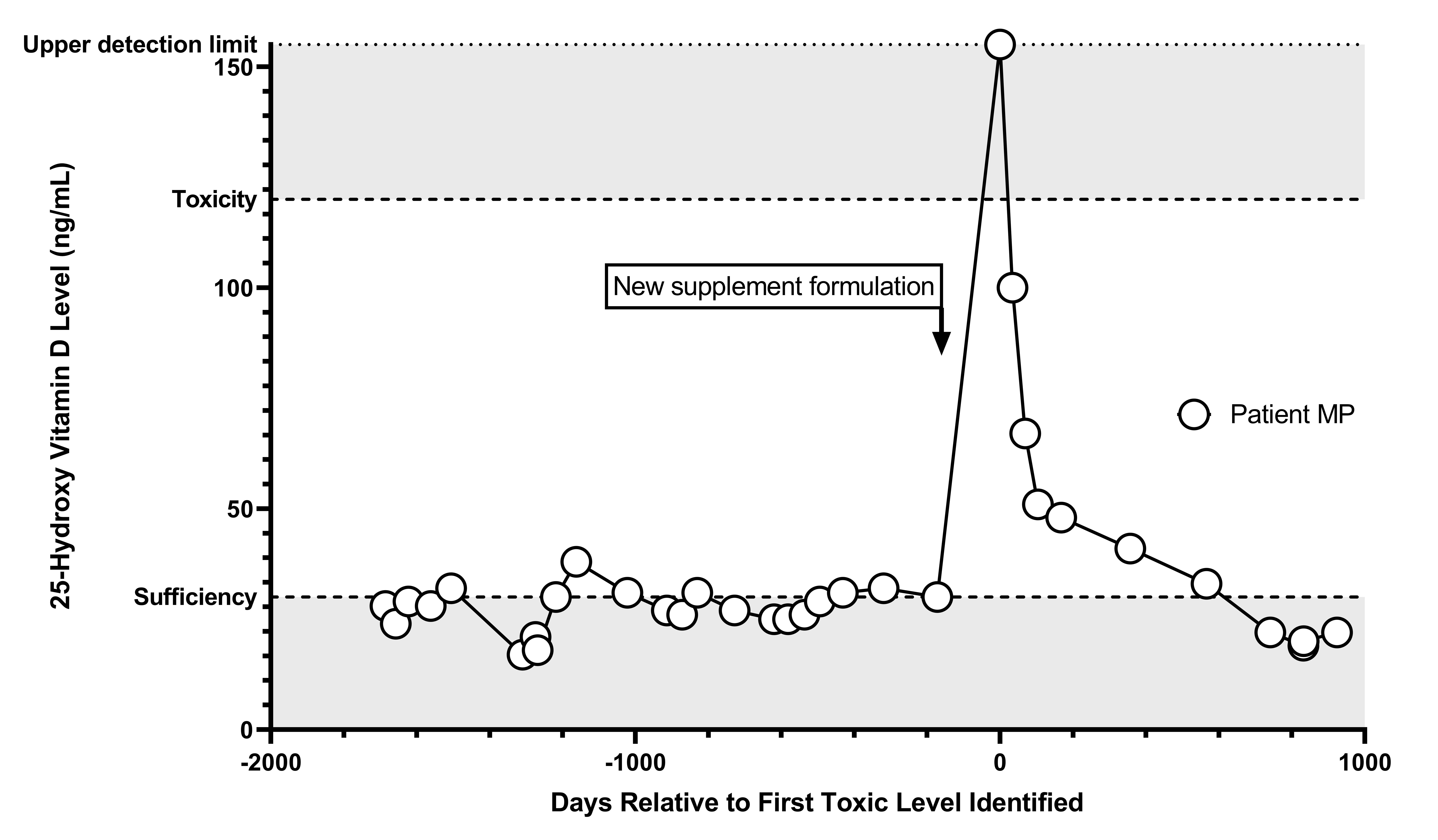
MP was found to have a toxic 25-hydroxy vitamin D level in August of her ninth year. At 4 years of age, she began a series of upward ergocalciferol titrations in response to insufficient vitamin D levels through December of her seventh year, when she began receiving ergocalciferol at a dose of 24 000 international units (IU) daily administered through her gastrostomy tube. Subsequent repeated insufficient vitamin D levels prompted a transition to cholecalciferol 50 000 IU administered daily through her gastrostomy tube. However, her vitamin D levels were largely insufficient with this dose, with values ranging from 25 to 32 ng/mL over the next year-and-a half. In early summer of MP’s ninth year, her mother transitioned from purchasing her cholecalciferol from a local pharmacy to purchasing it from a large e-commerce platform due to insurance coverage barriers that lead to a high out-of-pocket cost. Following this transition, MP’s 25-hydroxy vitamin D level rose beyond the upper limit of detection, from 30 ng/mL to greater than 155 ng/mL (see Figure). MP’s serum calcium was normal (9.2 mg/dL). Supplementation was discontinued and monthly vitamin D levels were obtained. Vitamin D supplementation was resumed, with cholecalciferol 10 000 IU administered twice daily and purchased through a local pharmacy.
Figure. MP’s 25-Hydroxy Vitamin D Levels
Commentary
Pediatric intestinal failure (IF) occurs when bowel digestive and absorptive function is insufficient to meet the demands of a growing body. Pediatric SBS is a heterogenous disorder resulting from extensive small bowel resection in the setting of primary bowel pathologies such as necrotizing enterocolitis and gastroschisis. Pediatric SBS is the most common cause of IF. The remnant bowel undergoes a process of physiologic adaptation over a period of years, increasing gut function and permitting the achievement of enteral autonomy in most patients, although the loss of key areas of the gut can be felt through the remainder of the child’s life. Hypovitaminosis D is a prevalent micronutrient deficiency that can be severe and hard to treat in children with SBS.
Vitamin D Deficiency in SBS
Micronutrient deficiency is common in IF, including deficiencies of fat-soluble vitamins, copper, and iron.1,2,3 These deficiencies risk metabolic bone disease, infection, anemia, thrombosis, demyelinating disease, growth failure, and more.4,5,6,7,8 Programs that care for children with SBS typically monitor vitamin and mineral levels.9 Vitamin D inadequacy is among the most common findings, with a prevalence of 20% to 42% during the months-to-years-long process of weaning from parenteral nutrition and of 30% to 68% after achievement of enteral autonomy.1,2,10
Vitamin D, a fat-soluble vitamin also referred to as calciferol, primarily promotes calcium absorption from the gut and facilitates bone mineralization for growth and strength. Vitamin D deficiency is associated with metabolic bone diseases such as rickets and osteomalacia, signs and symptoms of which include delayed growth, delayed acquisition of motor skills, bony pain, and muscular weakness.11 Vitamin D has additional roles in many organ systems, and hypovitaminosis D increases risk of many diseases.12
The achievement of nutritional sufficiency in patients with SBS through enteral supplementation is challenging due to malabsorption, decreased intestinal mass, and incomplete or absent coverage of supplementation costs. Thus, the high prevalence of hypovitaminosis D in patients with SBS supports the need for a systematic approach to supplementation, often employing doses higher than those used in other populations.13 Vitamin D supplementation can be in the form of ergocalciferol (D2) or cholecalciferol (D3). Supplements can be prescribed or obtained over the counter (OTC), with estimates of out-of-pocket costs ranging from $12 to $70 per month or more depending on dose and preparation (eg, liquid).14,15 Heightened testing needs are also costly.16
In 2020, the Intestinal Rehabilitation and Nutrition Support Center at Nationwide Children’s Hospital cared for 165 patients with SBS. Of these, 142 (86%) were supplemented with vitamin D with a median dose of 10 000 IU per day, with a range of 200 IU to 100 000 IU per day (E. A. Mezoff, MD, and R. Lee, unpublished data, 2020). Of note, the recommended dietary allowance (RDA) for vitamin D in children is 600 IU per day.17
Toxicity of vitamin D leads to hypercalcemia and imbalance in the regulation of bone metabolism. Hypercalcemia can cause symptoms of toxicity that span the neurological, gastrointestinal, and renal systems.18 In this case, a child developed vitamin D toxicity in the context of a complex medical condition in which high doses were needed. While the need for such high doses of vitamin D is rare, the ethical and practical challenges of prescribing vitamin D and other unregulated dietary supplements (DS) apply to many patient populations.
Inconsistent Access to Vitamin D
Despite the essential physiologic function of vitamin D and the deleterious side effects of vitamin D deficiency, most vitamin D preparations are sold as OTC DS. Insurance companies frequently restrict access due to OTC status.19 Inconsistent insurance coverage of OTC vitamin D and out-of-pocket costs of these preparations raise health equity concerns. As described in the case, MP transitioned from a product purchased at the local pharmacy to one purchased from an e-commerce platform due to insurance coverage barriers that lead to a high out-of-pocket cost. Unfortunately, DS purchased on large e-commerce platforms may be unreliable, as manufacturers may seek to cut costs. An additional issue that arises in this example is that the local pharmacy cannot be contacted to verify adherence, as can be done when a DS is prescribed and dispensed from a pharmacy.20
Absence of or Limited Regulation of Vitamin D Supplementation
In addition to concerns about toxicity, as in our case (MP fortunately remained asymptomatic), ineffective treatment that leads to persistent deficiency also poses an important risk to patients. Many DS contain micronutrients for which RDAs have not been determined, which can further complicate the issue of supplementation in the clinical and research setting.
Because manufacturing processes can be inconsistent, these products can contain quantities of ingredients in amounts not listed on the label. This inconsistency can lead to either over- or underdosing the desired supplement, which in turn can lead to poor clinical outcomes for patients. In the United States, deficits in regulatory and labeling laws also compromise the effectiveness and safety of these preparations.21,22 In the case of vitamin D, for example, a widely available preparation has a dose of 50 000 IU (which is 12 500% of the RDA).16 At the other extreme, in one study of echinacea products, 10% of samples contained no echinacea, and only 43% met the quality standard described by the label, suggesting that most echinacea products did not contain the claimed ingredient content.23
In addition, there are numerous reports of contamination and adulteration of DS with heavy metals and pharmaceutical compounds.24 For example, the US Food and Drug Administration has reported hundreds of adulterated sexual enhancement supplements.25 There has been some focus on improved regulation, including labeling requirements, mandatory adverse event reporting, and proposals for increased integrity of the manufacturing process.24,26,27 Nevertheless, the existing regulations are too narrow in scope, often ignored, and difficult to police. With 72% of adults and 50% of children using DS,28 clinicians must be aware of the potential risks involved with DS use, either when prescribed or obtained OTC.
Recommendations for Patient Education on Supplementation
To mitigate health risks due to inconsistent manufacturing processes, clinicians should guide patients to choose DS that are verified by the United States Pharmacopeia (USP). The USP Convention is a 200-year-old nonprofit organization that promotes safety of drugs, foods, and DS by establishing standards for quality and purity, auditing manufacturing facilities, and performing quality control testing.29 The USP verified mark ensures that a product contains the ingredients listed on the label in the declared potency and amounts and does not contain harmful levels of contaminants.30 A study that evaluated the potency of different vitamin D preparations found that the manufacturer that had USP verification had “generally more accurate and less variable” content of vitamin D, whereas the remaining manufacturers’ products had highly variable content, with potency of all OTC products ranging from 9% to 146% of the amount of vitamin D listed on the label.31 Unfortunately, only a very small percentage of DS use the USP seal, and other verification seals exist and can confuse consumers.23,29
Data indicate that 15% of people take pharmaceuticals and DS concurrently and that potential adverse interactions occur in 40% of users.32,33 Due to the risk of DS contamination and adulteration, inconsistent DS manufacturing processes, and the absence of pharmacokinetic data, these interactions can present a diagnostic challenge. Clinicians should be aware that the highest risk occurs in patients taking drugs with a narrow therapeutic window, such as digoxin and warfarin.24 Additionally, St John’s wort and ephedra are commonly involved in DS-drug interactions.26,34
A 2006 survey found that 38% of acute care facilities do not have a formal policy on DS use and that most allow DS if they are ordered by an “authorized prescriber.”35 Clinicians tasked with recommending or continuing DS use—or who have concerns regarding toxicity, adverse effects, or drug interactions—should have an open conversation with their patients about these products and their goals for use (see Table) and consider consulting with a medical toxicologist or regional poison center.
| Category | Questions |
|---|---|
| Origin | Who recommended the supplement? |
| Why is that person’s advice trusted? | |
| Rationale | What is supplementation trying to achieve |
| Is the preference for regulated or unregulated supplements, and why? | |
| What does regulation mean? | |
| Options | What are the options (eg, preparation and/or formulation, dosing route, concentration) and how are they regulated? |
| Are there medical reasons to narrow the options? | |
| What are the costs of options and what is good value? | |
| Where can the options be obtained? | |
| Is the source trusted? | |
| Goal | How will we know the supplement is effective? |
| How will we know the supplement is safe? | |
| Are there drug or disease state interactions? |
Conclusion
There are challenges in prescribing vitamin D and other dietary supplements, particularly for children. The OTC status of products, large number of products and suppliers, lack of oversight, and potentially inconsistent patient adherence and caregiver administration are all risk factors for harm in the form of toxicity or persistent deficiencies. Clinicians should explore patients’ knowledge, evaluate their adherence, and advocate for their patients with insurance companies to maximize effectiveness and minimize health inequities.
References
- Yang CF, Duro D, Zurakowski D, Lee M, Jaksic T, Duggan C. High prevalence of multiple micronutrient deficiencies in children with intestinal failure: a longitudinal study. J Pediatr. 2011;159(1):39-44.e1.
- Ubesie AC, Kocoshis SA, Mezoff AG, Henderson CJ, Helmrath MA, Cole CR. Multiple micronutrient deficiencies among patients with intestinal failure during and after transition to enteral nutrition. J Pediatr. 2013;163(6):1692-1696.
- Namjoshi SS, Muradian S, Bechtold H, et al. Nutrition deficiencies in children with intestinal failure receiving chronic parenteral nutrition. JPEN J Parenter Enteral Nutr. 2018;42(2):427-435.
- Stabler SP. Clinical practice. Vitamin B12 deficiency. N Engl J Med. 2013;368(2):149-160.
- Poskitt EM. Early history of iron deficiency. Br J Haematol. 2003;122(4):554-562.
- Vanderhoof JA, Langnas AN. Short-bowel syndrome in children and adults. Gastroenterology. 1997;113(5):1767-1778.
- Goulet O, Olieman J, Ksiazyk J, et al. Neonatal short bowel syndrome as a model of intestinal failure: physiological background for enteral feeding. Clin Nutr. 2013;32(2):162-171.
- Mutanen A, Mäkitie O, Pakarinen MP. Risk of metabolic bone disease is increased both during and after weaning off parenteral nutrition in pediatric intestinal failure. Horm Res Paediatr. 2013;79(4):227-235.
-
Nucci AM, Ellsworth K, Michalski A, Nagel E, Wessel J; ASPEN Pediatric Intestinal Failure Section. Survey of nutrition management practices in centers for pediatric intestinal rehabilitation. Nutr Clin Pract. 2018;33(4):528-538.
- Neelis E, Olieman J, Rizopoulos D, et al. Growth, body composition, and micronutrient abnormalities during and after weaning off home parenteral nutrition. J Pediatr Gastroenterol Nutr. 2018;67(5):e95-e100.
-
Inoue A, Itabashi K, Iwai T, Kitahara H, Watanabe Y. Imaging findings of vitamin deficiencies: are they forgotten diseases? BJR Open. 2021;3(1):20210011.
- Di Holick MF. Vitamin D: important for prevention of osteoporosis, cardiovascular heart disease, type 1 diabetes, autoimmune diseases, and some cancers. South Med J. 2005;98(10):1024-1027.
- Grenade N, Kosar C, Steinberg K, Avitzur Y, Wales PW, Courtney-Martin G. Use of a loading dose of vitamin D for treatment of vitamin D deficiency in patients with intestinal failure. JPEN J Parenter Enteral Nutr. 2017;41(3):512-516.
-
Vitamin D analogues. GoodRx. Accessed December 24, 2021. https://www.goodrx.com/vitamin-d-analogues
-
Office of Procurement, Acquisition and Logistics. Pharmacy prices. US Department of Veterans Affairs. Accessed December 24, 2021. https://www.va.gov/opal/docs/nac/fss/vaFssPharmPrices.xlsx
-
Vitamin D tests: when you need them—and when you don’t. Choosing Wisely. February 2014. Accessed January 4, 2022. https://www.choosingwisely.org/patient-resources/vitamin-d-tests/
-
Ross AC, Taylor CL, Yaktine AL, Del Valle HB, eds. Dietary Reference Intakes for Calcium and Vitamin D. National Academies Press; 2011.
-
Marcinowska-Suchowierska E, Kupisz-Urbańska M, Łukaszkiewicz J, Płudowski P, Jones G. Vitamin D toxicity—a clinical perspective. Front Endocrinol (Lausanne). 2018;9:550.
- Karaa A, Kriger J, Grier J, et al. Mitochondrial disease patients’ perception of dietary supplements’ use. Mol Genet Metab. 2016;119(1-2):100-108.
-
Riley WJ. Health disparities: gaps in access, quality and affordability of medical care. Trans Am Clin Climatol Assoc. 2012;123:167-172.
- Starr RR. Too little, too late: ineffective regulation of dietary supplements in the United States. Am J Public Health. 2015;105(3):478-485.
- Cohen PA. Assessing supplement safety—the FDA’s controversial proposal. N Engl J Med. 2012;366(5):389-391.
- Gilroy CM, Steiner JF, Byers T, Shapiro H, Georgian W. Echinacea and truth in labeling. Arch Intern Med. 2003;163(6):699-704.
-
Fox LM. Plant- and animal-derived dietary supplements. In: Nelson LS, Howland MA, Lewin NA, Smith, SW, Goldfrank LR, Hoffman RS, eds. Goldfrank’s Toxocologic Emergencies. 11th ed. McGraw-Hill Education; 2019:chap 43.
-
Tainted sexual enhancement products. US Food and Drug Administration. March 4, 2022. Accessed March 17, 2022. https://www.fda.gov/drugs/medication-health-fraud/tainted-sexual-enhancement-products
- Kurt TL, Hall AH, McKay C. ACMT position statement: dietary supplements. J Med Toxicol. 2006;2(3):116-118.
- Marcus DM, Grollman AP. The consequences of ineffective regulation of dietary supplements. Arch Intern Med. 2012;172(13):1035-1036.
-
Council for Responsible Nutrition. 2020 CRN consumer survey on dietary supplements: consumer intelligence to enhance business outcomes.
- Brown AC. An overview of herb and dietary supplement efficacy, safety and government regulations in the United States with suggested improvements. Part 1 of 5 series. Food Chem Toxicol. 2017;107(pt A):449-471.
-
USP Verified Mark. USP (United States Pharmacopeia). Accessed July 1, 2021. https://www.usp.org/verification-services/verified-mark
-
LeBlanc ES, Perrin N, Johnson JD Jr, Ballatore A, Hillier T. Over-the-counter and compounded vitamin D: is potency what we expect? JAMA Intern Med. 2013;173(7):585-586.
- Izzo AA, Ernst E. Interactions between herbal medicines and prescribed drugs: an updated systematic review. Drugs. 2009;69(13):1777-1798.
- Bush TM, Rayburn KS, Holloway SW, et al. Adverse interactions between herbal and dietary substances and prescription medications: a clinical survey. Altern Ther Health Med. 2007;13(2):30-35.
- Fugh-Berman A, Ernst E. Herb-drug interactions: review and assessment of report reliability. Br J Clin Pharmacol. 2001;52(5):587-595.
- Bazzie KL, Witmer DR, Pinto B, Bush C, Clark J, Deffenbaugh J Jr. National survey of dietary supplement policies in acute care facilities. Am J Health Syst Pharm. 2006;63(1):65-70.