Abstract
Portraits of clinicians quickly became emblematic of what the COVID-19 pandemic has demanded of everyone, especially caregivers who witnessed deaths likely unprecedented in number during their careers. This article describes an arts-based research protocol exploring portraiture as a medium for representing and understanding clinicians’ experiences, mostly during the first year of the pandemic. This article presents Shadow of Corona, a large oil on canvas portrait commissioned by the AMA Journal of Ethics to commemorate the American Medical Association’s 175th year. The article also includes Sarah, a charcoal study drawing for that portrait, and Front Lines of Care, a 3 by 3 collection of 9 smaller oil on canvas portraits.
Arts-Based Health Research
The Covid-19 pandemic has shed a harsh light upon difficulties in health decision making. Science is necessary but not sufficient to address the complexity and nuance needed to navigate an ever-evolving and uncertain climate.
Arts-based research captures what science cannot, as it seeks to depict subtle yet complex interactions, ambiguities, and vulnerabilities in a perceptible way. Art’s capacity to adumbrate—or faintly indicate, foreshadow, or symbolize—is what Barone and Eisner say allows meaning to be derived from art.1 The nuance of art invites audiences to experience the world in ways unseen or previously inaccessible.2 Portraiture, an emerging form of arts-based research, “bridge[s] the realms of science and art.”3 It seeks to study relational and aesthetic aspects of clinical interactions in medicine, such as trust, vulnerability, and reflection—qualities required for successful artist-sitter and doctor-patient interactions.4 Although portraiture is not intended as therapy, the relationship established between artist and sitter in portraiture allows the healing power of stories to be shaped and shared visually and verbally.
Sarah
Sarah was recruited as part of a convenience sample of 14 health care participants, including 5 nurses, 7 clinicians, a hospital chaplain, and a psychotherapist. Two participants were based in New York; 1 in Houston; 1 in Washington, DC; 1 in Boston; and 9 in the Midwest.
Sarah is an intensive care unit charge and rapid response nurse who has been working on the front lines of the Covid-19 pandemic in Nebraska since the beginning, all the while experiencing major life changes and caring for 4 small children. Sarah had a total of 9 portrait sessions from October 2020 to July 2021. The sessions took place in the second author’s (M.G.’s) studio, located at the University of Nebraska at Omaha. The times of the sessions varied depending on Sarah’s schedule. Portrait sittings ranged from 45 minutes to 2 hours, with most sessions lasting about an hour. Data were collected through initial interviews conducted by M.G., a final interview by the first author (B. L.), and audio recordings of all 9 portrait sessions between Sarah and M.G.
To analyze Sarah’s experience of the pandemic and participating in the portraiture study, we conducted an in-depth analysis of the data and engaged in repeated discussions of findings from multiple perspectives, a strategy known as immersion and crystallization.5 Qualitative analysis centered on Sarah’s responses to her portraits and her verbal reflections on participation in the study and working during the pandemic. Three major themes emerged from Sarah’s pandemic experiences and participation in our study: (1) confronting and overcoming uncertainty, (2) embracing vulnerability, and (3) assuaging feelings of burnout.
Overcoming Uncertainty
The COVID-19 pandemic. In this study, Sarah found some certainty at a time when uncertainty permeated everything around her—from not knowing what would happen to her patients who were “so vulnerable … and alone” to not knowing when the profound fatigue would settle in. Struggling with the lack of normal human contact and the ability to read the faces of patients, Sarah began to don the minimum required personal protective equipment (PPE) to facilitate more “human interaction vs the façade of all of the garb.” Just because patients are isolated from others does not mean they should feel isolated from their caretakers, who “become like their family,” or receive worse care. No matter the condition of patients, Sarah recognized that she has a specific “job and duty to perform care,” which drove her actions throughout the uncertainty of the pandemic. Sarah was able to confront and overcome this uncertainty because she is certain of what needs to be done as a caretaker.
The portraiture process. The creative process is inherently unpredictable for both artist and sitter. For the artist, working on the portrait is a practice of balancing observation and aesthetic striving, dialogue and silence, and uncertainty and trust.6 Neither artist nor sitter knows how the process will resolve, and it is susceptible to error and mistake. For the artist, the struggle lies in trying to represent the sitter in an intimate and real way that allows the viewer to visualize the sitter’s story. Sarah had no idea how she would be portrayed (see Figure 1) and no knowledge of arts-based research and its relation to medicine prior to this study. Sarah describes herself as “not artsy … not a fluff and rainbow person,” yet willingly shared her story and engaged with the portraiture process. Sarah yielded to the ambiguous results of the study, just as she may have accepted the ambiguous outcomes of the care she delivered to her patients. When looking back at her decision to participate, Sarah stated: “I felt like it [participation] wasn’t going to change anything because, you know, we were in the middle of the pandemic and it didn’t feel like it was going away.” However, upon completion of her participation, Sarah stated: “when I reflect upon all of the discussions and sessions and think back to where it started to where it is now, I honestly get … emotional. Because I think about when it [the study] started…. I mean I was a little bit lost in that time. It was overwhelming and there were so many unknowns.” Despite all of the unknowns she faced, Sarah surrendered to the portraiture process and was able to discover new meanings in relation to her experience, ultimately overcoming her uncertainty in a therapeutic manner.
Figure 1. Sarah, 2021

Media
Charcoal on paper, 44" x 30".
Embracing Vulnerability
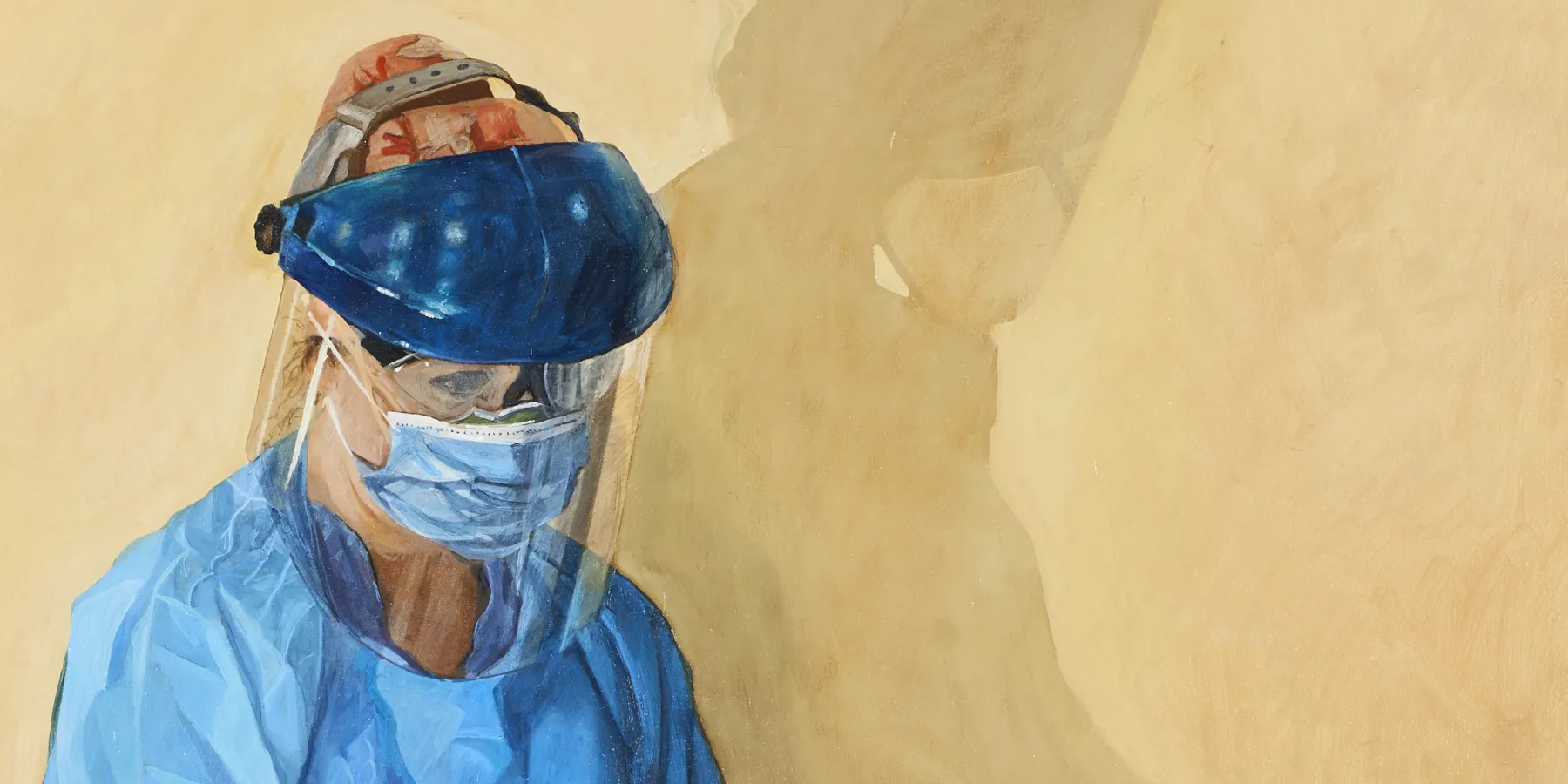
The portraiture process. Vulnerability is at the core of portraiture. The same is true in the medical setting when one is caring for or is a patient. Sarah was emotional in her interviews, which she described as “therapeutic,” because they allowed her time and space to reflect on her experiences critically and emotionally. Sarah stated that, without multiple sessions, the final portraits would “simply be a portrait and not a story to be told.” The portrait is a product of the relationship formed in the process of making it, and that relationship is simply underdeveloped after a single sitting because every interaction and connection between researcher and subject “makes the portrait come alive.” Sarah sees this depth and life in her own portrait portraying her in PPE (see Figure 2), saying:
When I look at it, and particularly my face and my eyes, I see a lot of really deep thought and like, I remember in that session I was reflecting on a lot, so as I see it progress, I think about how far it has come for me personally.… I see so many things with that picture. I see struggles and I see stress. I see that it is sad, but I also see strength with it as well, and perseverance—you know, you overcome it…. I see a lot of that in mine.
Figure 2. Shadow of Corona, 2020-2021

Media
Oil on Canvas, 58" x 56".
Moreover, Sarah stated that when she viewed other participants’ portraits in the studio, she recognized their own sadness, experiences, and perspectives, which generated a sense of fellowship that assuaged her feelings of isolation.
Burnout. Sarah believes her participation in the study played a major role in avoiding burnout during the pandemic because it increased her capacity to consider her patients’ and their families’ perspectives throughout the period of isolation. Objectivity alone can close the door to vulnerability. Perhaps this is why burnout among health care workers is so great7; emotions are not black and white like traditional scientific thinking can be. It is easier to disengage from emotions completely than to become absorbed by them. However, vulnerability invites opportunities for growth, connection, and reflection not otherwise possible. It demands a necessary balance between empathy and self-protection, which can only be achieved when invited to be practiced.
Sarah claims her participation set her apart from her coworkers in relation to burnout, saying: “I think that I am different than a lot of my peers in that [by] engaging in all of those conversations [with M.G.] … I was able to then process more in real time and I also think it helped [me] … learn how to better care for patients.” Additionally, Sarah discussed the need to put up a wall for protection of herself and patients. However, too much self-protection—to the point of desensitization—poses a threat to medical professionals and patients because it may lead to burnout and to avoidance of the vulnerability that is indispensable to the patient-clinician relationship. Instead of putting up a wall, Sarah establishes a boundary that is permeable and flexible, one that exists because she is aware of—and that enables her to reflect on—her personal biases and her patients’ wishes and beliefs. What maintains this boundary is Sarah’s compassion, which balances the objective with the subjective, or detachment with empathy.
Figure 3. Front Lines of Care

Media
Oil on canvas, 18" x 18" each.
Final Thoughts
We will all experience what it means to be a patient and a caregiver at some points in our lives. The COVID-19 pandemic has required everyone, especially frontline health care workers, to reflect on their experiences of self-care and caring for others. There is potential for fear, distress, and dissatisfaction to thrive in the midst of suffering if these experiences go unaddressed. Arts-based research is a novel approach for investigating health practitioners’ tolerance of ambiguity and the extent to which they embrace vulnerability to avoid desensitization. As discussed here, Sarah’s and others’ experiences illuminate the important role the arts can play in helping health care workers overcome uncertainty, embrace vulnerability, and assuage burnout by offering a way to better deal with ambiguity.
References
-
Barone T, Eisner EW. Arts Based Research. Sage Publications; 2011.
-
Free M. Can a “portrait” paint a thousand scholarly words? Paper presented at: Australian Council of University Art and Design Schools; September 30-October 2, 2009; Brisbane, Queensland, Australia. https://research-repository.griffith.edu.au/bitstream/handle/10072/29954/62553_1.pdf%3Bsequence=1
- Lawrence-Lightfoot S. Reflections on portraiture: a dialogue between art and science. Qual Inq. 2005;11(1):3-15.
- Gilbert MA, Lydiatt WM, Aita VA, Robbins RE, McNeilly DP, Desmarais MM. Portrait of a process: arts-based research in a head and neck cancer clinic. Med Humanit. 2016;42(1):57-62.
-
Miller WL, Crabtree BF. Clinical research. In: Denzin NK, Lincoln YS, eds. Handbook of Qualitative Research. Sage Publications; 1994:340-352.
- Aita VA, Lydiatt WM, Gilbert MA. Portraits of care: medical research through portraiture. Med Humanit. 2010;36(1):5-13.
-
Levine D. US faces crisis of burned-out health care workers. US News & World Report. November 15, 2021. Accessed March 28, 2022. https://www.usnews.com/news/health-news/articles/2021-11-15/us-faces-crisis-of-burned-out-health-care-workers
-
Eisner EW. The Arts and the Creation of Mind. Yale University Press; 2002.