Abstract
By March of 2020, the COVID-19 pandemic had changed our lives. Shadowing this pandemic is another one that adversely affects clinicians’ educations and well-being. This article features a digital photo painting and commentary.
Effects on Education
The 2020 pandemic changed the way health profession schools around the world teach knowledge and skills needed to become qualified clinicians. Most medical schools, for example, offer preclinical courses exclusively online.1 But virtual learning solutions have limitations for clinical skill building: interactions between students and real patients is irreplaceable. With shortages of personal protective equipment, clinicians are left in dire need of protection, so it was a difficult but necessary decision to temporarily suspend bedside teaching until we achieve substantial decreases in new COVID-19 case numbers per day. Despite easing some shortages in personal protective equipment, this decision to replace real-world, live, on-site, human-to-human interactions with patients and their loved ones with virtual, online learning has led to loss of opportunities to directly model human dimensions of patient care.
Effects on Residency and Fellowship Training
Most programs, especially surgical specialty training programs, have been disrupted. Despite a surge in telehealth encounters to maintain patient access to care,2 resident physicians and fellows lost opportunities to learn procedures and gain experience when the number of elective surgical procedures plummeted to prepare space for COVID-19 patients.3 Accredited programs are consequently challenged to assess their trainees’ skill development and preparedness to enter independent practice.3 Moreover, lack of social contact among trainees due to physical distancing and in-person conference cancelations also makes educational and patient care experiences less fulfilling.
Effects on Clinicians’ Well-Being
Several reports have assessed the pandemic’s influences on clinicians’ well-being.4,5,6 Psychological burdens of feeling overwhelmed, overworked, emotionally drained from losing patients or colleagues, and fearful of contracting the SARS-CoV-2 virus affect everyone, particularly nurses and physicians, who have frequent contact with patients.4 Before the pandemic’s start, the burnout rate among in-training and practicing physicians already exceeded 50%7 and is expected to increase.5,6 Witnessing patients’ deaths, losing colleagues to the disease, and social isolation at and outside work are also painful. Emotional distress also affects clinicians who are not directly involved in COVID-19 patient care and can accompany the moral distress of not being able to provide care, perhaps due to unavailability of telehealth, travel restrictions, or elective procedure deferral.
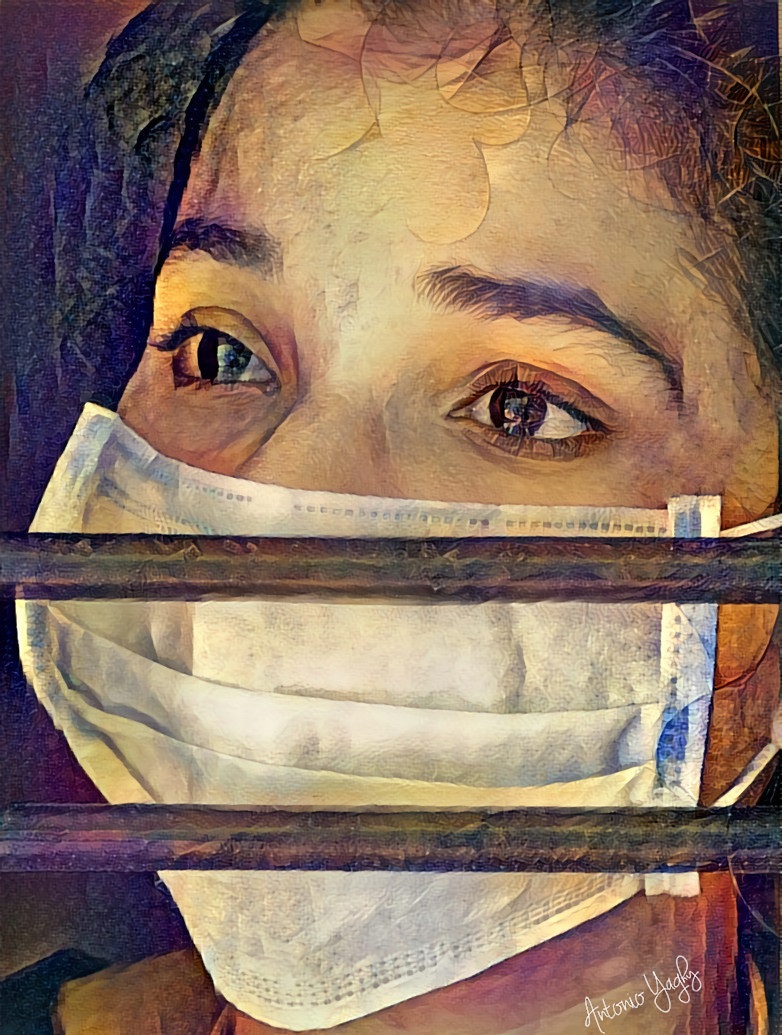
Figure. Uncertainty in Her Eyes, by Antonio Yaghy
Media
Digital photo-painting.
The woman in the image represents any clinician during pandemic times: a nurse who’s self-quarantining in her basement or garage out of fear of being an asymptomatic carrier who could transmit the virus to her loved ones, a medical student hoping to diagnose a patient, a resident on call, a fellow examining patients, or an attending physician in an intensive care unit. Two bars represent physical distancing that alone can negatively influence mental health. Although the woman is wearing a mask, one might easily recognize uncertainty and worry in her eyes.
This image not only seeks to raise awareness of the COVID-19 pandemic’s effects on clinicians, but also serves as a call to imminently address the insufficiency of clinicians’ personal protective equipment supplies and their overall well-being. National support is required for developing and integrating wellness programs that provide resources to help clinicians cope with pandemic-induced stress. Yet small actions can make big differences: be kind and acknowledge that we’re all in this together. Although smiles on mouths behind masks aren’t visible, sometimes smiles delivered with intention, sincerity, and compassion can be expressed with our eyes and be discernible.
References
-
Sandhu P, de Wolf M. The impact of COVID-19 on the undergraduate medical curriculum. Med Educ Online. 2020;25(1):1764740.
-
Perrone G, Zerbo S, Bilotta C, Malta G, Argo A. Telemedicine during Covid-19 pandemic: advantage or critical issue? Med Leg J. 2020;88(2):76-77.
- Potts JR III. Residency and fellowship program accreditation: effects of the novel coronavirus (COVID-19) pandemic. J Am Coll Surg. 2020;230(6):1094-1097.
-
Lai J, Ma S, Wang Y, et al. Factors associated with mental health outcomes among health care workers exposed to coronavirus disease 2019. JAMA Netw Open. 2020;3(3):e203976.
- Dzau VJ, Kirch D, Nasca T. Preventing a parallel pandemic—a national strategy to protect clinicians’ well-being. N Engl J Med. 2020;383(6):513-515.
- Restauri N, Sheridan AD. Burnout and posttraumatic stress disorder in the coronavirus disease 2019 (COVID-19) pandemic: intersection, impact, and interventions. J Am Coll Radiol. 2020;17(7):921-926.
- West CP, Dyrbye LN, Shanafelt TD. Physician burnout: contributors, consequences and solutions. J Intern Med. 2018;283(6):516-529.




