Abstract
Much has been written about the need for participants on global health service-learning experiences to contemplate ethical features of their involvement. This literature tends to neglect the role of self-interest in global engagement, however. This article explores how awareness of one’s own interests is critical to successfully engaging in global health experiences and proposes how US-based health professions students and trainees can practice critical self-exploration. Six themes beginning with the letter I (identity, ideology, ignorance, imagination, intention, and investment) are introduced as guides to nourish conscientious, collaborative global health learning and practice.
Global Health, Complexity, and Self-Awareness
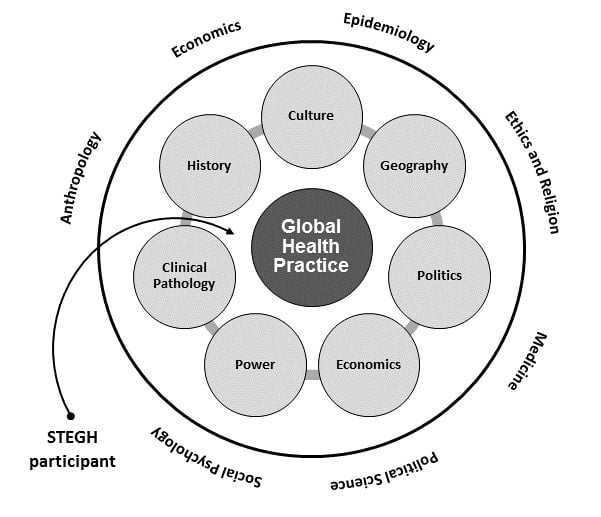
The work of global health is complex.1 It is as much about the study and application of anthropology, economics, political science, and psychology as about physiology and pharmaceuticals.2 It is as much about pathologies of power and good governance as about emerging infectious diseases.3,4,5 It is as much about relationships as about medical science.6 Opportunities for US-based health professions students and trainees to examine these complexities often come in the form of short-term experiences in global health (STEGHs)—service-learning immersions in international and domestic settings of need (see Figure 1).
Figure 1. Complexity in Global Health Practice—Representative Considerations and Areas of Study for Participants/Learners on STEGHs
Much has been written about the need for participants in service-learning experiences to contemplate the ethics of their involvement,7,8,9 but this focus commonly ignores the ways in which self-awareness is integrally intertwined with the concept of global health.10 Self-awareness is the ability to recognize and appreciate one’s perspectives—understandings, values, and biases—in relation to the complicated interpersonal and material worlds in which one lives.11 These perspectives are borne of experiential histories and acquired knowledge that give meaning to thoughts and actions.12 Insofar as STEGHs expose students and trainees to clinical and cultural environments markedly different than those to which they are accustomed, STEGHs create opportunities to cultivate self-awareness and, ultimately, foster mutually beneficial relationships that are relatively free of exploitation.
Absent self-awareness, US health professions students and trainees on STEGHs can project cultural insensitivity,13 act in ways that perpetuate patterns of domination,14 or unwittingly sabotage well-laid plans for implementing appropriate health care interventions.15 They could also underestimate the difficulty of creating equitable partnerships and promoting social change given significant differences in power, capital, and culture that exist around the world.16 Indeed, for students and trainees on STEGHs, self-awareness can be a defense against cultural ignorance or a lack of empathy and can help foster global humility.17
Nonetheless, simply participating in a STEGH does not guarantee growth in self-awareness and may even reinforce harmful preconceptions and prejudices. Pre- and post-STEGH educational sessions can help ameliorate such untoward consequences,18 just as writing narrative essays and attending to ethical guidelines for global health experiences can aid in personal and professional development.19,20,21,22,23 However, the key to growing self-awareness in relation to global health is critical self-exploration—the mindful, imaginative, and enduring practice of identifying and challenging one’s assumptions and actions in light of new information arising from exposure to new surroundings and the passage of time.24,25,26 On the basis of my more than 30 years’ work as a clinician-educator serving in US safety-net clinics and on several international engagements, I contend that developing self-awareness by practicing critical self-exploration is crucial for health professions students and trainees taking part in STEGHs.27
To encourage activities aimed at critical self-exploration in the context of STEGHs, I suggest 6 themes for use as reflective prompts: identity, ideology, ignorance, imagination, intention, and investment. These themes have emerged from experiences and conversations I have had and observations I have made along my professional path.
I-Themed Reflections for Global Health Immersions
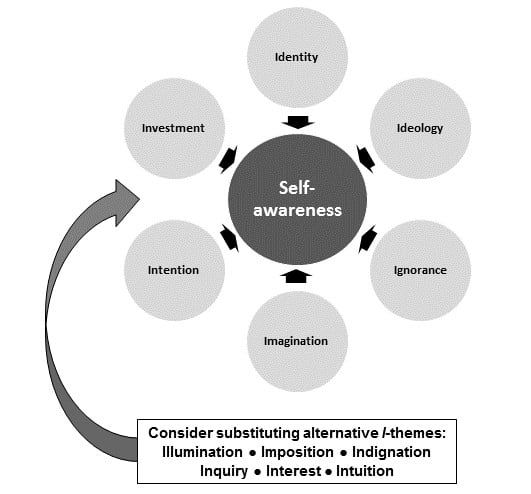
Each theme begins with the letter I to emphasize self-reflection as a critical component of professional development,28 cultural competency,29 and the transmission of knowledge30 (see Figure 2). Each builds on the concept of social construction,31 the idea that what we authentically bring to interpersonal encounters and how we interact in these encounters help us learn both individually and in community with others.32 Each theme is paired with several self-reflective questions informed by the framework of appreciative inquiry, an asset-based approach that promotes successful interactions in challenging environments.33
Figure 2. I-Themes for Developing Self-awareness as Participants in Short-term Global Health Experiences
Identity. Identity can be defined as the distinguishing character or personality of an individual. In the context of STEGHs, identity is linked to one’s relational “footprint” and, accordingly, encompasses such interpersonal qualities as reciprocity, generosity, and presence.34 In the context of global health, questions that speak to building and maintaining an authentic identity35 that fosters the compassion and insight essential to equitable, collegial, and supportive relationships include the following:
- How has my global health work informed who I am as an individual, as a member of a professional community, and as a representative of the larger community in which I live?
- What have I learned, what am I continuing to learn, and what do I anticipate learning in the future?
- How might I mentor others as they progress down their own paths of learning?
- How can I work to recognize the authentic identity of other people in their home settings?
Ideology. Ideology can be defined as a system of beliefs that prescribe how people in a group are typically expected to act. Ideologies are typically religious, economic, or political in nature and may manifest as projections of power.36 Across boundaries of culture and geography, ideologies often compete with each other. As such, it is worthwhile to ask the following questions:
- What ideologies, explicit or implicit, drive my motivations?
- How do I express the ideologies I hold in settings both similar to and different from those to which I am most accustomed?
- How might I open myself up to inquiring about and identifying the ideologies that guide others’ behaviors?
- Once these ideologies are identified, how might I work to comprehend the reasons they exist as important aspects of peoples’ lives?
Ignorance. Ignorance is a lack of information or the state of being uninformed. It is a major factor in people’s inability to appreciate how societal forces create and perpetuate adverse social determinants such as poverty,37 racism,38 gender discrimination,39 and globalization.40 The following 4 questions can help circumscribe the limits of one’s knowledge and awareness.
- How do I react when I realize I do not know something important?
- What interpersonal challenges am I encountering vis-à-vis the people with whom I am working, and how might these challenges encourage me to identify and examine my own implicit biases?
- What have I learned that I did not previously know?
- How shall I make use of my new understandings in service to others as I develop my own global fluency?
Imagination. Imagination can be defined as the ability to be creative and resourceful or as the capacity to use creativity in the service of adaptability. Both traits are essential in many areas of the world where accessible medical care is lacking. This reality suggests 4 questions:
- What is it like to practice as a local health professional in this setting?
- What do characteristics such as competency and usefulness look like here, based on the local, resource-limited circumstances that exist?41
- Can I imagine what it would be like to walk in the shoes of the people who live here continuously?
- What would it mean for us to work with, and not just for, others—wherever we are, with whatever we have, in the moment at hand?42
Intention. Intention can be defined as the purpose that underlies actions. It includes aspects of forethought and planning as part of the process that moves people to act. Exploring one’s intention in participating in STEGHs is especially important for positioning one’s objectives on the spectrum between learning and service (ie, between enhancing open-minded understanding and achieving purposeful outcomes). Intention suggests several questions, especially when one is faced with clinical concerns beyond the scope of one’s previous training.
- Why am I doing this work?
- What do I hope to get out of it?
- Whom does it primarily serve?
- What effects of my interactions here will reverberate into the future?
Investment. Investment can be defined as devoting time, effort, and energy to undertakings with the expectation of worthwhile results. Expectations of STEGHs vary, depending on how much one is willing and able to contribute. Reasonable questions include the following:
- Am I dedicated to working overtime in service of reducing the social inequities that undergird unequal outcomes in health and illness?
- How can I balance my needs for personal exploration and professional gratification with the acknowledged needs of others?
- If my efforts involve a long-term commitment, how might I share the success of my work with others, especially with colleagues who, by necessity, live and work in areas of need?43
Further Considerations
The use of these I-themed questions to promote self-awareness is appropriate before, during, and after participation in STEGHs. As with any educational activity that may well touch on emotional issues, care must be taken to create a safe space for learners to disclose deeply personal concerns.44 Many pedagogical modalities—among them narrative writing exercises,45 prospective case-study discussions,46 presentation of relevant movies or film clips,47 and even interactive online courses48—can be used to initiate self-exploration using the above questions. However, simply encouraging STEGH participants to share their personal reflections as they arise may be the most effective method to stimulate the growth of self-awareness.49 Such critical incident learning, cultivated by STEGH participants’ sense of curiosity, suspension of immediate judgment, and mindful attention to experience,50 can occur individually with supportive mentors or in groups with peers.
Of vital importance, these I-themes should neither be perceived as simply an inventory of competencies to be acquired nor taught as bullet points for rote acquisition.51,52 Coupled with an inquisitive stance vis-à-vis other people,53 they are prompts to learning through emergent reflection. Furthermore, they should not be seen as comprehensive in scope. Other I-themes are equally suitable (eg, illumination, imposition, indignation, inquiry, interest, or intuition), and non-I words pose assorted alternative themes for further inspiration. Lastly, none of the I-themes concerns solely international initiatives. Students and trainees might substitute local for global and consider how their points of view shape their personal and professional formations at home.17
Conclusion
STEGHs are one way for US health professions students and trainees to begin to appreciate the complex nature of the work of global health. By developing self-awareness through critical self-exploration, budding health professionals can maximize their ability to learn—conscientiously, collaboratively, and constantly—about this complexity. My hope is that these I-themes and corresponding questions will help participants in STEGHs in this endeavor, which is essential to enriching global health practice and advancing the health of the public.
References
- Leon JS, Winskell K, McFarland DA, del Rio C. A case-based, problem-based learning approach to prepare master of public health candidates for the complexities of global health. Am J Public Health. 2015;105(suppl 1):S92-S96.
-
Nichter M. Global Health: Why Cultural Perceptions, Social Representations, and Biopolitics Matter. Tucson, AZ: University of Arizona Press; 2008.
-
Farmer P. Pathologies of Power: Health, Human Rights, and the New War on the Poor. Berkeley, CA: University of California Press; 2003.
- Frenk J, Moon S. Governance challenges in global health. N Engl J Med. 2013;368(10):936-942.
- Vouga M, Greub G. Emerging bacterial pathogens: the past and beyond. Clin Microbiol Infect. 2016;22(1):12-21.
- Ventres WB. The joys of global medicine and the lesson of relationship. Am J Med. 2016;129(8):771-772.
-
Farmer P, Kleinman A, Kim J, Basilico M. Reimagining Global Health: An Introduction. Berkeley, CA: University of California Press; 2013.
- Pinto AD, Upshur REG. Global health ethics for students. Dev World Bioeth. 2009;9(1):1-10.
- Abdulaimi S, McCurry V. Ethical considerations when sending medical trainees abroad for global health experiences. Ann Glob Health. 2017;83(2):356-358.
- Abedini NC, Gruppen LD, Kolars JC, Kumagai AK. Understanding the effects of short-term international service-learning trips on medical students. Acad Med. 2012;87(6):820-828.
- Epstein RM. Mindful practice. JAMA. 1999;282(9):833-839.
-
Ventres WB, Fort MP. Eyes wide open: an essay on developing an engaged awareness in global medicine and public health. BMC Int Health Hum Rights. 2014;14(1):29.
- Bleakley A, Brice J, Bligh J. Thinking the post-colonial in medical education. Med Educ. 2008;42(3):266-270.
- Finnegan A, Morse M, Nadas M, Westerhaus M. Where we fall down: tensions in teaching social medicine and global health. Ann Glob Health. 2017;83(2):347-355.
- Shiffman J. Global health as a field of power relations: a response to recent commentaries. Int J Health Policy Manag. 2015;4(7):497-499.
- Ventres WB. Intentional exploration on international service learning trips: three questions for global health. Ann Glob Health. 2017;83(3-4):584-587.
-
Ventres W, Wilson B. Rethinking goals: transforming short-term global health experiences into engagements. Acad Med. In press.
-
EIESL Project. EIESL (Ethics of International Engagement and Service-Learning) Project. http://ethicsofisl.ubc.ca/?page_id=65. Accessed November 24, 2018.
- Peluso MJ, Encandela J, Hafler JP, Margolis CZ. Guiding principles for the development of global health education curricula in undergraduate medical education. Med Teach. 2012;34(8):653-658.
-
Crump JA, Sugarman J; Working Group on Ethics Guidelines for Global Health Training (WEIGHT). Ethics and best practice guidelines for training experiences in global health. Am J Trop Med Hyg. 2010;83(6):1178-1182.
-
DeCamp M, Rodriguez J, Hecht S, Barry M, Sugarman J. An ethics curriculum for short-term global health trainees. Global Health. 2013;9:5.
- Melby MK, Loh LC, Evert J, Prater C, Lin H, Khan OA. Beyond medical “missions” to impact-driven short-term experiences in global health (STEGHs): ethical principles to optimize community benefit and learner experience. Acad Med. 2016;91(5):633-638.
-
DeCamp M, Lehmann LS, Jaeel P, Horwitch C; ACP Ethics, Professionalism and Human Rights Committee. Ethical obligations regarding short-term global health clinical experiences: an American College of Physicians position paper. Ann Intern Med. 2018;168(9):651-657.
- Aronson L. Twelve tips for teaching reflection at all levels of medical education. Med Teach. 2011;33(3):200-205.
- Jayatilleke N, Mackie A. Reflection as part of continuous professional development for public health professionals: a literature review. J Public Health (Oxf). 2013;35(2):308-312.
- Aronowitz R, Deener A, Keene D, Schnittker J, Tach L. Cultural reflexivity in health research and practice. Am J Public Health. 2015;105(suppl 3):S403-S408.
- Neill KG. In the shadow of the temple: cross-cultural sensitivity in international health program development. Ethn Health. 2000;5(2):161-171.
- Wald HS. Professional identity (trans)formation in medical education: reflection, relationship, resilience. Acad Med. 2015;91(6):701-706.
- Lie D, Shapiro J, Cohn F, Najm W. Reflective practice enriches clerkship students’ cross-cultural experiences. J Gen Intern Med. 2009;25(suppl 2):119-125.
- Lockyer J, Gondocz ST, Thivierge RL. Knowledge translation: the role and place of practice reflection. J Contin Educ Health Prof. 2004;24(1):50-56.
- Launer J. A social constructivist approach to family medicine. Fam Syst Health. 1995;13(3-4):379-389.
- Philpott J, Batty H. Learning best together: social constructivism and global partnerships in medical education. Med Educ. 2009;43(9):923-924.
-
Frankel R, Beyt G. Appreciative inquiry: fostering positive culture. American Medical Association. https://edhub.ama-assn.org/steps-forward/module/2702691. Accessed February 21, 2019.
- Ventres WB. Global family medicine: a “UNIVERSAL” mnemonic. J Am Board Fam Med. 2017;30(1):104-108.
- Kreber C, Klampfleitner M, McCune V, Bayne S, Knottenbelt M. What do you mean by “authentic”? A comparative review of the literature on conceptions of authenticity. Adult Educ Q. 2007;58(1):22-43.
- Brunger F. Guidelines for teaching cross-cultural clinical ethics: critiquing ideology and confronting power in the service of a principles-based pedagogy. J Bioeth Inq. 2016;13(1):117-132.
-
Walraven G. Health and Poverty: Global Health Problems and Solutions. London, UK: Earthscan; 2011.
- Jones CP. Levels of racism: a theoretic framework and a gardener’s tale . Am J Public Health. 2000;90(8):1212-1215.
-
Phillips SP. Defining and measuring gender: a social determinant of health whose time has come. Int J Equity Health. 2005;4(1):11.
- Labonté R, Mohindra K, Schrecker T. The growing impact of globalization for health and public health practice. Annu Rev Public Health. 2011;32(1):263-283.
- Epstein RM, Hundert EM. Defining and assessing professional competence. JAMA. 2002;287(2):226-235.
-
Ventres W, Haq C. Toward a cultural consciousness of self in relationship: from “us and them” to “we.” Fam Med. 2014;46(9):691-695.
-
Ventres WB, Wilson CL. Beyond ethical and curricular guidelines in global health: attitudinal development on international service-learning trips. BMC Med Educ. 2015;15(1):68.
- Edmunds S, Brown G. Effective small group learning: AMEE Guide No. 48. Med Teach. 2010;32(9):715-726.
- Curtin AJ, Martins DC, Schwartz-Barcott D, DiMaria LA, Ogando BM. Exploring the use of critical reflective inquiry with nursing students participating in an international service-learning experience. J Nurs Educ. 2015;54(9):S95-S98.
- Stewart KA. Teaching corner: the prospective case study: a pedagogical innovation for teaching global health ethics. J Bioeth Inq. 2015;12(1):57-61.
- Blasco PG, Mônaco CF, De Benedetto MA, Moreto G, Levites MR. Teaching through movies in a multicultural scenario: overcoming cultural barriers through emotions and reflection. Fam Med. 2010;42(1):22-24.
-
Jacquet GA, Umoren RA, Hayward AS, et al. The Practitioner’s Guide to Global Health: an interactive, online, open-access curriculum preparing medical learners for global health experiences. Med Educ Online. 2018;23(1):1503914.
- Branch WT Jr. Use of critical incident reports in medical education. A perspective. J Gen Intern Med. 2005;20(11):1063-1067.
- Epstein RM, Siegel DJ, Silberman J. Self-monitoring in clinical practice: a challenge for medical educators. J Contin Educ Health Prof. 2008;28(1):5-13.
- Seibert PS, Stridh-Igo P, Zimmerman CG. A checklist to facilitate cultural awareness and sensitivity. J Med Ethics. 2002;28(3):143-146.
- Eichbaum Q. Acquired and participatory competencies in health professions education: definition and assessment in global health. Acad Med. 2017;92(4):468-474.
- Ventres W, Crowder J. When I say … anthropological gaze. Med Educ. 2018;52(6):590-591.




