There's been a quiet revolution over the past dozen years in the way patients are cared for in hospitals. Its outcome is the growing presence of the hospitalist—a physician whose focused area of practice is caring for patients while they are hospitalized. Hospitalist management of inpatient care means fewer visits to the hospital by the patient's office-based, primary care physician. In some regions and hospital systems, so-called “outpatient” physicians transfer care of their patients to the new inpatient specialists the minute the patient becomes hospitalized and resume care when the patient is discharged.
The several efficiency- and patient safety-related reasons for the revolution are well documented in this month's Virtual Mentor. (No one mentions that central casting challenges and plot stability demands drove daytime drama to invent the hospitalist quite some time ago. The de facto hospitalist appeared on General Hospital before he showed up at Mass. General.)
The questions of greatest interest to this month's contributors concern the effect of the new model of hospital medicine on patients. Have patients lost something critical to their well-being now that their own primary care physicians do not stop in to visit once or twice a day? Is the loss more than offset by gains in safety and shortened length of hospital stay? What sort of relationship is possible between the patient and hospitalist, who has the best interest of many patients on his or her mind at the same time? Finally and importantly, how do these new focused-practice physicians relate professionally to their patients' primary care physicians, and how do they demonstrate to their profession and the public that they have the special knowledge and skills needed to care for people who are very sick?
In VM's first clinical case, two physicians, a hospitalist and a primary care physician, differ on a patient's treatment plan. Commentator Dawn Brezina, a hospitalist and educator at Duke University Health System, explains that hospitalists must constantly be on guard against conflict between the interests of the patient and those of the hospital, since a compromise in treatment plan may be a breach of obligations to the patient.
The next clinical case examines the new questions in professional relationships introduced by the hospitalist movement. When both hospitalist and family physician are involved, who is better suited to initiate a discussion about end-of-life issues? Mary Ehlenbach argues that the hospitalist may have greater skill in conducting such intense conversations, but she acknowledges and welcomes the participation of a family physician who has a long and close association with the patients who are facing the difficult decision.
Laborists, a subset of hospitalists, are the subjects of clinical case three. Laborists' expertise can add to patient safety in many labor and delivery cases, but they have “a duty to preserve the established relationship between the treating obstetrician and patient.” By doing so, Louise P. King and George D. Wendel Jr. maintain, laborists can preserve continuity of care even in emergent situations.
How do hospitalists demonstrate their competence? Jeffrey G. Wiese, a medical educator at Tulane University, explains the effort under way to assure that all hospitalists are trained to high standards. A “focused-practice certification” is planned by the American Board of Medical Specialties, the main tenets of which are that “physicians must (1) demonstrate competence as internists, and (2) have practice experience in hospital medicine.”
Robert M. Wachter is, by all accounts, a founder of the field. He summarized the key developments in hospital medicine in his 2008 article, The State of Hospital Medicine in 2008, which is reviewed by AMA intern Chloe White in this month's journal discussion.
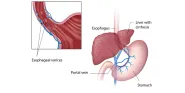
The clinical pearl guides us through the benefits and limitations of transjugular intrahepatic portosystemic shunts (TIPS) in treating portal hypertension—the source of controversy in clinical case one. A physician training to be a transplant hepatologist, Elizabeth C. Verna encapsulates the most important indications and counterindications for use of this procedure.
In the health law article, Erin A. Egan uses Domby v. Moritz to show how the limits of hospitalists' liability are being defined—a vital step if this medical model is to survive legal challenges.
If hospitalists are so great, why not make their use mandatory? In this month's policy forum, Marc B. Royo, Laura L. Kimberly, and Alexandria Skoufalos, all from Jefferson Medical College of Thomas Jefferson University, in Philadelphia, explore why this option was tried in some places and then modified in the course of the field's evolution.
How far can the hospitalist concept go? C. Edward Wells confides the concerns that laborists—hospitalists who oversee labor and delivery—have about patient acceptance of their role, new in the past five years, in one of this month's history of medicine articles.
Another historical look highlights the rapid evolution of hospitalist medicine as a “site-of-care” specialty—a rise far more rapid than that of emergency medicine, the other well-known example of site-specific practice. Joseph Ming Wah Li explains the two key reasons for its birth and growth: efficiency and patient safety.
In the medicine and society section, Elmer Abbo discusses the new paradigm of health care delivery. He argues that physicians who practice in hospitals day in and day out are best positioned to mediate the inevitable conflict between an individual patient's needs and scarce resources. Dr. Abbo views the model of hospitalist medicine as central to a realistic medical ethics in our health care system.
While the profession has become accustomed to working with these new colleagues in the hospitalist field, there's still an element—part nostalgia, part unease—that says, “Something's not right. What happened to the old-time family doctor?” Robert M. Centor writes an op-ed article on the adjustments that are yet to be made. “I have heard tales of horrible hospitalists with lousy bedside manners. I have heard praise for wonderful hospitalists with superb bedside manners.” He is well placed to comment, having made the transition to hospital-based medicine himself.
We hope that this issue of Virtual Mentor helps readers understand the causes, outcomes, and ethical concerns raised by a revolution in hospital medicine so quiet that many may have not known it was occurring. Finally, we thank Erin A. Egan for the idea that led to this theme issue.