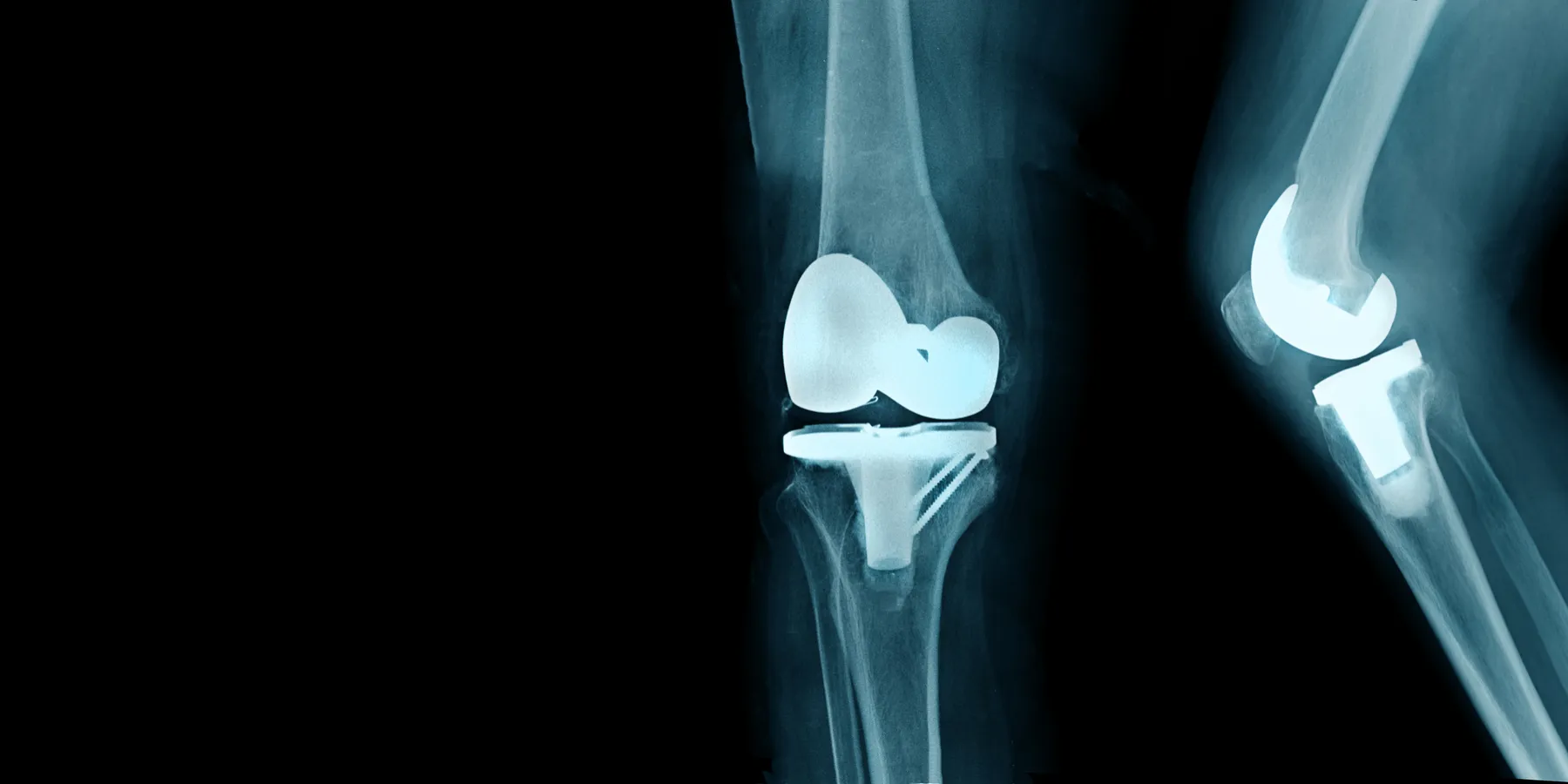
Total joint arthroplasties are a common and effective treatment for end-stage osteoarthritis. In the United States alone, there are more than 200,000 such primary total hip replacements done each year for those older than 80 years [1], and the number is expected to reach 600,000 annually by the year 2030 [2]. The exponential rise in primary arthroplasties is expected to double the number of revision surgeries in the next two decades [3, 4]. This anticipated rise in caseloads and the use of new, evolving implant technology demand a reliable and objective method of monitoring and feedback.
Outside the U.S., such monitoring and feedback already exist in the form of national joint registries. The Swedish Knee Register, established in 1976, was the first, followed by the Swedish Hip Register in 1979 [5, 6]. Since the early 1980s, a host of national registries have been established in Europe, Canada, and Australia. Registries like the Nordic Arthroplasty Registry Association are now expanding past the traditionally national scope [7]. Efforts are underway to launch an American National Joint Registry in the summer of 2010.
Registries thus far have proven to be powerful surveillance systems, improving outcomes and cost-effectiveness for total joint replacement surgeries. Effective registries provide: (1) timely feedback to surgeons and industry; (2) a sentinel for complications; (3) a reduction in patient morbidity; (4) the monitoring of new surgical techniques and implant technology; and (5) indications of poor implant design [8].
The Components of a Registry
Over time, it has become clear that there are four essential components of the successful registry: (1) organizational control and funding; (2) participation on the part of surgeons and hospitals; (3) data management; and (4) a mechanism for timely feedback.
Most registries are run by national orthopaedic associations, and are funded by their respective national governments [9]. Widely considered successful, the Swedish Hip Registry is owned by the Swedish Orthopaedic Association, and financed by Sweden’s Board of Health and Welfare. On the other hand, the National Joint Registry of England and Wales is managed (and funded) by the United Kingdom Atomic Energy Authority. Not surprisingly, there is local concern for the lack of joint replacement expertise and surgeon representation on its steering committee, and the overwhelming wish of the U.K.’s orthopedic community is to have a surgeon-run national registry [10]. Obviously, adequate funding of a registry is also critical to survival. The German National Registry, which was initially financed by industry and surgeons, eventually succumbed to a lack of private funds [9]. It therefore appears that long-term success of any registry would require the stable funding afforded by government in one way or another.
Participation in a registry by surgeons and hospitals has generally been voluntary. Expert consensus in fact recommends that the participation rate be at least 85 percent so data are not skewed by unreported revisions or complications [8]. The voluntary system may allow participation rates to be low, as is the case in Canada, which is not ideal. In Finland, Slovakia, and Denmark, however, participation is mandated by law [9].
Data management involves collection, validation, and analysis. Data are collected prospectively, and usually submitted via electronic means. Information would, for example, include a patient identifier, surgeon identifier, date of operation, diagnosis, procedure, surgical approach, and implant specifications [9]. Currently, revision surgery is the main indicator of failure of the primary procedure in most registries [8]. There is now a movement to include patient-derived outcomes data along with radiographic details to help improve the sensitivity of assessment.
Needless to say, the utility of the registry data depends on its accuracy and completeness. Validation exercises suggest that there may be an error rate of about 1 percent in recording surgery dates and sites of implant [11]. Thus, at every stage of data collection and entry, there need to be mechanisms for regular validation in order to minimize error propagation. Once the data are stored, qualified personnel need to test the external validity of these data cross-sections, and put quality control mechanisms in place prior to analysis. Data are normally presented as survival analyses with time to first revision, and analyzed using Kaplan-Meier statistical methods [8].
Though registries serve multiple functions, a national registry’s primary objective is to inform surgeons, industry, and the lay public about the performance of different surgical techniques and implant designs. This process is intended to promote best practices and evidence-based medicine by presenting objective and unbiased information. It is important that underperformers not perceive negative feedback as punitive, but rather as constructive, with the shared goal of improving patient outcomes in mind. Most reports are compiled annually and published in peer-reviewed journals, and are accessible via the Web sites of the various national joint registries themselves [9, 12].
With new and evolving implant technology, a national registry represents a powerful surveillance system for quality control. The response to lipid contamination of Sulzer Orthopaedic components in 2000 is a prime example of this process [13]. There were 17,500 contaminated Sulzer total hip arthroplasty components implanted in the U.S., 3,000 of which were later revised. By contrast, as explained in a 2002 conversation with Dr. Henrik Malchau, Swedish surgeons were notified by their registry of the unacceptably high failure rate at about the same time, and the implants were discontinued after only 30 were used (with 5 patients later requiring revision surgery).
Registry feedback has also had a tremendous impact on the use of hip resurfacing in Australia. Beginning in the late 1990s there was a resurgence in its use (especially for patients younger than 55 years old), and the procedure accounted for almost 10 percent of all arthroplasties done in 2006 [14]. The survival of these metal-on-metal bearing implants was followed closely by the national registry, and it was noted that women who had had resurfacing were twice as likely to have revision surgery as women who had had conventional total hip replacement (i.e., 4.2 percent versus 2.0 percent). Because information about the gender-related failure and increased revision risk was disseminated quickly, there has been an overall decline in the use of resurfacing in Australia; particularly on women (from 28.8 percent in 2007 to 23.6 percent in 2009) [15].
Feedback has also been a catalyst for improvement programs. One local hospital was identified by the Swedish Hip Registry in 2005 as having an unacceptably high revision rate due to dislocation (4.8 percent, as opposed to the national average, 1.4 percent) [16]. A site-specific program was immediately implemented to improve patient education, patient selection, and pre-operative templating and to increase the use of cup-positioning instrumentation, use of larger femoral heads, and capsular and piriformis tendon repair for the posterior surgical approach. There have been no revisions due to recurrent dislocation since 2006. As a matter of fact, it has been surmised that the Swedish Hip Registry has helped to reduce Sweden’s national revision burden by 2.5 times (from 17 percent in 1979 to 7 percent in 1997) [17].
Socioeconomic Implication
The economic burden of revision surgery is significantly lower in countries with registries, such as Sweden, than in the United States, which does not yet have a national registry. There was a 16.9 percent revision rate in the U.S. from 1992 to 2000 for patients who were older than 65 years and had had a primary total hip replacement [1]. At the same time in Sweden, there was a revision rate of only 6.4 percent for the same demographic group. Each percentage point reduction in revision surgeries saves an estimated $42.5 million to $112.6 million annually [1]. A 10 percent reduction in the U.S. revision rate would approach Swedish standards and could save upwards of $1 billion each year.
Figures also indicate that most hip arthroplasties in the U.S. are done by surgeons who do fewer than 20 such procedures per year [18]. The majority of all revision procedures are performed in centers that have fewer than 10 revisions annually [18]. Most arthroplasty research and outcomes studies, however, are conducted by surgeons who perform many replacement procedures in tertiary or quaternary centers. The patient outcome in these centers may not necessarily reflect the average outcome across the nation. A national registry would help identify unsafe outliers in the system.
Conclusion
These data strongly suggest that the presence of national joint registries has had a positive effect on overall outcomes for arthroplasty patients. The regular feedback has provided information to surgeons, industry, and the lay public regarding the performance of various surgical techniques, implant designs, and associated complications. Registries have also been a critical sentinel, warning of early implant failure and potential harm. Valuable demographic information on patients has helped determine current and future needs of the population. The demand for both primary and revision arthroplasty surgery are only expected to rise in the future, and national registries will help ensure that evidence-based best practices and technology are allowed to flourish.
References
- Kurtz S, Mowat F, Ong K, et al. Prevalence of primary and revision total hip and knee arthroplasty in the United States from 1990 through 2002. J Bone Joint Surg Am. 2005;87(7):1487-1497.
- Kurtz S, Ong K, Lau E, et al. Projections of primary and revision hip and knee arthroplasty in the United States from 2005 to 2030. J Bone Joint Surg Am. 2007;89(4):780-785.
- Kurtz SM, Lau E, Ong K, et al. Future young patient demand for primary and revision joint replacement: national projections from 2010 to 2030. Clin Orthop Relat Res. 2009;467(10):2606-2612.
- Bozic KJ, Kurtz SM, Lau E, et al. The epidemiology of revision total hip arthroplasty in the United States. J Bone Joint Surg Am. 2009;91(1):128-133.
-
Herberts P, Ahnfelt L, Malchau H, et al. Multicenter clinical trials and their value in assessing total joint arthroplasty. Clin Orthop Relat Res. 1989;(249):48-55.
-
Ahnfelt L, Herberts P, Malchau H, Andersson GB. Prognosis of total hip replacement: a Swedish multicenter study of 4,664 revisions. Acta Orthop Scand Suppl. 1990;238:1-26.
-
Havelin LI, Fenstad AM, Salomonsson R, et al. The Nordic Arthroplasty Register Association: a unique collaboration between 3 national hip arthroplasty registries with 208,201 THRs. Acta Orthop. 2009;80(4):393-401.
-
Von Knoch F, Malchau H. Why do we need a national joint replacement registry in the United States? Am J Orthop (Belle Mead, NJ). 2009;38(10):500-503.
- Kolling C, Simmen BR, Labek G, Goldhahn J. Key factors for a successful National Arthroplasty Register. J Bone Joint Surg Br. 2007;89(12):1567-1573.
- Philipson MR, Westwood MJ, Geoghegan JM, et al. Shortcomings of the National Joint Registry: a survey of consultants' views. Ann R Coll Surg Engl. 2005;87(2):109-112.
- Arthursson AJ, Furnes O, Espehaug B, et al. Validation of data in the Norwegian Arthroplasty Register and the Norwegian Patient Register: 5,134 primary total hip arthroplasties and revisions operated at a single hospital between 1987 and 2003. Acta Orthop. 2005;76(6):823-828.
-
Joint Replacement Unit, Sahlgrenska University Hospital, Goteborg University. http://www.jru.orthop.gu.se. Accessed January 15, 2009.
-
Lefevre G. Hip replacement patients may face more surgery: 17,500 hip units recalled. CNN. January 17, 2001. http://archives.cnn.com/2001/HEALTH/01/17/hip.replacement/index.html. Accessed June 23, 2009.
- Buergi ML, Walter WL. Hip resurfacing arthroplasty: the Australian experience. J Arthroplasty. 2007;22(7 Suppl 3):61-65.
-
Australian Orthopaedic Association. 2009 Annual Report: Hip and Knee Replacement. Sydney, Australia: Australian Orthopaedic Association; 2009.
-
Karrholm J, Garellick G, Herberts P. Swedish Hip Arthroplasty Register: Annual Report 2006. Gothenburg, Sweden: Sahlgrenska University Hospital; 2007.
-
Herberts P, Malchau H. How outcome studies have changed total hip arthroplasty practices in Sweden. Clin Orthop Relat Res. 1997;(344):44-60.
- Katz JN, Losina E, Barrett J, et al. Association between hospital and surgeon procedure volume and outcomes of total hip replacement in the United States medicare population. J Bone Joint Surg Am. 2001;83(A 11):1622-1629.