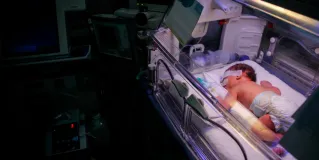
Iatrogenesis in Pediatrics
Despite best efforts to do no harm, clinicians should be prepared to respond to patients who experience adverse outcomes of even the best health care. Often thought to refer only to medical error, iatrogenesis characterizes a wider range of possible health care outcomes that are, as the Greek etymology suggests, physician generated. Iatrogenic consequences can be side effects from medications, surgical complications, traumatic stress from specific health care experiences, or failure to provide necessary care. Iatrogenic outcomes are particularly fraught in pediatrics, due to children’s inherent vulnerability as patients who typically lack decision-making authority. This month’s issue of the AMA Journal of Ethics grapples with neglected clinical and ethical questions about pediatric iatrogenesis, including how clinicians communicate iatrogenic risks to patients’ parents or guardians, how clinicians manage therapies with inevitable iatrogenic harms, and how clinicians might consider, respond to, and mitigate iatrogenic consequences of their practices.