Case
Mrs. Brown, who is 35 years old, has a BMI of 37. Her father struggled with diabetes mellitus type 2 for 30 years. She was his sole caretaker, nursing him through complications of peripheral neuropathy and helping him to complete his tasks of daily living after a leg amputation. Recently, he went into renal failure and died. Mrs. Brown also has a 45-year-old brother and several other first-degree relatives who have diabetes type 2 and are insulin dependent. Mrs. Brown confided her worries to her physician and was referred to a bariatric surgeon for a consultation. She says that she has worked with nutritionists and tried to exercise more, but her efforts have not been successful over the long term. Determined to avoid becoming a diabetic, she would like to have bariatric surgery. The surgery cured her friend’s diabetes. With a BMI of 37 and no obesity-related diseases, Mrs. Brown does not qualify as a candidate for the surgery under the current guidelines. But were she either to gain weight (raising her BMI to 40) or develop diabetes (a condition which would lower the recommended BMI to 35), she would qualify for the intervention. She understands that insurance is not likely to cover the procedure, but money is not an obstacle. What should the consulting surgeon say to Mrs. Brown?
Commentary 3
Even after a lengthy debate between bioethicists, physicians and surgeons and a plethora of publications, there currently are no formal, federal regulations that apply specifically to surgical innovation [1-3]. Consequently, the gap between regulatory goals and professional reality still exists, and as some argue, is widening due to increasing call for evidence-based surgery [4].
To close the reported gap between research idealism and surgical innovation, several authors have presented solutions to this ethical challenge. Recently published recommendations from a multidisciplinary group, which included both surgeons and bioethicists, put forth some specific and detailed guidelines for surgical innovators [3]. These guidelines were designed to help surgeons determine at what point their efforts to improve their operative techniques and therapies become innovations that would warrant additional scrutiny and outside review. Basically, they explain exactly how and when such innovations become different enough to be viewed as a form of experimentation. This signifies a point at which clinical practice goes beyond the existing standard of care, and outside of the realm of tried-and-true treatments [3]. The guidelines that were firmly founded on earlier work [2], stipulate the following:
An “innovation” is a new or modified surgical procedure that differs from currently accepted local practice, the outcomes of which have not been described, and which may entail risk to the patient. Many innovations are used on an ad-hoc basis as dictated by the clinical situation. Some innovations, however, may be developed in a more systematic fashion and may ultimately meet the criteria for human subject research, although they do not meet the criteria at the time they are performed. Example: A surgeon decides to perform Natural Orifice Translumenal Endoscopic Surgery, removing an appendix via a patient’s vagina [3].
In earlier work published by two authors from the same group [1], an additional definition of innovation was offered. Innovative use of a procedure included its application to a disease or diagnosis for which it had never been used before. This particular situation appears to apply to the clinical scenario we are discussing—performing prophylactic bariatric surgery for diabetes mellitus type 2.
First, let us take a step back and frame the ethics of surgical innovation in general. Innovative or experimental surgery has the potential to provide great benefit to patients who undergo new, sometimes life-saving procedures. In and of itself, surgical innovation is not an unethical thing, but because its risks are partly unknown and its benefits equally so, because of the lack of existing evidence, it is ethically contentious. Striking the right balance between beneficence and non-maleficence is challenging. The flipside of non-maleficence, in the case of surgical innovation, is that not offering the latest available therapies to a patient may constitute doing harm. Performing an older procedure that is going out of fashion because of disappointing outcomes instead of a newer, more promising technique seems harmful. Surgeons are required to stay current with the developments in their profession, and adopt techniques that are proven superior to the existing ones. The importance of this is reflected in the obligation to earn continued medical education (CME) credits and in (medico-legal) licensing procedures. Not staying up-to-date and hanging onto obsolete techniques while being wary of innovation is not considered good surgical practice. This stance was underscored by some of the responses to a survey among US surgeons [1]. One respondent wrote: “Surgeons that do not innovate should be the ones that need to be regulated!” One might conclude that the balance between harming and doing good is indeed delicate, and perhaps even ambiguous, when it comes to innovative surgery.
Even more ethically ambiguous is prophylactic innovative surgery. Bariatric surgery in and of itself is not an innovative or experimental surgical procedure. It has been performed for a number of years, studied and evaluated for its merits. What is innovative is the application discussed in this case: performing bariatric surgery for a new diagnosis, essentially a possible future diagnosis, one that does not exist yet but is a possible occurrence, though by no means a certainty, at a later point in the patient’s life. As is well established, diabetes mellitus type 2 (DM type 2) can develop over time in overweight individuals, particularly those with a family history of the disease. While it would be wise for everyone to avoid becoming obese for a wide variety of health—and other related—reasons, anyone with a family history of DM type 2 especially should avoid obesity in order to have a better chance to ward off DM type 2. This can be done by adhering to a healthy lifestyle, which includes regular exercise (as little as a 30-minute brisk walk each day) and a wholesome diet. For most people, this should be adequate to retain a healthy weight and a normal body mass index (BMI), which subsequently diminishes the chances of developing DM type 2. Some might argue that for particular individuals, such as those with a predisposition toward weight gain and a family history of obesity or those who cannot exercise regularly because of severe physical limitations, these measures may not be able to control weight. For such individuals, bariatric surgery may be viewed as an extreme but appropriate measure to ensure the lowest calorie intake possible, leading to reaching a healthy weight.
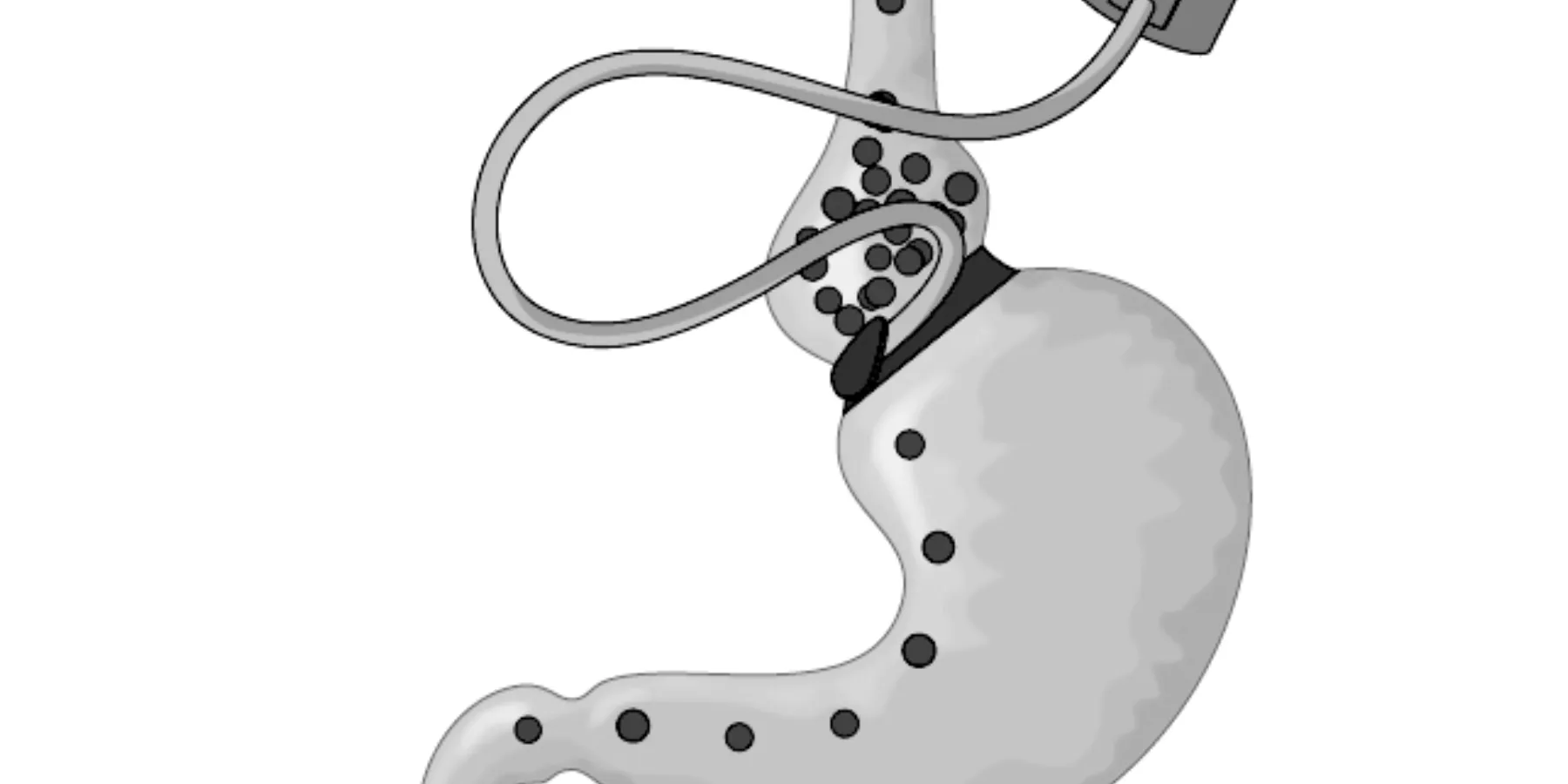
Bariatric surgery significantly minimizes the size of the patient’s stomach, thereby allowing only small amounts of food and drink to be taken in at one time. This makes it difficult for a person to eat large amounts of food throughout the day and, hence, reduces caloric intake, resulting in weight loss. But bariatric surgery is by no means a guarantee for continued weight loss or, better said, maintaining a healthy weight. Although the stomach may be small, patients who consume calorie-dense food and drinks and do not exercise enough will gain weight. We have only to look at the tabloids and see the celebrities who had their stomachs stapled, lost huge amounts of weight, and then gained some, sometimes a lot, of it back within years. This means that even after bariatric surgery, patients must be counseled about a lifelong healthy diet, learning which foods and drinks to avoid reversing the effects of the operation. Bariatric surgery in and of itself is no long-term guarantee for maintaining low weight and thereby indirectly minimizing the chances of developing DM type 2. Significant lifestyle changes would still be necessary to achieve that.
To offer this surgery to someone for the purpose of avoiding the potential long-term effects of her obesity, given this knowledge and the fact that this is a major surgical procedure with significant risk and morbidity, is not good surgical practice. With this in mind, I think it is clear that using bariatric surgery prophylactically in this case is not ethical and should not be performed.
References
-
Reitsma AM, Moreno JD. Ethical regulations for innovative surgery: the last frontier? J Am Coll Surg. 2002;194(6):792-801.
- Reitsma AM, Moreno JD. The ethics of innovative surgery: US surgeons’ definitions, knowledge and attitudes. J Am Coll Surg. 2005;200(1):103-110.
- Biffl WL, Spain DA, Reitsma AM, et al. Responsible development and application of surgical innovations: a position statement of the Society of University Surgeons. J Am Coll Surg. 2008;206(3):1204-1209.
-
Reitsma AM. Evidence-based surgery: a growing need for a limited enterprise. Virtual Mentor. 2004;6(10). http://virtualmentor.ama-assn.org/2004/10/oped1-0410.html. Accessed January 12, 2010.