Abstract
This article builds a case for raising occupational consciousness by critically questioning ahistorical and apolitical uses of battle language, especially when referring to infectious diseases. Words such as invasion, colonization, and resistance are particularly ethically troubling, and this article considers why the social practices our language brings about matter in health care. Dynamic relationships among humans and microbes, as well as metaphor, are considered here in historical context and through the lens of Derrida’s portmanteau hostipitality, which invites reconsideration of an infectious disease notion of host and how conceptions of hospitality have been institutionalized and commodified. This article argues that language used in infectious disease care settings should be informed by coexistence as a guiding value of clinical and ethical relevance.
I had been talking to a patient. We had found drug-resistant bacteria in her lungs, and she was understandably worried. I tried to reassure her that the bacteria were not causing any problems and didn’t need any treatment, they just happened to be there. The language I used to do this was “it’s just a colonizer.” This particular patient was Native American.
Olivia S. Kates, MD, MA
Word Choices Are Ethics Choices
The epigram reveals the ethical importance of interrogating geopolitical terminologies and analogies (eg, invasion, colonization, resistance) in how we talk about the dynamic relationships among humans, microbes, and their shared environment. Our thinking about this topic is informed and guided by our Global South-based research involvement in decolonizing global health—a subdiscipline within public health and medicine—and our recognition that colonialism and global health are inextricably linked. As Nunn and Qian pointed out, the worldwide expansion of European presence has resulted in the transmission of new diseases and demographic, ecological, and economic changes to the Global South.1 The field of infectious disease is significantly shaped by the historical origins and evolution of global health, previously known as colonial or imperial medicine (1500-1800), missionary medicine (early 1800s), tropical medicine (late 1800s) and international medicine (after 1950), and, as Cator and Borrell note, “each synonym has nuances in its goal and the period in which the term predominated.”2 Acknowledging that it is impossible to comprehensively address the complex subject of geopolitical terminologies and analogies in the field of infectious disease, our main aim is to illustrate how use of geopolitical battle language legitimizes outdated and potentially harmful colonial practices and mindsets in infectious disease. We approach and engage this topic through 2 conceptual lenses: occupational consciousness and Derrida’s deconstructionist portmanteau hostipitality.
Occupational Consciousness
We first wish to briefly speak to why language and languaging in particular matters. Swain defines languaging as “a process of making meaning and shaping knowledge and experience through language.”3 Language can be approached from the perspective of structural and generative linguistics, whereby it is conceived as “an autonomous system of science” and “a mental grammar,” whereas languaging allows for language to be viewed through a critical linguistics lens as “a series of social practices and actions.”4 Occupational consciousness, a concept coined and theorized by Ramugondo, also applies to the terminologies we use in our practices. It is defined as “ongoing awareness of the dynamics of hegemony and … [how] through what people do every day” we can either sustain or disrupt “dominant practices … with implications for personal and collective health.”5 In other words, without being critically and sensitively conscious of the ends of our daily occupations, including languaging,6,7,8,9 we may unintentionally cause or perpetuate harm, which we are ethically obliged to mitigate.10,11,12,13 For example, Cox and Fritz have highlighted that “Some commonly used language in healthcare confers petulance on patients, renders them passive, or blames them for poor outcomes”; “Such language negatively affects patient-provider relationships and is outdated”; “Research is needed to explore the impact that such language could have on patient outcomes”; and lastly, “Clinicians should consider how their language affects attitudes and change as necessary.”14
The definition of the occupational consciousness concept in terms of “dynamics of hegemony” and “dominant practices” prompts us to acknowledge and interrogate the ahistorical and apolitical use of the “battle” metaphors invasion, colonization, and resistance in languaging the dynamic relationships among humans, microbes, and their shared environments.15,16,17,18,19,20,21,22 Given that biomedicine is predominantly occupied with diagnosing and treating symptoms and diseases rather than their underlying causes,23 it seems apt to adopt a historicizing approach to understanding why geopolitical terminologies are problematic. This approach allows us to consider that the use of battle language24 may originate from what Maldonado-Torres identifies as “a ‘master morality’ of dominion and control at the heart of western modernity … [which] constitutes the centre of a warring paradigm that inspires and legitimizes racial policies, imperial projects, and wars of invasion.”25
Biomedicine Remains a Tool of Empire
It is imperative to underscore that, historically, the practice of modern medicine and its specialization, infectious disease, are deeply embedded in and held in check by colonial thinking in Western modernity23 in partnership with white supremacy. The American sociologist Barbara Katz Rothman goes so far as to suggest that biomedicine is today’s “ruling empire, colonising the planet.”23 Horton points out in the Lancet that though Rothman does not deny that biomedicine has saved lives, her concern is with the growing economic, governmental, and religious power of biomedicine in society.10 In particular, health and health care in the biomedical empire have come to mean commodified medical services, which Rothman describes as “very individualised and very professionalised.”10,23 Biomedicine is not preoccupied with understanding and advancing people-planet health but, arguably, at best with preventing death and at worst with determining who lives and who dies. The latter commitment is manifest, for example, in practices of using drugs on certain populations without their consent (eg, AZT trials conducted on HIV-positive African subjects by US physicians in 199426) and privileging and withholding treatment (eg, Tuskegee Study of Untreated Syphilis in the Negro Male from 1932 to 197227).
Keeping in mind the deep embeddedness of biomedicine in colonial thinking and practices, we now critically and ethically review the prevailing understanding in infectious disease of humans, microbes, and their dynamic relationships in a shared environment.
All Humans Are Counted, But Not Treated as Equals
In infectious disease, the thesis (ontological assumption) that underlies the dominant understanding of humans appears to be that “being human is a given for all [italics added].”28 This apolitical and ahistorical premise is supported by the ongoing tracking of our rapidly growing global population.29 Literally every human body counts as human, given the logic that the earth’s human inhabitants, currently over 8 billion,30 (are to) share the same planetary environment. Additionally, microbes do not discriminate among humans they select as hosts. However, across centuries, a political review of human history irrefutably evidences that not every body that is counted as a human also gets treated as one. Frantz Fanon languaged this disturbing historical reality in terms of a man-made division of humanity along “the racialized line of the human”: above the “Zone of Being” (superior “whiteness”) and below the “Zone of Non-Being” (inferior “blackness”).31 Fanon basically produced the antithesis that being regarded as human is not a given for all. In his doctoral research, the first author (F.K.) offers the synthesis that “Being [regarded as] human … [is] not a given but a political potentiality which manifests on a continuum of enacted harmful negations and salutogenic affirmations of our humanity.”28 Based on this decolonial, historicized perspective on humans, we problematize the use of battle and geopolitical analogies in explaining antimicrobial resistance in infectious diseases.
Bacteria-Like Ancestors of Humans
The other core concept for understanding dynamic relationships in infectious disease is microbes, or microorganisms, which are viruses, bacteria, and fungi. In the human body, the ratio of bacteria to human cells is close to 1:1.32 Most evolutionary biologists agree that bacteria-like organisms are the ancestors of humans.33 Sometimes microbes (pathogenic ones) cause sickness, but, most of the time, microorganisms (non-pathogenic ones) are in a symbiotic relationship with their human hosts.34,35,36 They have adapted to parts of the body (skin, gut, other organ systems and mucous membranes) and provide vital functions essential for human survival. Foreign microbes from the atmosphere, other people, and other sources (including biological weapons) must gain entrance to the body for infections to occur. It is at this point that battle and geopolitical terminologies are used: when microbes enter through the respiratory, gastrointestinal, urogenital tracts, or breaks in the skin surface (see Figure).
Figure. Terminologies Used in Infectious Diseases and Geopolitical Discourses
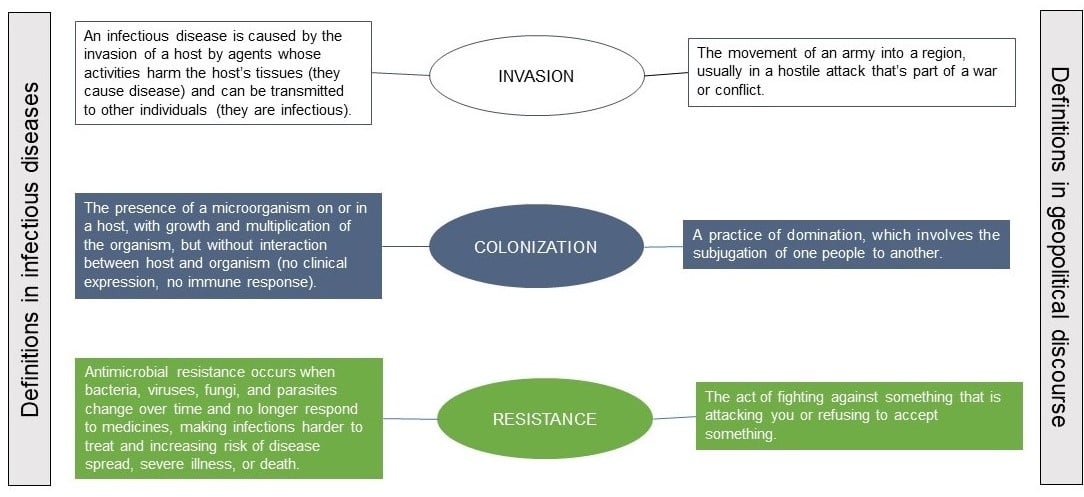
Relationship Between Humans and Microbes
In infectious disease, the relationship between humans and microbes is premised on the former being host to the latter. Given that microorganisms can either be “friendly” or “enemy-like,” it seems useful to consider the etymology of the word host. Host is derived from the Latin hospes and hospit (guest). The similar-sounding hostis means stranger or foreigner and, in classical use, enemy.37 You may also hear these Latin words’ relation to the words hostility and hostage. In infectious disease, this category of hostile or unfriendly microbes would be called pathogens.38
It seems apt to adopt a historicizing approach to understanding why geopolitical terminologies are problematic.
Other apt terms derived from host are hospitality, from the Latin hospitalitem (friendliness to guests) and hostility, from the Latin hostilis (inimical and warfare).39 Hospitality and hostility are etymologically interlinked yet seemingly contradictory concepts. Jacques Derrida, the Algerian-born French philosopher and principal exponent of deconstructionism, coined the term hostipitality, which merges the word hospitality—“being friendly or welcoming to strangers”—and its antonym hostility—“being unfriendly or hostile to strangers.”40 Hospitality, it has been argued, is always conditional and includes within it the potential for hostility, just as hostility includes within it the potential for hospitality; both imply “the possibility of the other.”41 Indeed, Derrida famously argued that hospitality is a word of “a troubled and troubling origin, a word which carries its own contradiction incorporated into it,”40 by which he refers to hostility.
As a case in point of how languaging can be harmful, we share why Derrida coined the word hostipitality. In 1997, the French government had imposed the Debre bill on immigrants and those without rights of residence, the so-called sans-papier. At the time, Derrida wrote: “I remember a bad day last year: It just about took my breath away, it sickened me when I heard the expression for the first time, barely understanding it, the expression crime of hospitality.” Derrida was reacting to the Debre Bill, which concerned a law permitting the prosecution, and even the imprisonment, of those who take in and help foreigners whose status is held to be illegal. Derrida continued: “What becomes of a country, one must wonder, what becomes of a culture, what becomes of a language when it admits of a ‘crime of hospitality,’ when hospitality can become, in the eyes of the law and its representatives, a criminal offense?”42
Taking a cue from Derrida, from an ethics perspective, are we not compelled to ask, What becomes of health care when it admits of battle analogies—when invasion, colonization, and resistance can become, in the eyes of biomedicine and its representatives, an acceptable way of talking about infections? The notion of hostipitality may serve to ignite health care practitioners’ occupational consciousness, prompting them to be mindful of and mitigate the risk of languaging, of using language in everyday practices that may cause or sustain harm done to those in need.
Coexistence: A Guiding Value of Clinical and Ethical Relevance
Although the context of Derrida’s thinking about hostipitality was worldwide mass-scale migrations,42 the term arguably does have a real bearing on antimicrobial resistance challenges, particularly for Western countries grappling with pressing migration problems: the influx of refugees and asylum seekers due to armed conflict, natural disasters, or economic hardship. The perpetual political-historical reality is that some populations of humans are hosted whereas others are treated with hostility.31 What we are exploring here is a juxtaposition of geopolitical and infectious disease analyses: on the one hand, relationships between humans in the Zone of Being and othered ones in the Zone of Non-Being and, on the other hand, between humans and invading, colonizing, and resisting microbes in their environments.
The instance that triggered the writing of this article was the generatively disruptive realization that the use of the phrase “it’s just a colonizer” may not be innocent but rather ambivalent, ethically and logically speaking. Therefore, the idea of humans hosting microbes as “strangers” may present as an alternative to languaging microbes as “invaders” who turn out to be “just colonizers.” Again, we draw from Derrida, who speaks of “unconditional” and “conditional” hospitality. Unconditional hospitality refers to the law of real hospitality as a moral attitude to others, demanding the unconditional reception of strangers; conditional laws of hospitality impose conditions by translating the unconditional law into a reciprocal right to receive and a duty to offer hospitality.40,42,43 Historical accounts suggest that at times Indigenous peoples’ first response during the earliest encounters with Europeans was consistent with Derrida’s definition of unconditional hospitality. Only when Indigenous peoples realized that these Europeans had come to take advantage of their original welcome in the most brutal ways did they start to resist. Metaphorically speaking, their “social immune system” kicked in and fought back, resisted. In other words, if we invert the infectious disease use of geopolitical terminologies in a historicized way, “the European colonizers were the ultimate pathogens” who caused mass-scale death and destruction of other cultures and civilizations.44 Grounded in Western modernity they deemed superior (Zone of Being), the conquerors, invaders, and colonizers also benignly regarded themselves as “explorers,” “Christianizers,” and “civilizers,” which in our contemporary age is languaged as bringing or spreading “development,” “democracy” and “human rights”45 to othered human populations in the south, the geopolitical peripheries of our global and local societies (Zone of Non-Being).
However, ultimately our argument is not to throw the baby out with the bathwater but to identify and pursue other guiding values of clinical and ethical relevance. The pioneering environmentalist Rachel Carson suggested that “Man is a part of nature, and his war against nature is inevitably a war against himself [italics added].”46 The latter part of this quotation resonates with Maldonado-Torres’ “‘master morality’ of dominion and control at the heart of western modernity,”25 while the former prompts us to draw from other worldviews, those that are based on the principle of coexistence.47,48 In the context of infectious disease, appreciating and tapping into humans’ capability to ethically negotiate coexistence with and discernment among friendly and enemy-like pathogens and people could indeed present as a more evolved intelligence for critical practical judgments than the ahistorical and apolitical logic and use of battle language.
Conclusion
The current way of languaging infectious disease, along with its geopolitical context, is problematic: it frames microbes alone as pathogens (nonhuman and therefore harmful) and Europeans as colonizers (human and therefore not harmful). This characterization, however, creates confusion for some, as we have not all experienced the world in the same way. Colonization constituted a dehumanization exercise across the world, and therefore using this term with reference to microbes in human bodies may create further distress for those who have been colonized, necessitating new language or terminology in infectious disease. The term coined by Derrida, hostipitality, provides the possibility of both hostility and hospitality with respect to people as well as pathogens. As such, it calls for us to become and remain occupationally conscious of biomedicine’s colonial mindset of empire and geopolitical use of language and to bring about a shift from merely preventing death to embracing unconditional and conditional coexistence.
In closing, we revisit the epigraph that opened the article, with the infectious disease practitioner saying in effect to her Native American patient: “Don’t worry, it’s just a colonizer.” One wonders what this patient would have said or done in response.
References
- Nunn N, Qian N. The Columbian exchange: a history of disease, food, and ideas. J Econ Perspect. 2010;24(2):163-188.
-
Castor D, Borrell LN. The cognitive dissonance discourse of evolving terminology from colonial medicine to global health and inaction towards equity—a Preventive Medicine golden jubilee article. Prev Med. 2022;163:107227.
-
Swain M. Languaging, agency and collaboration in advanced second language learning. In: Byrnes H, ed. Advanced Language Learning: The Contributions of Halliday and Vygotsky. Continuum; 2006:95-108.
-
Fairclough N. Critical Discourse Analysis: The Critical Study of Language. Routledge; 2013.
- Ramugondo EL. Occupational consciousness. J Occup Sci. 2015;22(4):488-501.
- Holt RIG, Speight J. The language of diabetes: the good, the bad and the ugly. Diabet Med. 2017;34(11):1495-1497.
- Chakrabarti S. What’s in a name? Compliance, adherence and concordance in chronic psychiatric disorders. World J Psychiatry. 2014;4(2):30-36.
-
Fernández L, Fossa A, Dong Z, et al. Words matter: what do patients find judgmental or offensive in outpatient notes? J Gen Intern Med. 2021;36(9):2571-2578.
- Goddu AP, O’Conor KJ, Lanzkron S, et al. Do words matter? Stigmatizing language and the transmission of bias in the medical record. J Gen Intern Med. 2018;33(5):685-691.
-
Horton R. Offline: how others see us. Lancet. 2021;398(10308):1290.
- Ledford H. Millions affected by racial bias in healthcare algorithm. Nature. 2019;574(31):609-610.
-
Ogedegbe G. Responsibility of medical journals in addressing racism in health care. JAMA Netw Open. 2020;3(8):e2016531.
-
Rivara FP, Bradley SM, Catenacci DV, et al. Structural racism and JAMA Network Open. JAMA Netw Open. 2021;4(6):e2120269.
-
Cox C, Fritz Z. Presenting complaint: use of language that disempowers patients. BMJ. 2022;377:e066720.
- Hommes F, Monzó HB, Ferrand RA, et al. The words we choose matter: recognising the importance of language in decolonising global health. Lancet Glob Health. 2021;9(7):e897-e898.
- Mendelson M, Balasegaram M, Jinks T, Pulcini C, Sharland M. Antibiotic resistance has a language problem. Nature. 2017;545(7652):23-25.
- Kamenshchikova E, Wolffs P, Hoebe C, Penders J, Horstman K. Metaphors of foreign strangers: antimicrobial resistance in biomedical discourses. Sci Cult. 2023;32(2):294-314.
- Hodgkin P. Medicine is war: and other medical metaphors. Br Med J (Clin Res Ed). 1985;291(6511):1820-1821.
-
Institute of Medicine. Ending the War Metaphor: The Changing Agenda for Unravelling the Host-Microbe Relationship: Workshop Summary. National Academies Press; 2006.
-
Sontag S. AIDS and Its Metaphors. Farrar, Straus & Giroux; 1989.
-
Lakoff G, Johnson M. Metaphors We Live By. University of Chicago Press; 1980.
-
Crimp D. AIDS: Cultural Analysis/Cultural Activism. MIT Press; 1988.
-
Rothman BK. The Biomedical Empire: Lessons Learned From the COVID-19 Pandemic. Stanford University Press; 2021.
-
Davenport D, Lloyd G. How Public Policy Became War. Hoover Institution Press; 2019.
-
Maldonado-Torres N. Against War: Views From the Underside of Modernity. Duke University Press; 2008.
- Lurie P, Wolfe SM. Unethical trials of interventions to reduce perinatal transmission of the human immunodeficiency virus in developing countries. N Engl J Med. 1997;337(12):853-856.
- Brawley OW. The study of untreated syphilis in the Negro male. Int J Radiat Oncol Biol Phys. 1998;40(1):5-8.
-
Kronenberg FCW. Everyday Enactments of Humanity Affirmations in Post 1994 Apartheid South Africa: A Phronetic Case Study of Being Human as Occupation and Health. Dissertation. University of Cape Town; 2018. Accessed June 21, 2023. https://open.uct.ac.za/server/api/core/bitstreams/9a183673-9e26-44ed-8538-b6130dac37bb/content
-
Info. Worldometer. Accessed November 1, 2023. https://www.worldometers.info/
-
Day of eight billion: 15 November 2022. United Nations. Accessed June 21, 2023. https://www.un.org/en/dayof8billion
-
Fanon F. Black Skin, White Masks. Grove Press; 1952.
- Sender R, Fuchs S, Milo R. Are we really vastly outnumbered? Revisiting the ratio of bacterial to host cells in humans. Cell. 2016;164(3):337-340.
-
Zimmer C. From bacteria to us: what went right when humans started to evolve? New York Times. January 3, 2006. Accessed June 21, 2023. https://www.nytimes.com/2006/01/03/science/from-bacteria-to-us-what-went-right-when-humans-started-to-evolve.html
-
Afzaal M, Saeed F, Shah YA, et al. Human gut microbiota in health and disease: unveiling the relationship. Front Microbiol. 2022;13:999001.
- Belkaid Y, Harrison OJ. Homeostatic immunity and the microbiota. Immunity. 2017;46(4):562-576.
- O’Callaghan D, Stebbins CE. Host-microbe interactions: bacteria. Curr Opin Microbiol. 2010;13(1):1-3.
-
Host. Online Etymology Dictionary. Accessed June 21, 2023. https://www.etymonline.com/word/host
-
Alberts B, Johnson A, Lewis J, et al. Introduction to Pathogens. Molecular Biology of the Cell. 4th ed. Garland Science; 2002.
-
Berg ML, Fiddian-Qasmiyeh E, eds. Hospitality and hostility towards migrants: global perspectives. Migr Soc. 2018;(1, theme issue):1-225.
- Derrida J. Hostipitality. Angelaki. 2000;5(3):3-18.
-
Selwyn T. An anthropology of hospitality. In: Lashley C, Morrison A, eds. In Search of Hospitality: Theoretical Perspectives and Debates. Routledge; 2011:18-37.
-
Kakoliris G. Jacques Derrida on the ethics of hospitality. In: Imafidon E, ed. The Ethics of Subjectivity: Perspectives Since the Dawn of Modernity. Palgrave Macmillan; 2015:144-156.
-
Berg ML, Fiddian-Qasmiyeh E. Introduction to the issue: encountering hospitality and hostility. Migr Soc. 2018;1(1):1-6.
- Ehrenpreis JE, Ehrenpreis ED. A historical perspective of healthcare disparity and infectious disease in the Native American population. Am J Med Sci. 2022;363(4):288-294.
-
Grosfoguel R. Decolonizing post-colonial studies and paradigms of political-economy: transmodernity, decolonial thinking, and global coloniality. Transmodernity. 2011;1(1):T411000004. Accessed June 21, 2023. http://escholarship.org/uc/item/21k6t3fq
-
The story of Silent Spring. Natural Resources Defense Council. August 13, 2015. Accessed December 8, 2023. https://www.nrdc.org/stories/story-silent-spring
-
Sousa Santos B. Epistemologies of the South: Justice Against Epistemicide. Routledge; 2014.
-
du Plessis G. Microbial Geopolitics: Living With Danger and the Future of Security. Dissertation. University of Hawaii; 2017. Accessed June 21, 2023. https://core.ac.uk/download/pdf/211329168.pdf