Third Parties in the Clinical Encounter
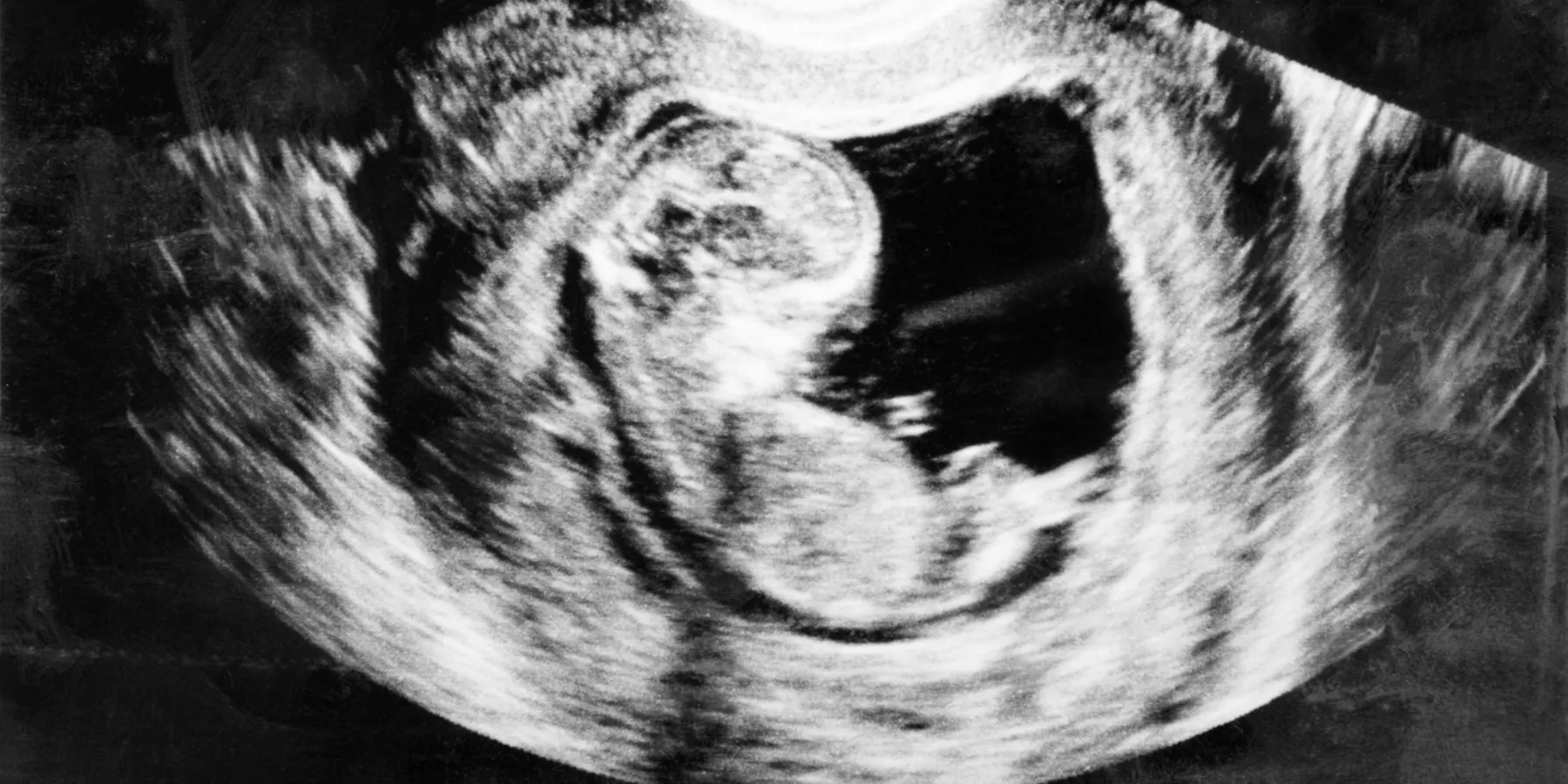
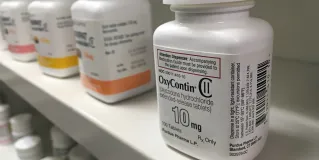
Medical licensure laws and legal informed consent requirements protect patient safety, promote shared decision making, and foster public trust in the profession. In the view of April contributors, however, other types of regulation are more troubling. These include mandated actions—e.g., making a woman view an ultrasound before an abortion and reporting possible child neglect—and prohibited actions—e.g., the “gag” on discussing gun safety with parents. Third-party activities that restrict access to certain drugs or function to maintain high drug prices also interfere with ideal standards of clinical patient care.